Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Kirsten Due, General Practitioner, South Australia, Australia. Reviewed by Greg Miles, former Kakadu Chief Ranger and Park Naturalist, Northern Territory, Australia. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Maria McGivern/Gus Mitchell. December 2017.
Introduction
Demographics
Cutaneous infection associated with a warmer climate
Vector-borne disease
Waterborne disease
Food-borne disease
Thermal injury
Exposure to ultraviolet radiation
Inflammatory skin diseases
Barriers to long-term projections
Climate change is a lasting alteration in patterns of weather caused by factors such as oceanic circulation, variations in solar radiation, plate tectonics, volcanic eruptions, and human factors. These factors may impact global or local temperature, humidity, rainfall, and weather extremes.
Colloquial use of the term 'climate change' specifically refers to environmental changes caused by human factors, including global warming due to the production of gases that may trap heat in the atmosphere — carbon dioxide (CO2), methane (CH4), nitrous oxide (N2O) and fluorinated gases.
Climate change has been called a 'risk–multiplier' rather than a risk–generator or risk factor, due to it worsening pre-existing climate-related health concerns.
Climate influences a wide range of systemic diseases and conditions. Heat exposure — a combination of air temperature, humidity, air movement, and heat radiation — can present an environmental hazard. The most common measures used to describe heat stress are the Wet Bulb Globe Temperature (WBGT) and Universal Thermal Climate Index (UTCI). A WBGT of 29 degrees has been shown to reduce work performance and to cause a wide variety of respiratory, cardiac and gastrointestinal diseases.
