Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Olivia Egan, Medical Student, University of Sydney, Sydney, NSW, Australia. DermNet Technical Editor: Elaine Mary Luther, Medical Student, Ross University School of Medicine, Barbados. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. February 2020.
Introduction
Demographics
Causes
Clinical features
Diagnosis
Differential diagnoses
Treatment
Outcome
Keratosis pilaris atrophicans faciei is an uncommon form of keratosis pilaris with scar-like follicular depressions and loss of hair particularly in the eyebrows [1]. This results in atrophy and permanent loss of hair in the affected areas.
Keratosis pilaris is also called ulerythema ophryogenes. Ulerythema means ‘scar with redness’, and 'ophryo' refers to the eyebrow.
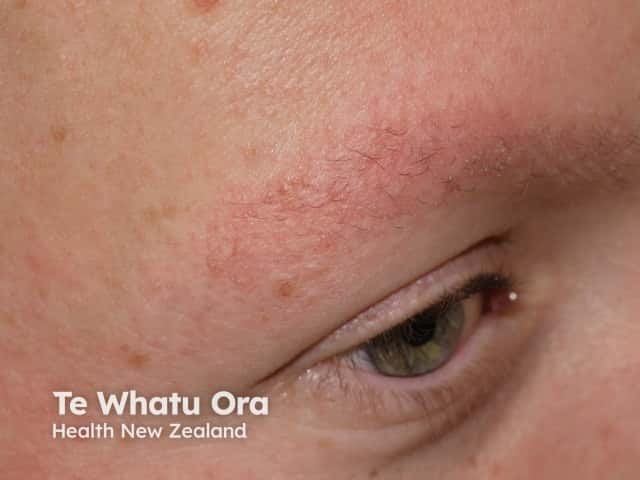
Keratosis pilaris
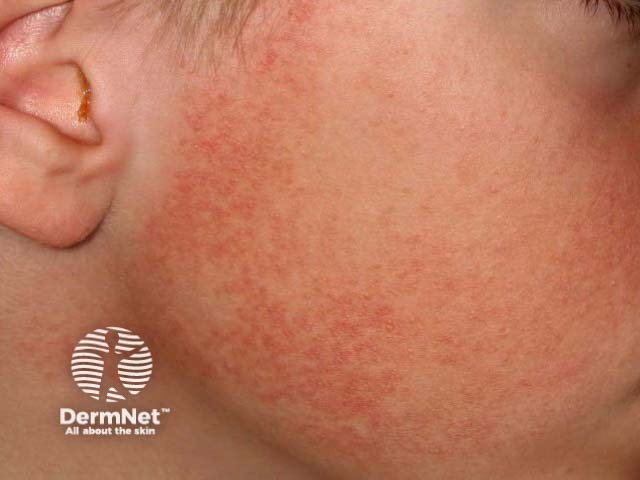
Keratosis pilaris faciei atrophicans
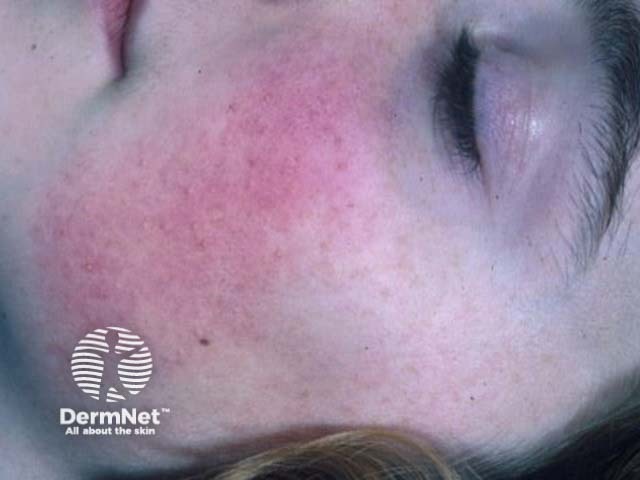
Keratosis pilaris faciei atrophicans
See more images of keratosis pilaris.
Keratosis pilaris atrophicans faciei usually occurs sporadically; however, autosomal dominant and autosomal recessive inheritance have been described [1,2,3]. It first appears in infancy, and is mainly diagnosed in children and adolescents.
Keratosis pilaris atrophicans faciei is caused by abnormal keratinisation of the follicular infundibulum. Scale fills the follicle and obstructs the hair shaft resulting in inflammation. Over time, chronic inflammation results in atrophy and alopecia [1].
Some cases of keratosis pilaris are due to an autosomal recessive mutation in the desmoglein 4 (DSG4) gene [3]. The rare association of keratosis pilaris atrophicans faciei with some congenital syndromes also suggests that chromosome arm 18p might contain genes for follicular keratinisation and be involved in disease pathogenesis [4].
Keratosis pilaris atrophicans faciei is characterised by facial inflammatory keratotic papules.
