Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Vanessa Ngan, Staff Writer, 1997. Updated: Dr Ian Coulson, Consultant Dermatologist, East Lancashire NHS Trust, Lancashire, UK. Copy edited by Gus Mitchell. September 2021
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Itchy anus is a common complaint described as an intense itch in the perianal area between the buttocks. Perianal itch can be the result of an infestation, skin infection, inflammatory skin condition, and, rarely, a skin tumour. When there is no obvious cause for the itch it is called pruritus ani.
Itchy anus is common, affecting up to 5% of individuals at some time in their life. Men are more commonly affected than women, with a male to female ratio of 4:1. Although all age groups can be affected, the fourth to sixth decade is the most common time to develop an itchy anus.
Itchy anus can be classified as being primary (idiopathic, no obvious cause) or secondary.
Primary perianal itch is more common than secondary.
Factors contributing to an itchy anus may include:
Any common skin disease may involve the anogenital area resulting in secondary anal itching, and this may be the only site of involvement. Anal itch is unrelated to haemorrhoids or other anal conditions.
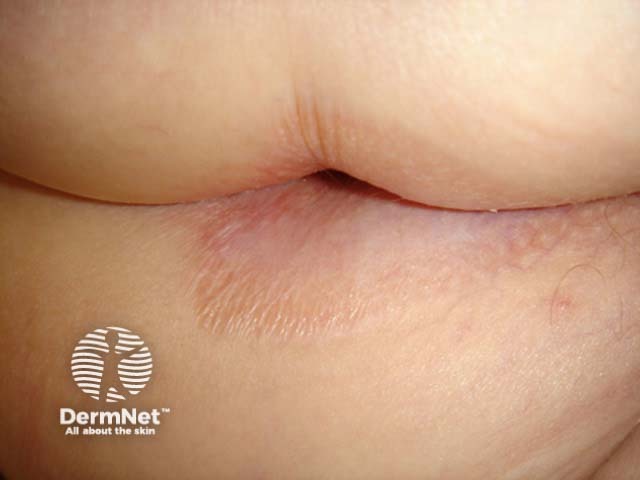
Lichen sclerosus
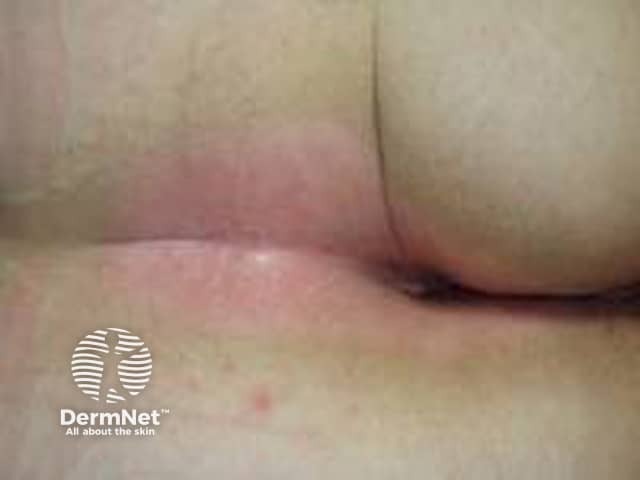
Flexural psoriasis
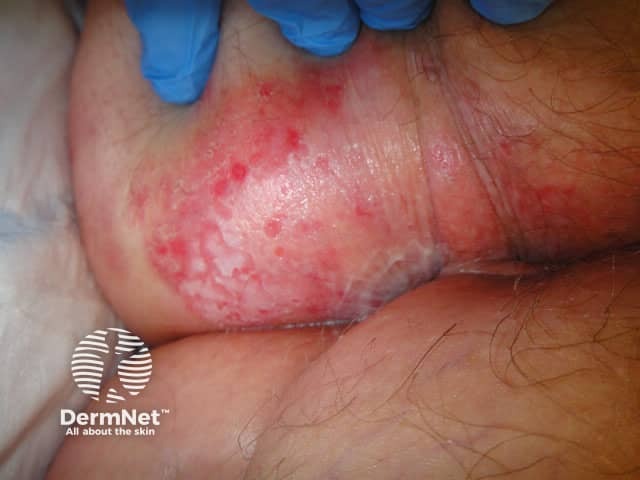
Extramammary Paget disease
Itchy anus is a symptom not a diagnosis, so a careful history and skin examination is required to reach a diagnosis.
See image pages — Perianal lichen sclerosus, Genital psoriasis, Extramammary Paget disease, Anal cancer
Pruritus ani is diagnosed on a normal examination of perianal skin apart from possible secondary excoriations and lichenification.
The cause of secondary itchy anus is usually established on history and examination.
Investigations may be required to confirm the cause.
Perianal itch usually improves with attention to the above. It may relapse during periods of stress, flare of the associated dermatosis, or if the above measures are relaxed.