As skin is exposed to the environment, it is especially vulnerable to increased heat and humidity. In this article, we describe the effects of a warmer environment on cutaneous infections and inflammatory diseases of the skin.
Individuals at particularly high risk from hot conditions include:
Warmer conditions lead to a greater prevalence of cutaneous infections, including:
One study showed that for every 1°C rise in average temperature, the rate of hand foot and mouth disease increased by 10% and for every 1% increase in relative humidity (under 65%) the rate increased by 6.6%.
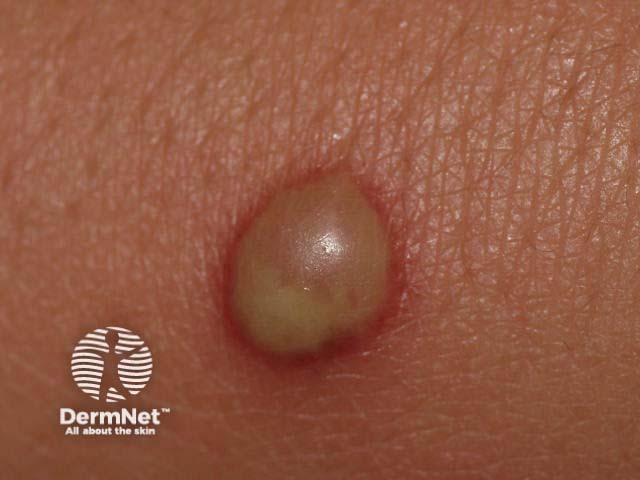
Bullous impetigo
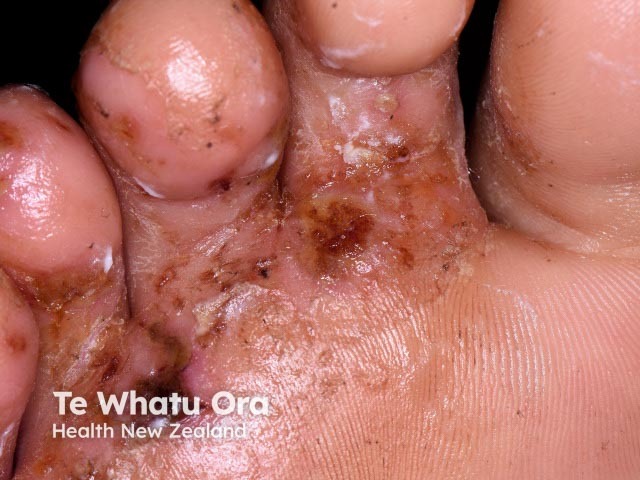
Tinea pedis
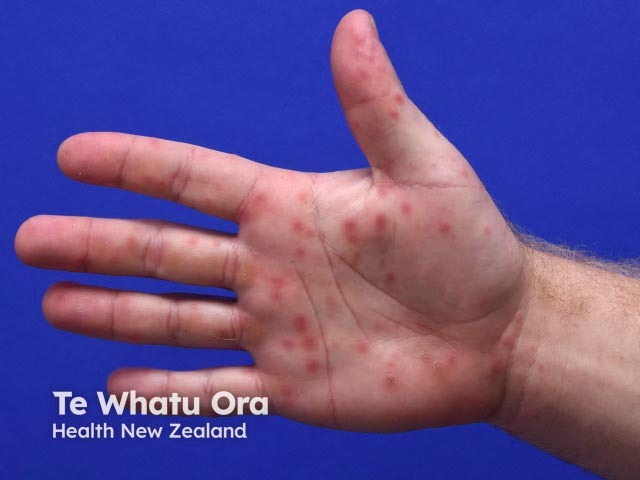
Enterovirus infection
Mosquitoes, ticks, and fleas are vectors that carry pathogenic viruses, bacteria, and protozoa, which can be transferred from one host (eg, a mosquito) to another (eg, a person or animal). Temperature plays an important role in the spread of vectors and vector-borne disease. Warmer conditions lead to faster replication of certain viruses and vectors and increased rates of transmission.
Tick borne infections include:
Mosquito-borne infections include:
The incidence of plague is likely increase with a warmer climate.
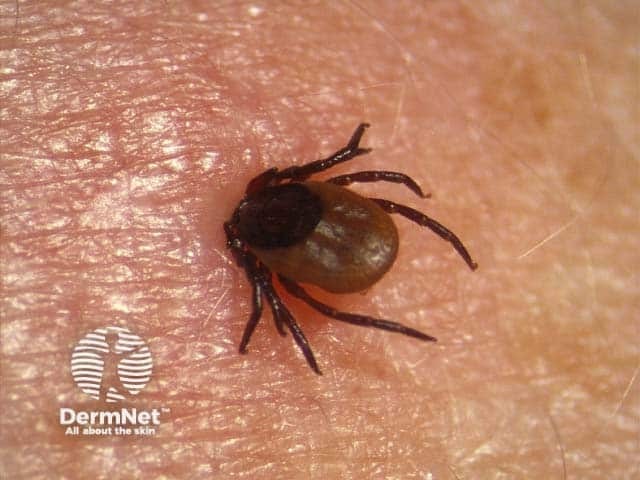
Tick bite
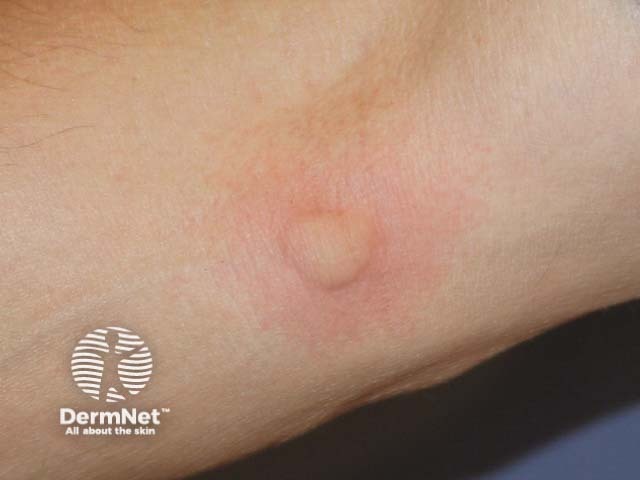
Mosquito bite
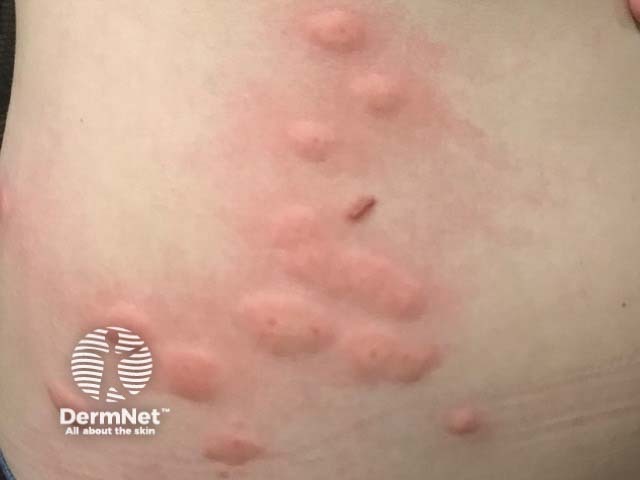
Flea bites
Heavy rainfall and flooding are predicted to increase with climate change and these often lead to outbreaks of water-borne disease. Water sources may undergo increased contamination due to flooding or become stagnant in drought. Flooding also causes disease to spread as people move en masse to seek dry ground.
