Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Brett Thomas, Medical Student, Kansas City University, Kansas City, MO, United States; A/Prof Rosemary L Nixon, Dermatologist, Occupational Dermatology Research and Education Centre, Skin Health Institute, Melbourne, VIC, Australia. Copy edited by Gus Mitchell. October 2020.
Introduction
Demographics
Causes and clinical features
Diagnosis
Treatment
A perianal dermatosis is a rash or skin change around the anus, between the buttocks.
Patients with a pre-existing inflammatory dermatosis may have anogenital involvement as commonly occurs with psoriasis, or the dermatosis predominantly involves the anogenital area (eg, lichen sclerosus).
Patients are often embarrassed, and it may be difficult for them to visualise and examine the area. Their quality of life can be markedly affected yet do not mention it at medical appointments.
A compromised skin barrier may predispose to a perianal dermatosis. Advanced age, faecal incontinence, immobility, hyperhidrosis, obesity, occlusion from clothing, and poor anal hygiene all contribute to skin barrier dysfunction.
Because of the effects of occlusion and maceration, scaling may not be apparent, and the skin signs may be non-specific, although there are usually clinical clues to make the diagnosis. It is important to ask about and look for skin problems elsewhere.
Perianal dermatoses often present with itch (see Itchy anus). Pruritus ani means itch around the anus with no visible skin change when used in the strict sense.
Intertrigo is an inflammatory rash in a skin fold, often due to sweat and friction, an inflammatory dermatosis, or infection.
Perianal irritant contact dermatitis can be due to:
Topical allergens that can cause perianal allergic contact dermatitis include:
Flexural psoriasis often involves the anogenital skin and natal cleft, presenting with well-demarcated symmetrical, non-scaly erythema. There will be signs of psoriasis elsewhere such as in other skin folds, scalp, or nails.
Seborrhoeic dermatitis typically affects the scalp, eyebrows, and nasolabial folds, but can involve the perineum and intergluteal fold.
Although the cubital and popliteal fossae are more commonly involved, the intergluteal fold can also be affected in atopic dermatitis.
Perianal lichen planus may be seen as an extension of vulval disease and has been reported to transform to anal squamous cell carcinoma.
Perianal lichen sclerosus shows a female predominance usually associated with vulval disease. There is an associated risk of perianal squamous cell carcinoma.
Lichen simplex commonly complicates perianal itch of various causes.
Clinical features of hidradenitis suppurativa include comedones, papules, nodules, draining sinuses, and abscesses in apocrine gland-rich skin. Fistula formation may occur in the perianal region. Genital Crohn disease can also result in perianal fistulae but lacks the other features of hidradenitis suppurativa.
Erythrasma is an infection caused by Corynebacterium minutissimum. It is often asymptomatic and causes an erythematous brown patch with maceration and slight scaling in a skin fold. Characteristic coral red fluorescence is seen with a Wood lamp.
Perianal streptococcal dermatitis is seen in children as a sharply demarcated, beefy erythematous ring around the anus with possible fissuring and exudate.
Perianal candidal intertrigo presents as soreness and irritation with bright red erythema and satellite lesions extending into the natal cleft.
Tinea cruris is usually due to T. rubrum and presents as an asymmetrical erythematous patch with a scaly, annular border in the groin. Perianal tinea is uncommon.
Pinworm infestation typically causes perianal itch at night and perianal redness or dermatitis.
Viral warts and herpes simplex virus can infect the perianal skin.
Pemphigus vulgaris often begins in the oral mucosa or the anogenital area. Benign familial pemphigus (Hailey-Hailey disease) typically involves skin folds including the skin around the anus.
Malignancies of the perianal skin may resemble a rash.
Extramammary Paget disease is an intraepithelial adenocarcinoma which can involve the perianal skin particularly in males. Lesions may appear as itchy, unilateral or asymmetric, erythematous or pigmented plaques with scaling, ulceration, or crusting.
Anal intraepithelial neoplasia (AIN) is a superficial squamous-cell carcinoma usually associated with human papillomavirus (HPV) 16 and 18, often seen in HIV/AIDS. The clinical features are non-specific, presenting as a bleeding, well-defined red, scaly erythematous rash-like plaque on the perianal skin.
