Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Morphoea en coup de sabre — extra information
Morphoea en coup de sabre
Author: Elaine Luther, Medical Student, Ross University School of Medicine, Barbados, West Indies. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. April 2020.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
What is morphoea en coup de sabre?
Morphoea en coup de sabre is a variant of linear morphoea (a localised form of scleroderma) restricted to the frontoparietal region (forehead). The name ‘en coup de sabre’ (the blow of a sword) derives from the characteristic scar that indents the skin of the scalp and the underlying bone. Morphoea en coup de sabre also can cut into the brain, causing neurological abnormalities and vision problems.
Morphoea en coup de sabre is also known as frontoparietal linear morphoea (American spelling morphea), linear morphoea en coup de sabre, or just 'en coup de sabre'.
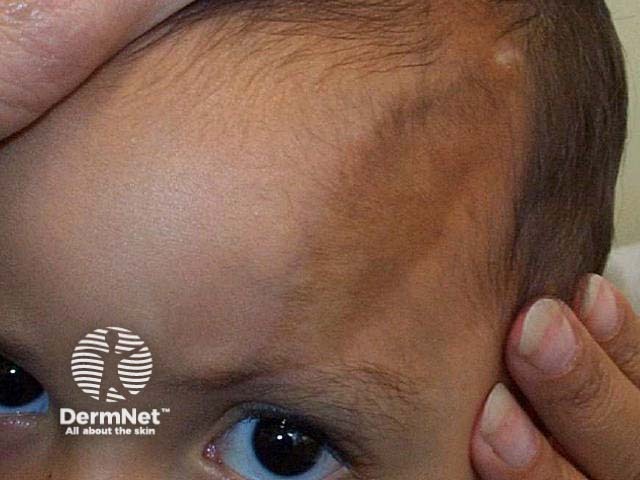
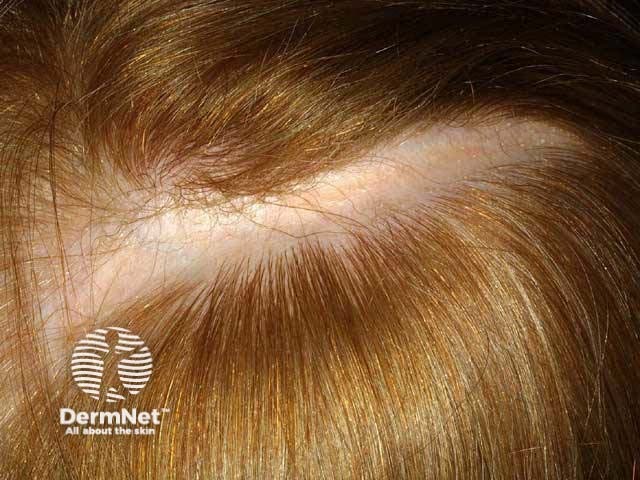
Linear cicatricial alopecia in morphoea en coup de sabre
Who gets morphoea en coup de sabre?
Morphoea en coup de sabre mostly occurs in children (67%), with a slight predominance in girls (about 2:1). It usually first appears in the first two decades of life. The average age of onset was 13.6 years of age in a series of 41 patients reported from the Mayo Clinic over a 20 year period, compared to 32 patients in Wisconsin presenting at 6.9 years of age (range 1-15 years).
What causes morphoea en coup de sabre?
The exact cause of morphoea en coup de sabre is unknown. It is believed to be an autoimmune inflammatory disease. There is probably a genetic predisposition, although the specific genetic factors are unknown. The trigger initiating the inflammation is usually unknown, but has been reported to include trauma, radiotherapy, and herpes zoster ophthalmicus. The resulting inflammatory response causes the characteristic damage.
What are the clinical features of morphoea en coup de sabre?