Climate factors have been identified as important in outbreaks of the following water-borne diseases:
Flooding and droughts may lead to a lack of fresh water for washing and cooking, especially in resource-poor nations. The warmer waters brought about by increased temperatures can cause outbreaks of shellfish-borne disease, such as Vibrio parahaemolyticus.
Increases in temperature and humidity cause food to decay and thus increase the consumption of mycotoxins, which are metabolites of moulds. Mycotoxins may also cause disease by penetrating the skin.
Phycotoxins are potent natural toxins produced by some marine algae and cyanobacteria species. Outbreaks of phycotoxins or 'algal blooms' are often colloquially known as 'red tides' or 'green tides'. Seafood intended for human consumption can be contaminated by phycotoxins in massive quantities.

Red tide

Green tide
The warmer climate created by climate change is likely to lead to hot surfaces and increased numbers of bushfires and building fires. This is likely to result in increased thermal burns.
Measured levels of ultraviolet radiation are largely independent of heat and humidity. However, higher outdoor temperatures in previously temperate climates may result in people wearing less clothing and spending longer periods outdoors, and thus increase exposure of the skin to UV radiation.
Likely UV damage could include:
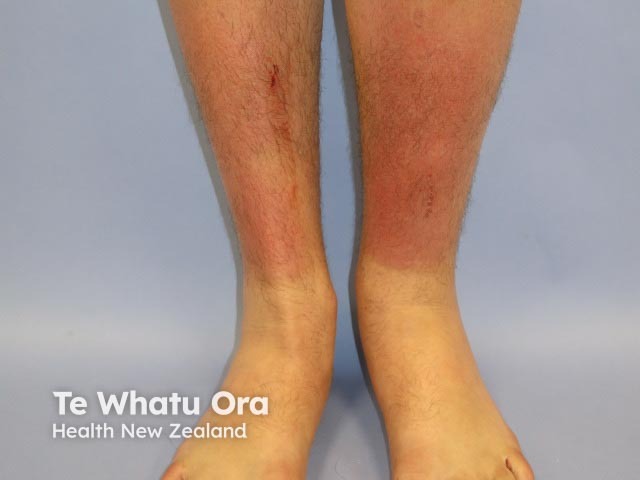
Sunburn
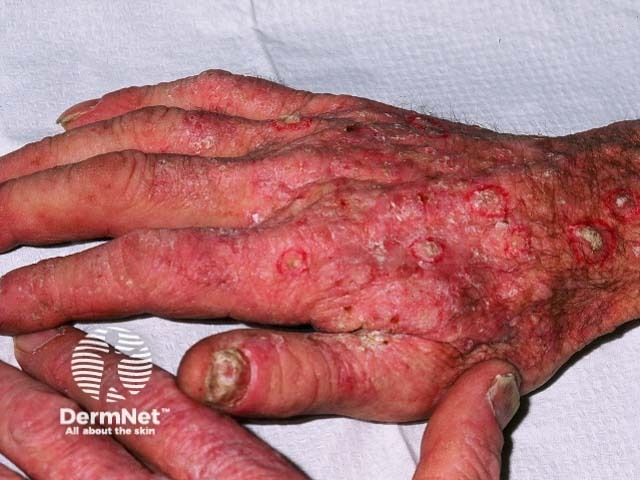
Actinic keratoses
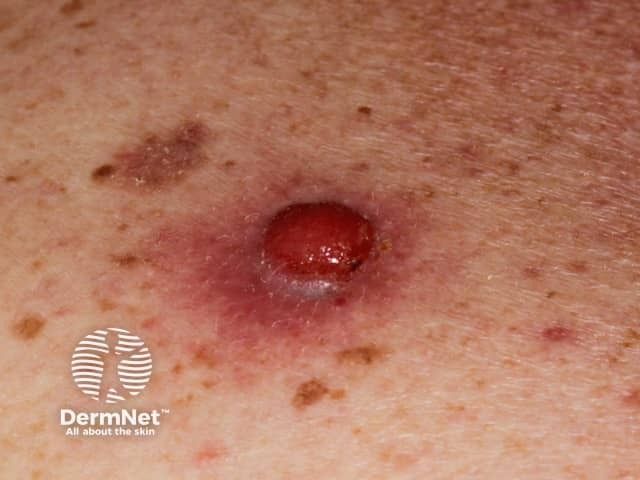
Amelanotic nodular melanoma
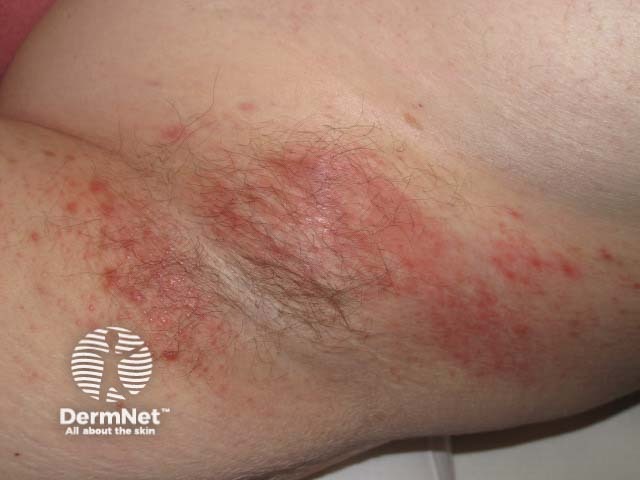
Contact dermatitis causing intertrigo
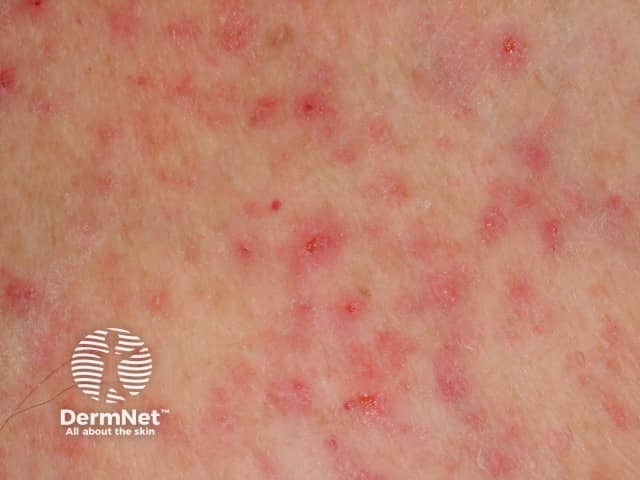
Miliaria
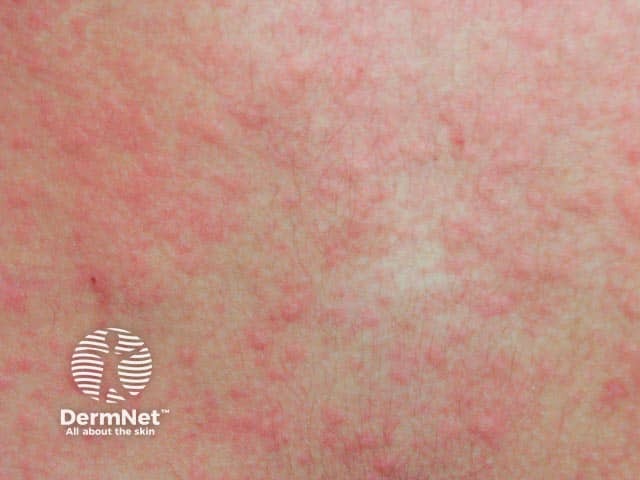
Cholinergic urticaria
Better early warning systems and prediction tools would enable the improved prevention and management of any disease epidemics likely to be associated with a changing climate — including those affecting the skin.
The current barriers to making accurate long-term epidemiological assessments and projections related to climate change include: