Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brian Wu PhD. MD Candidate, Keck School of Medicine, Los Angeles, USA; Chief Editor: Dr Amanda Oakley, Dermatologist, Hamilton, New Zealand, September 2015.
Common variable immunodeficiency is one of the more common forms of primary immunodeficiency disorder and is also called common variable hypogammaglobulinemia. Common variable immunodeficiency leads to immune system impairment and to increased vulnerability to secondary infections.
The exact cause of most cases of common variable immunodeficiency is only incompletely understood. What is known is that:
Common variable immunodeficiency is inherited most frequently in an autosomal recessive pattern and, much more rarely, in an autosomal dominant pattern. Family history is absent in 90% of patients.
Common signs and symptoms of common variable immunodeficiency include:
Patients with common variable immunodeficiency cannot be protected from infectious diseases through vaccination since they cannot mount an antibody response.
Common variable immunodeficiency may cause skin disease. The most common cutaneous manifestations of common variable immunodeficiency are:
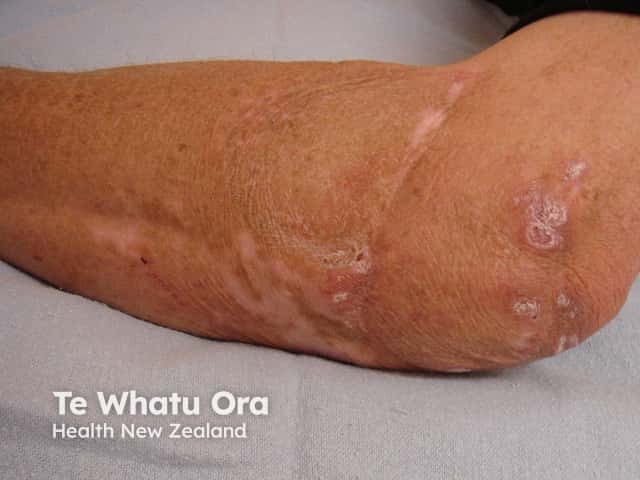
Granulomas in a patient with common variable immunodeficiency
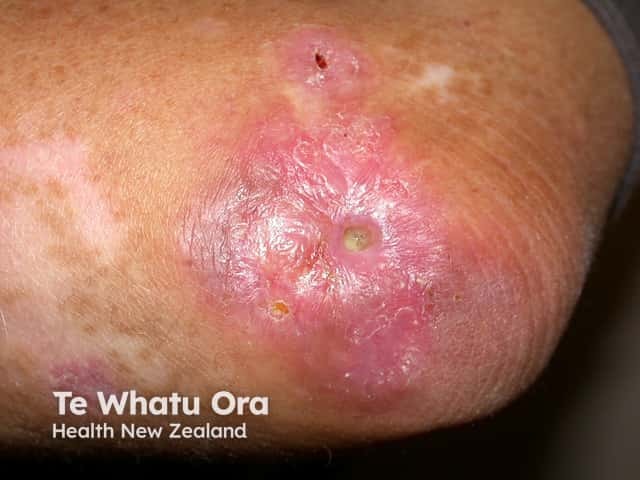
Granulomas in a patient with common variable immunodeficiency
Common variable immunodeficiency may be suspected in a patient presenting with a history of recurrent respiratory infections. The diagnosis is confirmed by measuring B-cell counts and immunoglobulin levels.
Skin lesions often require biopsy for precise diagnosis. Granulomas often resemble granuloma annulare or sarcoidosis histologically, although they are clinically distinctive.
Antibiotics are used to treat secondary bacterial infections.
Common variable immunodeficiency is generally treated by immunoglobulin replacement therapy administered by slow intravenous injection (monthly), intramuscularly or subcutaneously (weekly). Brands available in New Zealand are listed here. They are made from human plasma.
Adverse reactions have been estimated to occur within 6 hours in 2–25% of immunoglobulin infusions and are usually mild. They include malaise, headache, fever, urticaria, itch, nausea, abdominal pain, hypertension and hypotension. Headache may persist for several days after infusion. Rare severe reactions are reported to include tightening of the throat, anaphylaxis and seizures.
Persistent pain, bruising, swelling and erythema may occur at the site of subcutaneous immunoglobulin.
Delayed systemic adverse reactions are uncommon but may be serious.
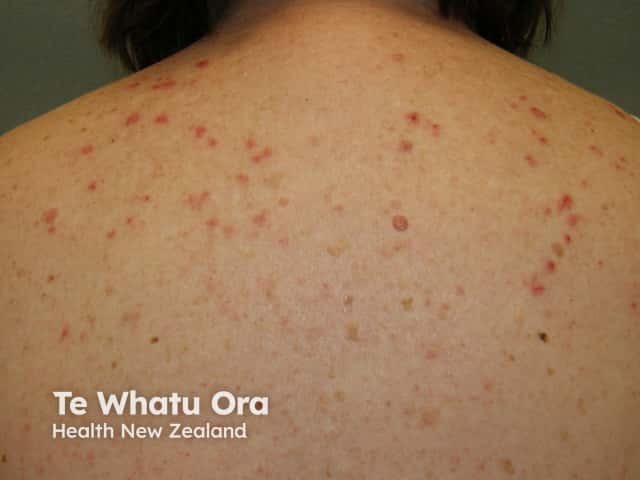
Lichenoid reaction
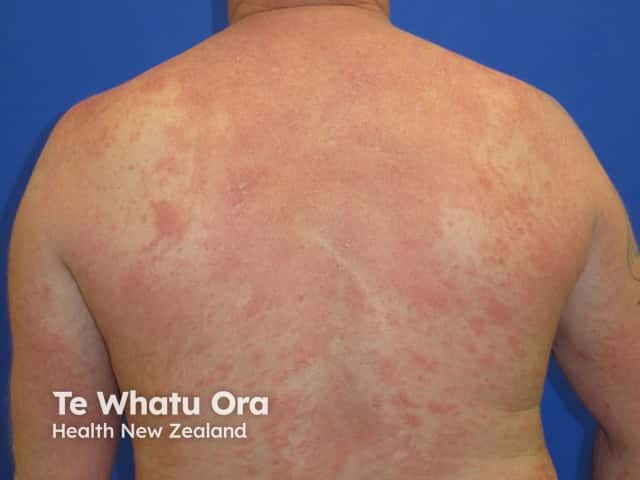
Dermatitis
Patients with granulomas and autoimmune reactions may be treated with immunosuppressive agents (corticosteroids, ciclosporin, cyclophosphamide) and anti-TNFα biologic agents.