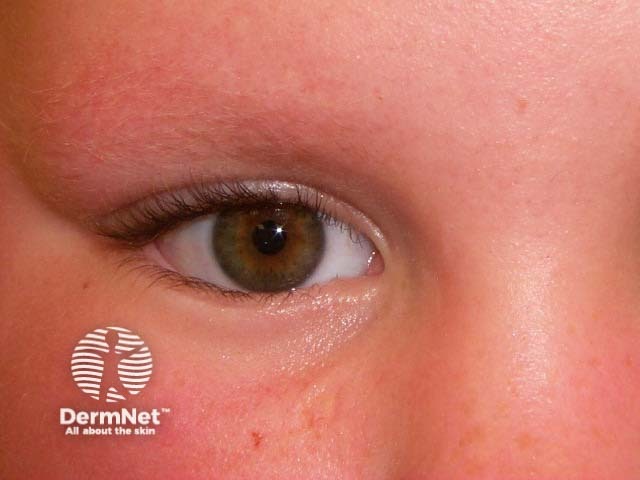
Keratosis pilaris atrophicans faciei
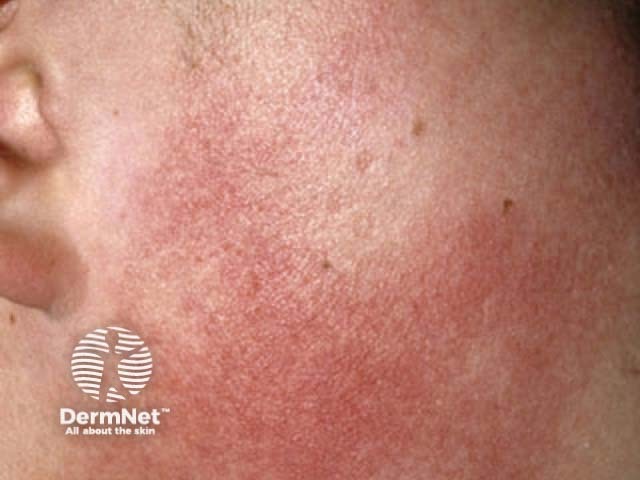
Keratosis pilaris atrophicans faciei
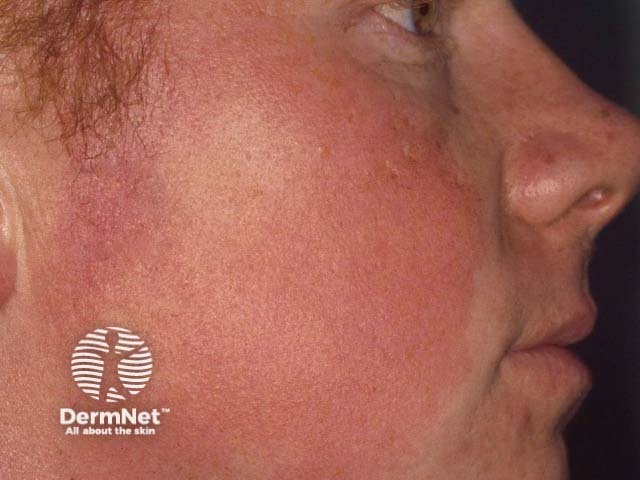
Keratosis pilaris atrophicans faciei
Keratosis pilaris atrophicans faciei is occasionally associated with Noonan syndrome, Rubinstein-Taybi syndrome, Cornelia de Lange syndrome, and cardiofaciocutaneous syndrome [4].
Keratosis pilaris atrophicans faciei is diagnosed clinically.
If a skin biopsy is performed, nonspecific histopathologic features include a widened infundibulum, plugged hair follicle, loss of hair follicle, superficial perivascular lymphocytic infiltrate, and dermal fibrosis [1,3].
Keratosis pilaris atrophicans faciei is on a spectrum with other follicular keratotic disorders, and is usually regarded as one form of keratosis pilaris atrophicans, with overlapping features commonly seen [3,5].
Keratosis pilaris rubra faciei is a variant of keratosis pilaris in which redness is prominent. It is characterised by perifollicular erythema on the forehead, cheeks, and neck without atrophy or hair loss.
Erythromelanosis follicularis faciei et colli is a variant of keratosis pilaris characterised by well-defined patches of erythema, hyperpigmentation, and follicular papules on the cheeks and neck. Most cases have been reported in Asian men [5].
Atrophoderma vermiculatum is a variant of keratosis pilaris atrophicans with prominent follicular atrophy resulting in a honeycombed pattern on the cheeks developing in childhood [3,5].
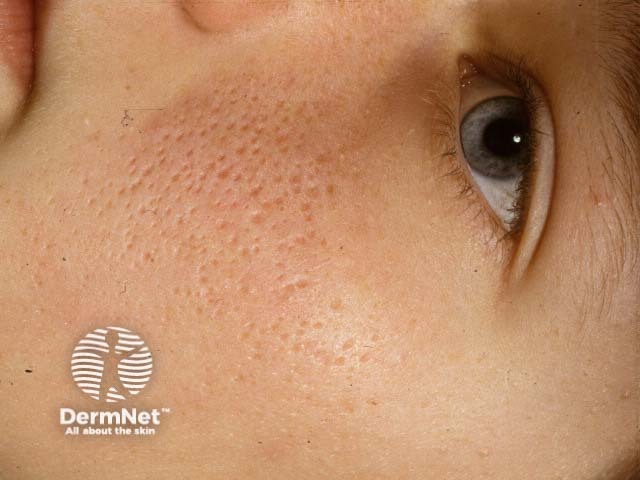
Keratosis pilaris atrophicans faciei
Keratosis follicularis spinulosa decalvans is a severe form of keratosis pilaris atrophicans with widespread follicular papules, scarring hair loss, keratoderma and keratitis [3,5].
Frontal fibrosing alopecia is a type of follicular lichen planus or lichen planopilaris in which there are facial follicular papules, loss of the lateral eyebrows, and receding frontal hairline due to scarring alopecia. It mainly affects postmenopausal women.
There is no cure for keratosis pilaris atrophicans faciei. The following can be useful to minimise the follicular scale.
Pulse dye laser or intense pulsed light (IPL) can reduce erythema temporarily but it tends to recur. Sun exposure tends to worsen redness, so sun protection is recommended.
Keratosis pilaris atrophicans faciei usually becomes less noticeable after puberty. However, atrophy with hair loss is permanent.