Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author(s): Dr Nicole A. Seebacher, Department of Oncology, University of Oxford, UK. Copy edited by Gus Mitchell. February 2022
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Melanoma of the nail unit is usually a variant of acral lentiginous melanoma, a malignant melanoma arising from the palms of the hands and soles of the feet. Other rare forms of melanoma that may arise in the nail unit are nodular melanoma or desmoplastic melanoma.
Melanoma of the nail unit most often affects the great toe and thumbnail, accounting for 75–90% of cases. However, any nail on the finger or toe may be involved.
The term includes:
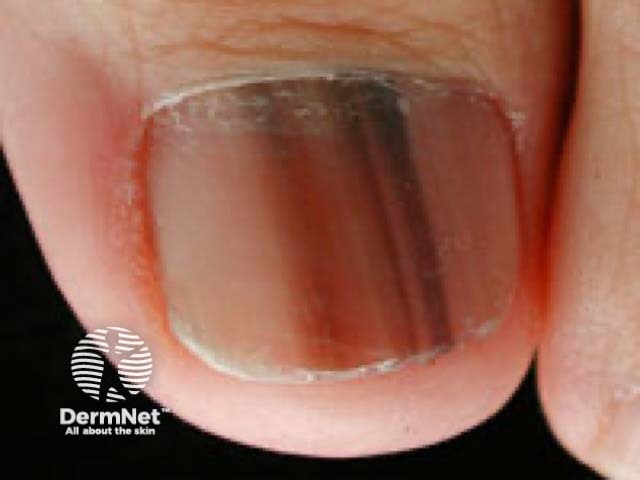
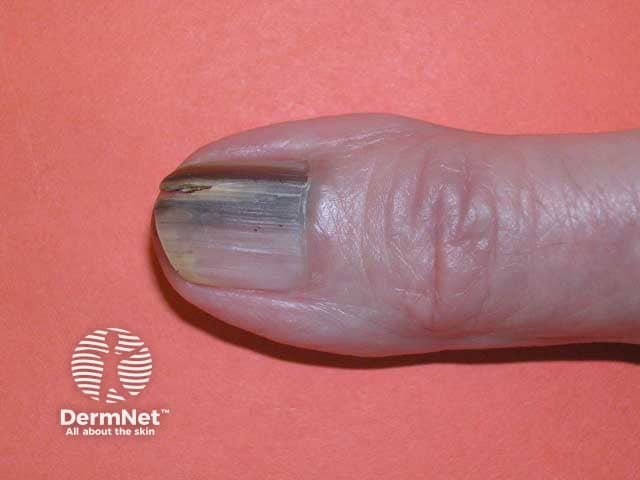
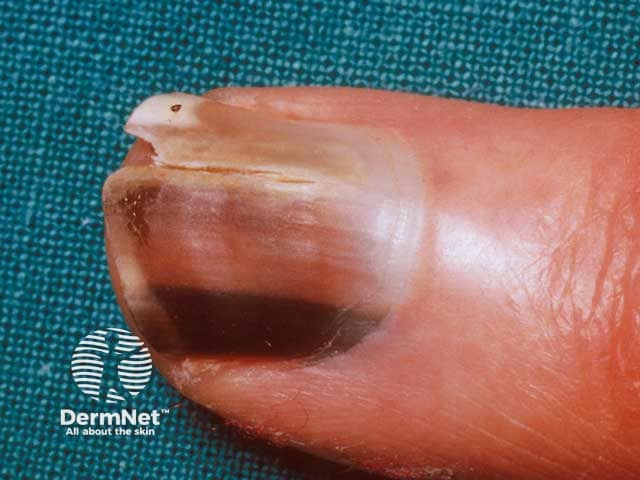
Melanoma of the nail unit is rare. While occurring equally in all racial groups, it accounts for around 0.7–3.5% of malignant melanomas in white-skinned populations and up to 75% of dark-skinned and Asian populations.
It is the most common type of melanoma diagnosed in deeply pigmented individuals, probably due to this population's low incidence of cutaneous melanoma, due to the melanin pigment protection from ultraviolet (UV) radiation.
It is most often diagnosed in the 60 to 70-year-old age group.
Melanoma management is an evolving area. For up-to-date recommendations, refer to the Australian Cancer Council Clinical practice guidelines for the diagnosis and management of melanoma.
In contrast to cutaneous melanoma, melanoma of the nail does not appear to be related to sun exposure. Melanoma of the nail unit originates from activation and proliferation of melanin producing melanocytes of the nail matrix.
Injury or trauma may be a factor, accounting for the greater incidence in the big toe and thumb (75–90% of cases).
Melanoma of the nail unit most often starts as a narrow brown to black pigmented band, visible on the length of a single nail plate (melanonychia). It is most prevalent in the nail of the thumb or big toe. It is not easy to differentiate from a benign lentigo or naevus (mole) in its early stages. However, over weeks to months, the pigment band:
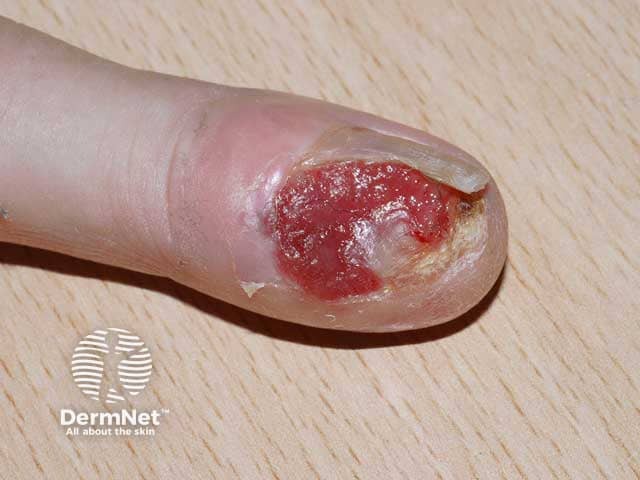
Melanoma of the nail unit
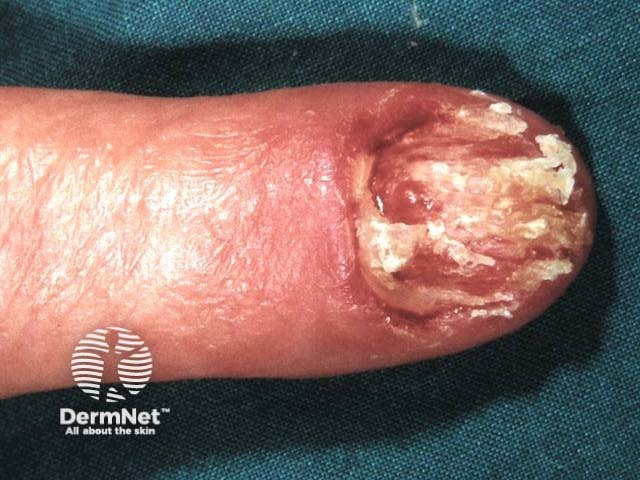
Amelanotic melanoma of the nail unit
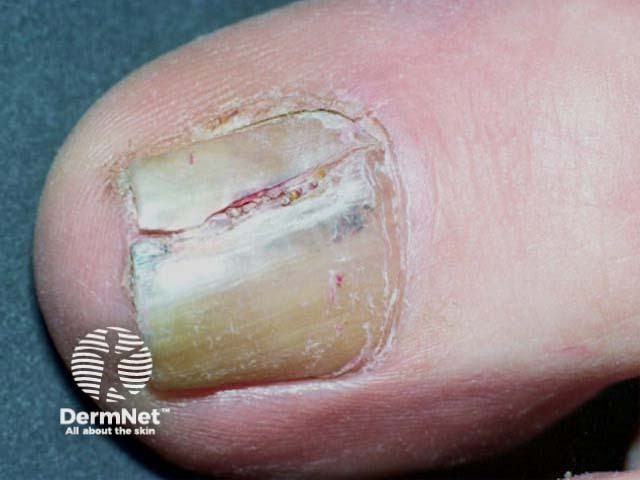
Subungual amelanotic melanoma of nail unit, toe
Melanoma of the nail unit arises in people of all skin colour and race.
It is important to note that while longitudinal melanonychia only occurs in around 1% of white-skinned individuals, it is very common in dark-skinned races, occurring in an estimated 100% of African-Americans by the age of 50 and around 20% of Asians. This may lead to misdiagnosis or delayed diagnosis of nail unit melanoma, and therefore poorer outcomes.
Melanoma of the nail unit diagnosis requires:
A thorough history to establish the onset, progression, and possible triggers. Clues to the aetiology should be sought, including medical and drug history, digital trauma, and any external exposures.
A thorough examination of all nails looking for:
Dermoscopy of the nail plate may help with an early clinical diagnosis of melanoma of the nail and help rule out lesions not requiring further examination. However, clinicians should maintain a low threshold of suspicion for performing a biopsy for histopathologic examination. Dermoscopic clues for nail unit melanoma include:
The ABCDEF mnemonic is helpful for the assessment of pigmented nail lesions:
Definitive diagnosis requires a biopsy of the nail matrix and nail bed. Any clinical features suspicious of melanoma of the nail unit warrants a biopsy.
Some experts suggest avoiding nail matrix biopsies in children where possible (unless the band is getting larger or darker).
Histopathologic examination is the gold standard for diagnosing nail melanoma. Differentiating early melanoma of the nail from benign lesions is often challenging due to similar features. The pathologist will report if the melanoma is invasive and the tissue level invaded. Common subtypes are acral lentiginous, followed by nodular and desmoplastic.
The management plan for melanoma of the nail unit will usually require a multidisciplinary melanoma team to direct further investigations and treatment. The mainstay of management of melanoma of any kind is excision.
Melanoma management is an evolving area. Please refer to your local guidelines or speak with a medical specialist for up-to-date treatment protocols.
Melanoma of the nail unit is an uncommon form of melanoma with a worse prognosis than other cutaneous melanomas. The main factor associated with the risk of metastatic melanoma and death is the thickness of the melanoma at the time of primary tumour excision. It is often diagnosed late, particularly when the toe is involved, and may have spread at the time of diagnosis.
According to the American Cancer Society, the 5-year survival rate for cutaneous melanoma varies between 15–97% depending on stage. Melanoma of the nail unit may have a worse prognosis compared with cutaneous melanoma, but this may be related to the late presentation. A meta-analysis of mortality rates for melanoma of the nail unit reported a five-year survival of 77%.