Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Maham Ghani, Medical Student, CUNY School of Medicine, New York City, New York, United States. DermNet New Zealand Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. October 2019.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Prevention
Outcome
Paederus dermatitis is a skin irritation due to contact with certain species of the rove beetle, such as the Nairobi fly. It is also known as rove beetle rash, dermatitis linearis, spider lick, night burn, and Nairobi fly rash.
A blistering rash occurs 24–48 hours after brushing against or crushing the beetle against the skin, and can take several weeks to disappear [1,2].
At least 60,000 different species of rove beetle have been identified — the largest group of insects worldwide. These insects are of the family Staphylinidae, in the order Coleoptera (beetles) [2,3]. The beetles have narrow bodies, ranging from 0.5–1.5 cm [4]. They tend to have a shiny black head and thorax, with blue or black elytra (forewing), and an orange-red abdomen [1,4].
Rove beetles can be found in decaying vegetable and animal matter in most environments around the world, except Antarctica [4]. There are more than 1000 different species of rove beetle in New Zealand. They are more prevalent in warmer climates [5]. The beetle breeding period is during the rainy seasons [1,4].
Paederus dermatitis is due to contact with one of more than 622 paederus species of rove beetle, which have a blistering agent in their haemolymph (haemolymph is analogous to blood in vertebrates).
Outbreaks of paederus dermatitis are most commonly reported in Europe and Asia, but outbreaks have occurred in many other countries including:
The beetle is attracted to ultraviolet radiation (UVR); epidemics have been reported in warm regions with military units and hospital wards with open windows and fluorescent lights [4].

Paedarus littoralis
Paederus dermatitis is due to paederin, a toxin produced by pseudomonas bacteria in the haemolymph and released by the female paederus beetle [2,4,7]. Paederin causes a release of epidermal proteases and a loss of intercellular connection, inhibiting protein synthesis, DNA synthesis, and mitosis [2,5].
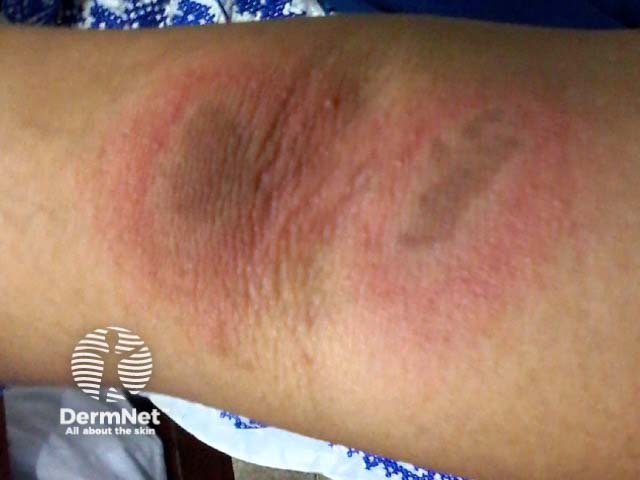
A localised streaky or linear erythema appears 24–48 hours after contact with the beetle and is typically followed by vesicles and pustules after 2–4 days [2,4,8]. Signs take a week or more to disappear [2].
The cutaneous features of paederus dermatitis include:
The primary complication of paederus dermatitis is the pain associated with the rash. Secondary complications include:
Paederus dermatitis is diagnosed clinically.
Paederus dermatitis may be confused with:
The distinguishing features of paederus dermatitis include [1]:
Once symptoms have appeared, the initial step should be to wash the affected area with soap and clean water to remove the pederin toxin.
After cleaning the area, apply a cold wet compress and a topical steroid [1].
Paederus dermatitis can be prevented by limiting the chance of exposure to the rove beetle.
It can take a few weeks for paederus dermatitis to resolve, and postinflammatory pigmentation may persist for several months [1,2].