Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Mirain Phillips, Resident Medical Officer, Waikato Hospital, Hamilton, New Zealand. DermNet Editor in Chief: Adjunct A/Prof. Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. March 2020.
Introduction Causes Clinical features Diagnosis Differential diagnoses Treatment Outcome
Subungual haemorrhage is bleeding under a nail where blood is located between the nail matrix and nail plate. Subungual haemorrhage (escape of blood) is also called subungual haematoma (collection of blood).
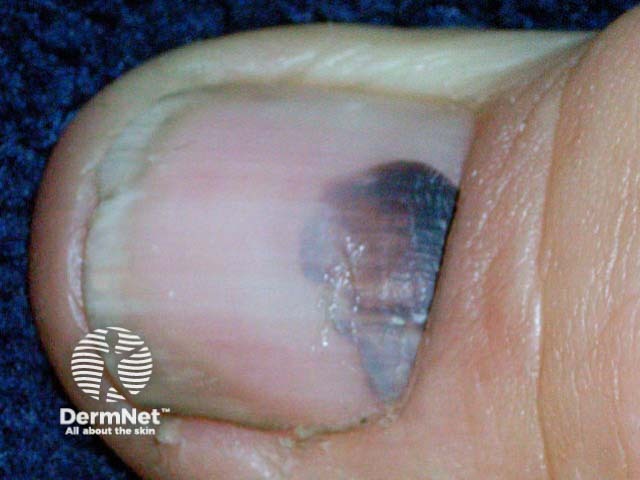
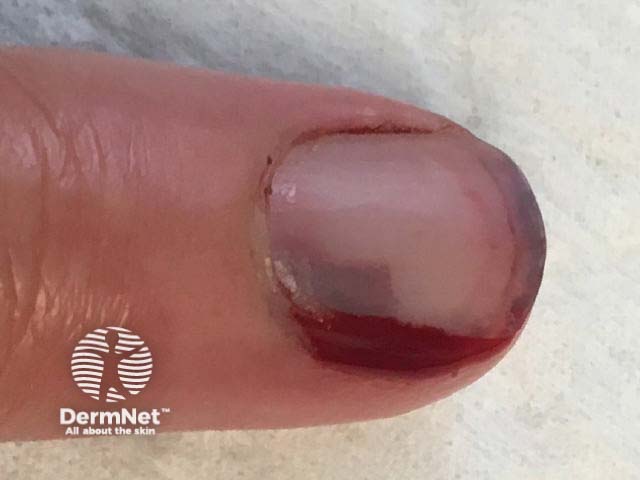
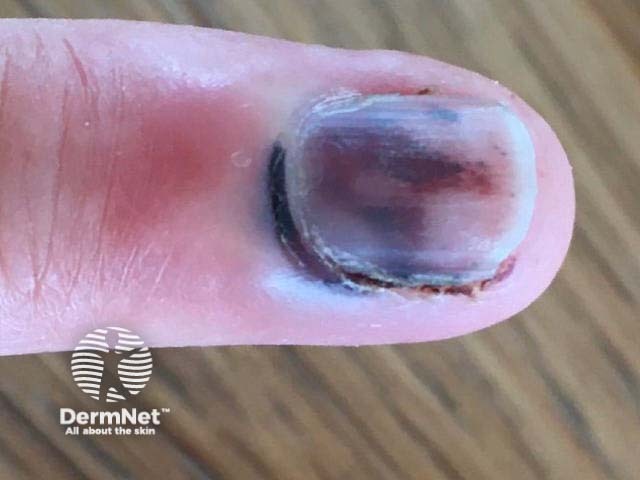
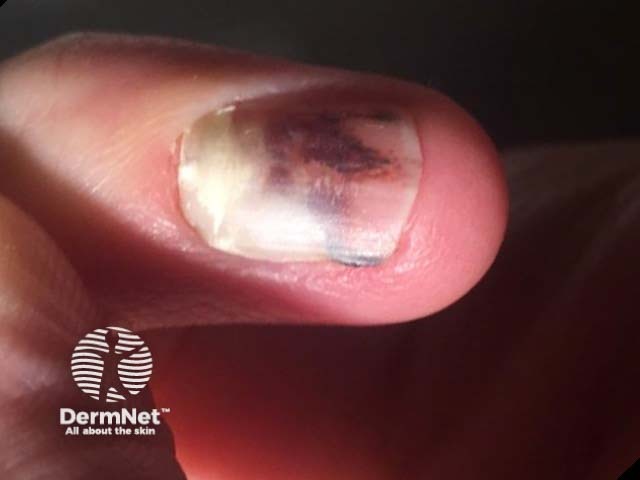
Subungual haemorrhage
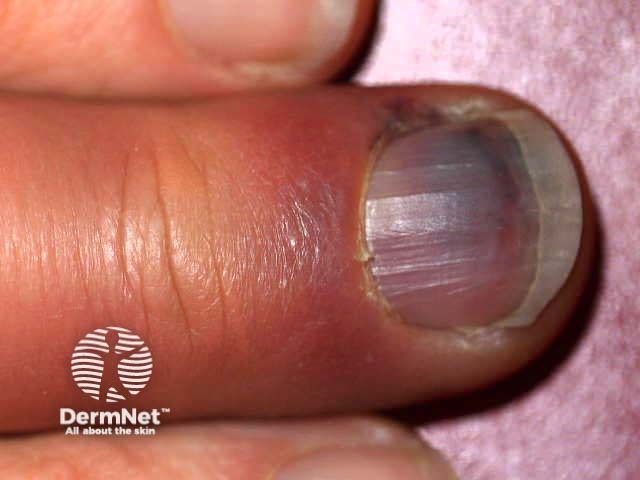
Subungual haemorrhage
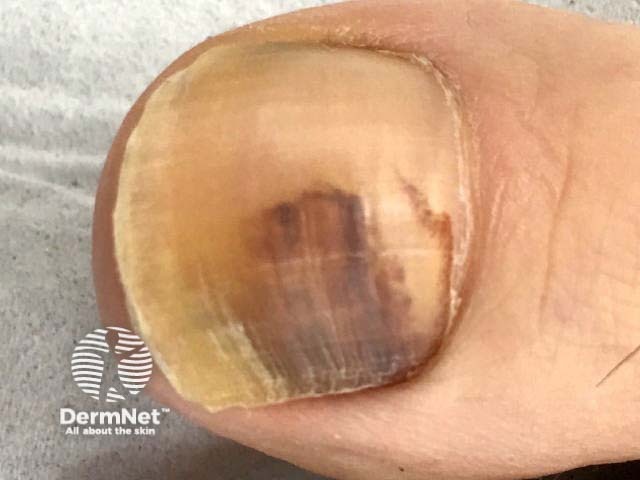
Subungual haemorrhage
See more images of subungual haemorrhage.
Subungual haemorrhage is caused by an injury to the nail [1–3].
The types of precipitating injury may include:
Rarely, subungual haemorrhage is associated with a malignant tumour of the nail unit, such as squamous cell carcinoma or melanoma [4].
Subungual haemorrhage usually presents as a single discoloured or pigmented nail, which may be painless, tender, or painful.
The patient may remember an injury leading to intense pain due to the pressure from the pooling of blood in an enclosed space and damage to surrounding tissues. Reactive inflammatory changes, such as swelling and erythema, may be observed around the nail fold shortly after the injury.
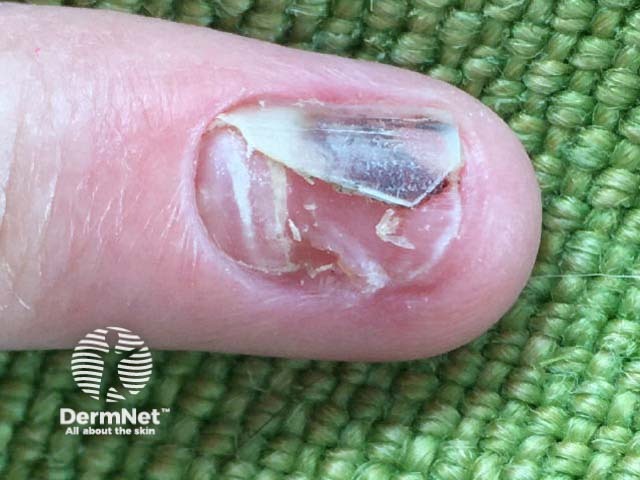
Trauma may destroy or fracture the nail plate, resulting in the nail being opaque and yellowish due to detachment from the nail bed (onycholysis). The hyponychium (the skin under the free distal edge of the nail) may appear thickened due to blood between the nail plate and the nail bed.
Subungual haemorrhage may appear reddish, purple, brown, black, or a combination of these colours. The variation in colour is related to the duration and stage of healing [2].
A clear proximal margin in the nail plate appears within a few weeks due to normal nail growth after the injury and the discoloured nail plate grows outwards.
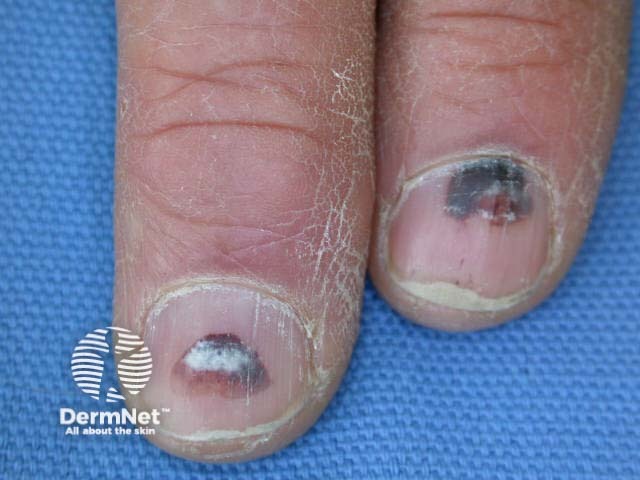
Subungual haemorrhage
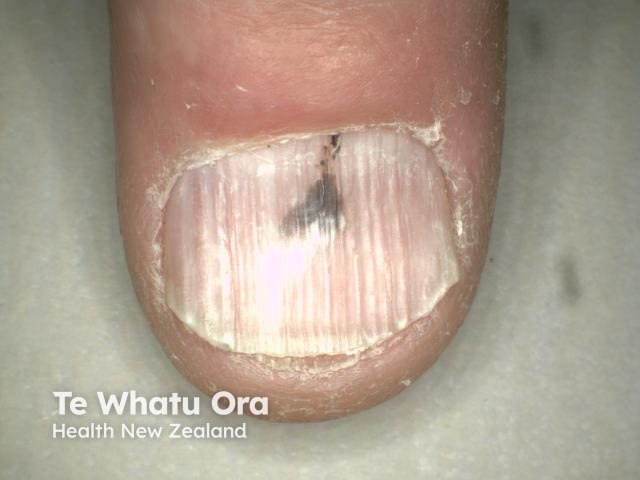
Subungual haemorrhage
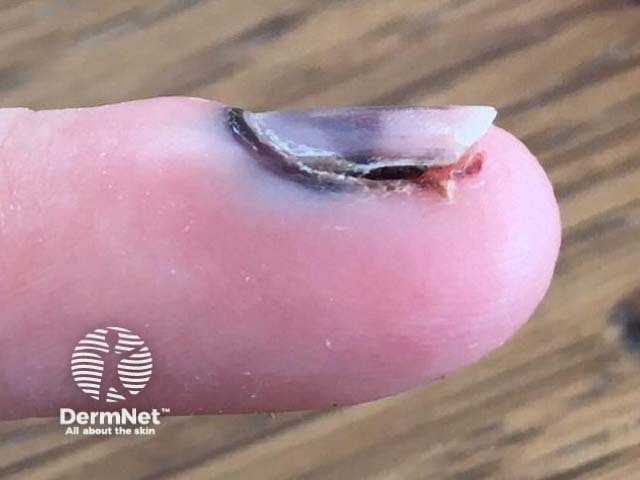
Subungual haemorrhage
Subungual haemorrhage is a clinical diagnosis supported by dermoscopy.
The dermoscopic features of subungual haemorrhage can include [2–4]:
The assessment of a pigmented nail should always evaluate the features that might be suggestive of subungual melanoma [4].
A plain X-ray should be considered for an acute injury to assess for an underlying fracture.
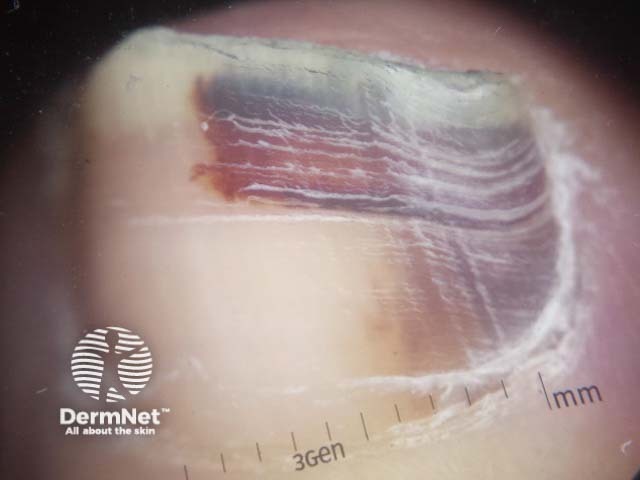
Subungual haemorrhage
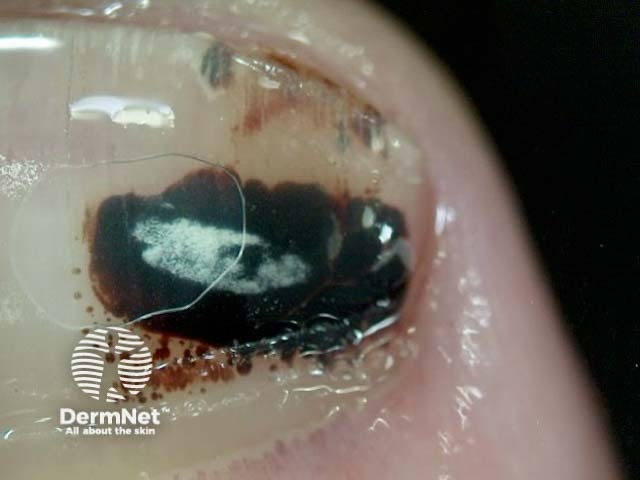
Dermoscopy of subungual haemorrhage
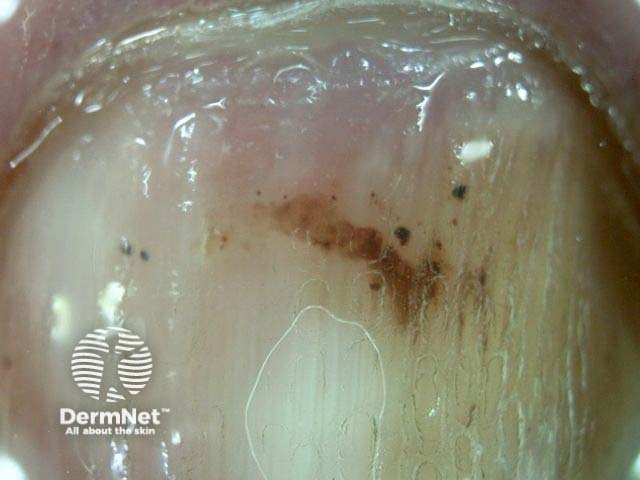
Dermoscopy of subungual haemorrhage
The differential diagnoses to consider for nail pigmentation include:
Nail unit melanoma appears as a pigmented linear or triangular band along the entire length of the nail plate. It develops the following features over time:
A normal-appearing proximal nail excludes a melanocytic lesion [5].
No treatment is required for subungual haemorrhage in the majority of cases. In the case of repetitive subungual haemorrhage, precipitating factors should be avoided, such as tight or ill-fitting shoes.
In the case of diagnostic uncertainty, the nail should be monitored using photography.
If subungual haemorrhage is acutely painful (< 48 hours after the injury), trephination can be considered [6,7]. Small holes are made in the nail plate to decompress and drain the haematoma. This can be done simply with a hot pointed metal implement [6].
Occasionally the nail plate is best removed, and the nailbed surgically repaired. A surgical opinion should be sought if there is an underlying fracture [7] or for biopsy if melanoma cannot be excluded.
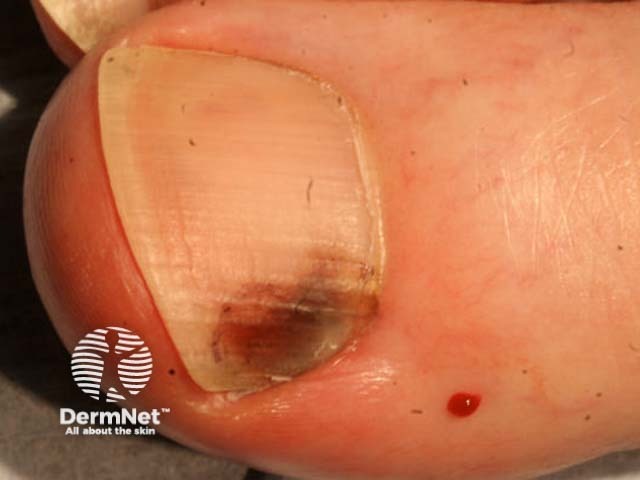
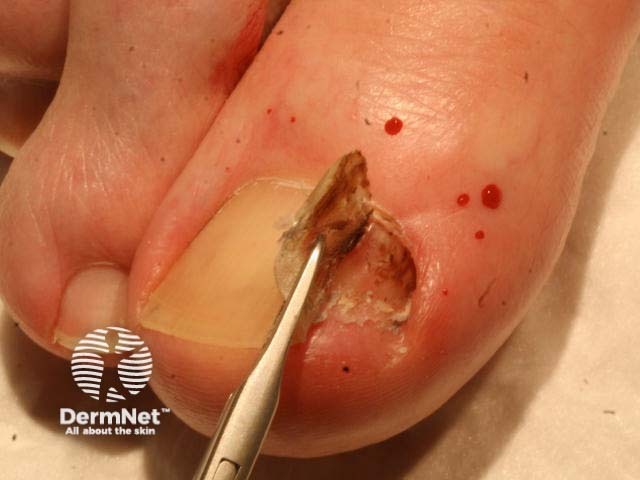
Subungual haemorrhage resolves slowly over months to years, with toenails taking longer than fingernails to recover.