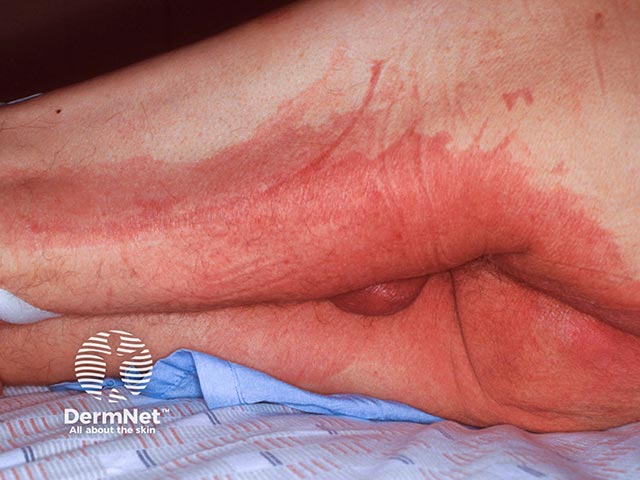
Burns resulting from overflow incontinence following co-danthrusate use

Perianal psoriasis
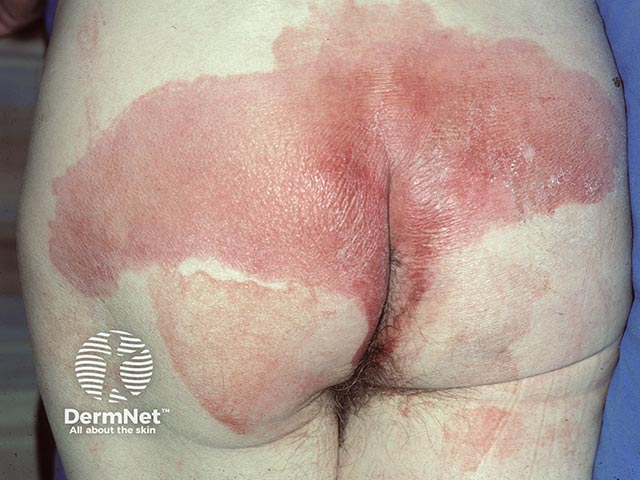
An irritant reaction due to co-danthrusate ingestion and overflow incontinence

Perianal lichen sclerosus
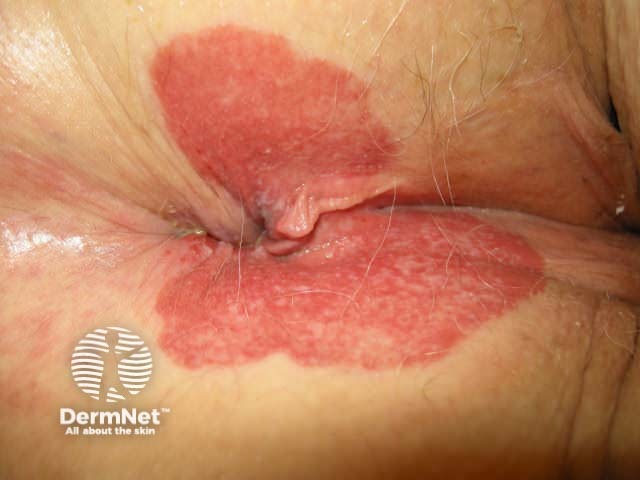
Perianal extramammary Paget disease of the skin
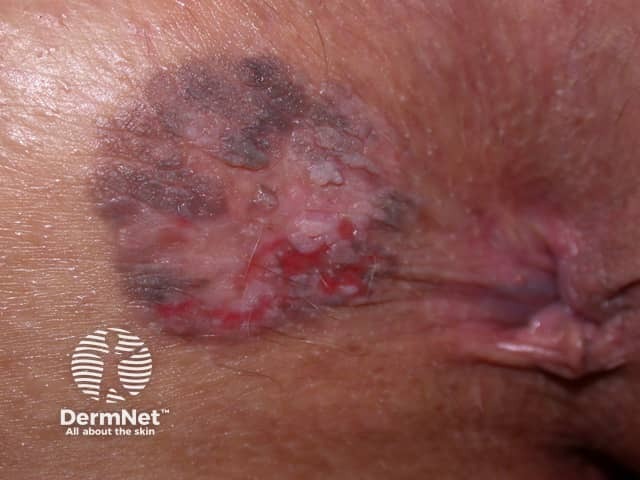
Anal intraepithelial neoplasia (AIN)
see also perianal lichen sclerosus images, genital psoriasis images, mammary and extramammary Paget disease of the skin images, anal cancer images
Perianal dermatoses are diagnosed by taking a comprehensive history, including hygiene practices, use of tight-fitting clothing, bowel habits, use of topical preparations, systemic symptoms, associated medical conditions, personal and family history of skin conditions, and response to treatment.
Following clinical examination of the perianal area and skin generally, investigations may include:
If allergic contact dermatitis is suspected, patch testing is required to identify the allergen.
Anal manometry can be performed to identify abnormalities of the anal sphincter, which may contribute to faecal incontinence and/or constipation.
Following diagnosis, it is important to relieve symptoms, restore the skin barrier, prevent recurrence, and treat the specific condition.
Specific treatments for perianal dermatoses depend on the diagnosis, but may include the following.
Topical calcineurin inhibitors
Topical local anaesthetics
Other