The clinical features of morphoea en coup de sabre evolve over months to years. En coup de sabre begins with a slightly hyperpigmented or hypopigmented streak on the forehead. Other sites may also be involved including the nose, cheek, lip, and neck. Although morphoea en coup de sabre is usually unilateral, changes can affect both sides of the face. Typically the skin becomes ivory in colour with a violaceous margin. The streak becomes indurated, evolving into a scar. The underlying scalp and sometimes even the skull indent which can result in facial asymmetry. As the scar grows, it reaches past the hairline into the scalp, causing linear cicatricial alopecia.
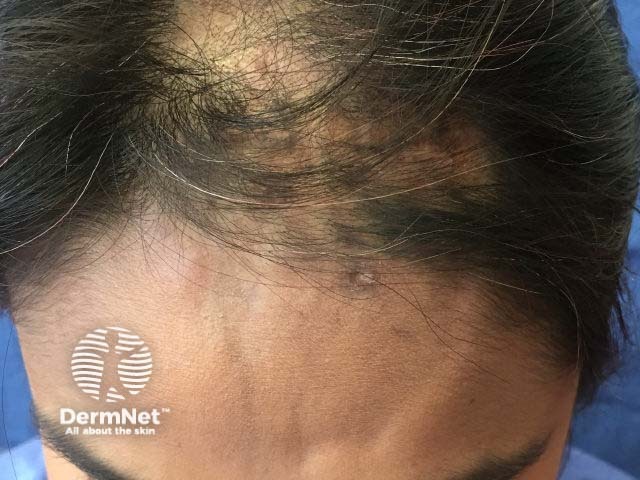
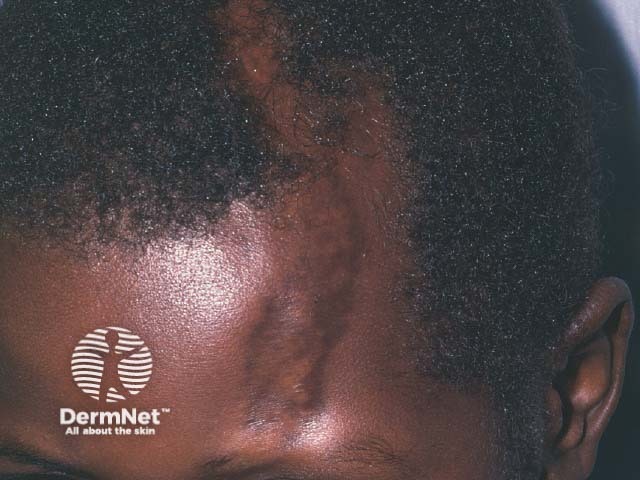
What are the complications of morphoea en coup de sabre?
The complications of morphoea en coup de sabre include:
- Hair loss
- Scalp atrophy or atrophy of the underlying bone
- Progressive hemifacial atrophy (Parry-Romberg syndrome)
- Ipsilateral eye problems (structural and visual abnormalities)
- Neurological abnormalities (eg, seizures and headaches)
- Facial deformity
- Gum, tongue, and other dental problems
- Reduced self-esteem See psychosocial factors in dermatology.
How is morphoea en coup de sabre diagnosed?
The diagnosis of morphoea en coup de sabre is usually made clinically by noting the characteristic forehead and scalp features. Dermoscopy shows thickened telangiectatic vessels due to inflammation, fibrosis, and loss of follicles.
If necessary, a skin biopsy can distinguish en coup de sabre from similar conditions. The histology shows the classical pathological features of scleroderma.
Negative tests for anti-endothelial antibodies, antinuclear antibodies, and anti-Scl-70 can rule out other connective tissue diseases.
Imaging may include ultrasound, plain X-rays, and computed tomography (CT) scans. Magnetic resonance imaging (MRI) may show skull abnormalities, focal brain atrophy, calcification, and white matter lesions.
What is the differential diagnosis for morphoea en coup de sabre?
Diagnosis can be difficult during the early phase when the morphoea is no more than a pigmented line. Other conditions confused with morphoea en coup de sabre may include:
- Traumatic injury
- A birthmark
- Birth trauma
- Bandlike melasma
- Linear cutaneous lupus erythematosus
- Linear facial lichen sclerosus.
What is the treatment for morphoea en coup de sabre?
The goal of treatment is to prevent progression of the en coup de sabre. The most commonly used treatment is a combination of methotrexate with oral corticosteroids. There are no published guidelines for treatment of morphoea en coup de sabre, and no standard of care. A wide range of other treatments have been reported in individual case reports.
Reconstructive surgery
Once morphoea en coup de sabre is burnt out, the atrophic skin and underlying structures may undergo surgical repair. Techniques may include:
- Dermal fat graft
- Implants of bone or synthetic materials
- Tissue expansion
- Surgical resection
- Skin and muscle flap.
What is the outcome for morphoea en coup de sabre?
The natural history of morphoea en coup de sabre is to progress slowly over many years, then to be self-limiting. There are three phases.
Active phase
The active phase of morphoea en coup de sabre features areas of active sclerosis with erythematous or violaceous borders, with or without expansion of the plaque. The goal of treatment during the active phase is to slow or stop progression with immunosuppressants.
Regression phase
The regression phase of morphoea en coup de sabre retains persistent sclerosis without erythema or a violaceous border. The loss of redness indicates regression.
Burnt-out phase
The burnt-out phase of morphoea en coup de sabre demonstrates no sclerosis and no erythema. The burnt-out phase signals that the course of en coup de sabre is complete, and no further damage will occur.
Bibliography
- Lauesen SR, Daugaard-Jensen J, Lauridsen EF, Kjær I. Localised scleroderma en coup de sabre affecting the skin, dentition and bone tissue within craniofacial neural crest fields. Clinical and radiographic study of six patients. Eur Arch Paediatr Dent. 2019;20(4):339–50. doi:10.1007/s40368-019-00427-7. PubMed
- Holland KE, Steffes B, Nocton JJ, Schwabe MJ, Jacobson RD, Drolet BA. Linear scleroderma en coup de sabre with associated neurologic abnormalities. Pediatrics. 2006;117(1):e132–6. doi:10.1542/peds.2005-0470. PubMed
- Tollefson MM, Witman PM. En coup de sabre morphea and Parry-Romberg syndrome: a retrospective review of 54 patients. J Am Acad Dermatol. 2007;56(2):257-63. doi:10.1016/j.jaad.2006.10.959. PubMed
- Chiu YE, Vora S, Kwon EK, Maheshwari M. A significant proportion of children with morphea en coup de sabre and Parry-Romberg syndrome have neuroimaging findings. Pediatr Dermatol. 2012;29(6):738–48. doi:10.1111/pde.12001. PubMed
- Fledelius HC, Danielsen PL, Ullman S. Ophthalmic findings in linear scleroderma manifesting as facial en coup de sabre. Eye (Lond). 2018;32(11):1688–96. doi:10.1038/s41433-018-0137-9. PubMed
- Saceda-Corralo D, Tosti A. Trichoscopic features of linear morphea on the scalp. Skin Appendage Disord. 2018;4(1):31-3. doi:10.1159/000478022. PubMed
- Taniguchi T, Asano Y, Tamaki Z, et al. Histological features of localized scleroderma 'en coup de sabre': a study of 16 cases. J Eur Acad Dermatol Venereol. 2014;28(12):1805–10. doi:10.1111/jdv.12280. PubMed
- Albuquerque JVD, Andriolo BNG, Vasconcellos MRA, Civile VT, Lyddiatt A, Trevisani VFM. Interventions for morphea. Cochrane Database Syst Rev. 2019;7(7):CD005027. doi:10.1002/14651858.CD005027.pub5. PubMed
On DermNet
Other websites
- Morphea — Medscape Dermatology
- Morphoea — The Australasian College of Dermatologists
- Morphoea — Skin Support UK
- International Scleroderma Network
- Scleroderma Foundation
- Scleroderma Research Foundation
- Morphea — Genetic and Rare Diseases Information Center (GARD)
- Morphea Facebook group
