Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author(s): Reuben Martin-Hendrie, Oral Medicine Registrar and Hadleigh Clark, Oral Medicine Specialist, Hospital & Specialist Dentistry, Auckland District Health Board, New Zealand. Copy edited by Gus Mitchell. May 2022
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Plasma cell mucositis is a rare, benign, inflammatory disorder of the upper aerodigestive tract that shares clinical and histologic features with plasma cell (Zoon) balanitis/vulvitis.
Plasma cell mucositis most commonly affects the oral mucosa and gingiva. Although it is typically painful with potential oral and oropharyngeal functional consequences, it can also be asymptomatic.
The condition has been known by multiple terms, including plasma cell orificial mucositis, idiopathic plasmacytosis, mucous membrane plasmacytosis of the upper aerodigestive tract, and oral papillary plasmacytosis. When limited to the lips, it is referred to as plasma cell cheilitis. Plasma cell gingivitis is a related condition, with exclusive gingival involvement. While concomitant oral and genital or cutaneous involvement has been described, it is exceedingly rare.
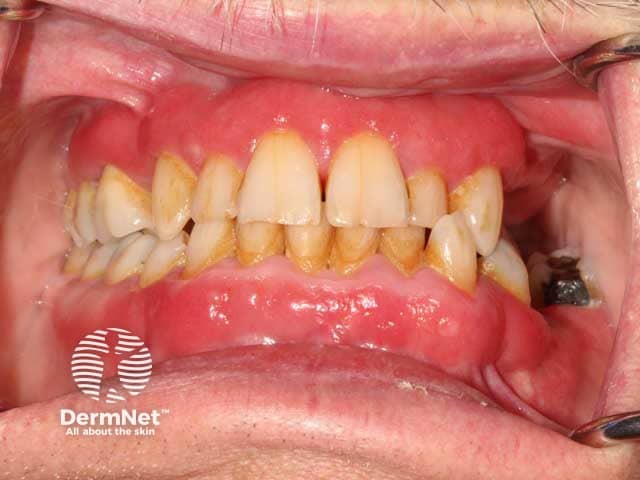
Red, glazed and oedematous changes on the gingivae in plasma cell mucositis (PCM-patient1)
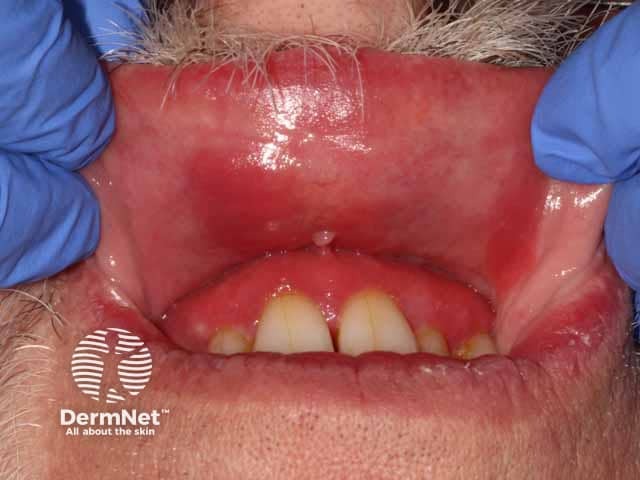
Red, glazed and oedematous changes on the gingiva and buccal mucosa in plasma cell mucositis (PCM-patient1)
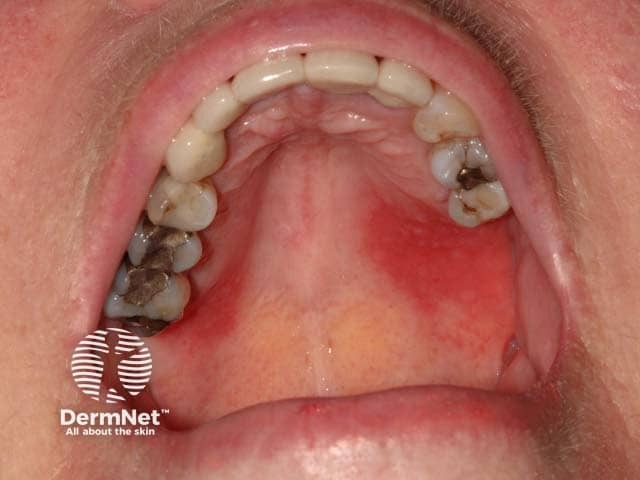
Red, glazed and oedematous changes on the hard palate in plasma cell mucositis (PCM-patient2)
Click to see more images of plasma cell mucositis
Fewer than eighty cases have been reported. Accurate prevalence and incidence data is therefore scarce. Approximately half of cases described involve the oral mucosa.
Plasma cell mucositis has a slight male predominance (1.2:1) with onset typically after the fourth decade. In the majority of cases, affected individuals have associated autoimmune or immunologically-mediated disease.
Since the early 2000s, an association between khat (qat) chewing and plasma cell mucositis has been observed. Khat is a plant (Catha edulis) endemic to the Eastern peninsula of Africa and Arabia. The leaves are chewed as part of cultural practice; the alkaloid cathinone produces stimulant and euphoric effects. The W.H.O. has classified khat as a drug of abuse and in many countries it is a controlled substance.
The cause of plasma cell mucositis is unknown. It has been postulated that an immune response may develop in susceptible individuals to an as-yet-unidentified infectious trigger (eg, Candida albicans, herpes simplex virus), actinic damage (of the lips), or contact sensitisation.
Plasma cell gingivitis appears to be a distinct variant presenting as a localised hypersensitivity reaction of the gingivae to flavouring agents (typically cinnamon and cinnamaldehydes) in toothpaste and chewing gums. Compared to plasma cell mucositis, which may be of insidious onset, plasma cell gingivitis typically arises abruptly (weeks/months) in response to the offending agent, with equally rapid resolution on agent withdrawal.
To date, no cases have evolved to plasma cell neoplasms.
Diagnosis can be challenging and requires a high index of suspicion, alongside clinicopathologic correlation.
Dependent on the distribution and surface morphology of involved sites, initial blood and microbiologic testing may include studies to exclude immunobullous (e.g. skin autoantibodies), granulomatous (e.g. sACE), infectious (e.g. fungal swabs, treponemal serology) and autoimmune (e.g. coeliac serology, ANA, ANCA, C3/C4, IgG subclasses) processes. When contact reactions are suspected, patch testing may be considered.
Tissue biopsy reveals a dense subepithelial infiltrate of mature plasma cells and pseudoepitheliomatous hyperplasia, Russell body formation, and secondary microabscess formation may be noted.
Adjunctive immunohistochemical (CD138) and immunoperoxidase (kappa and lambda in situ hybridisation) techniques are used to confirm polyclonality. Both cell markers on fresh-submitted tissue and complementary serology (immunoglobulins, serum protein electrophoresis, serum-free light chains), urinary Bence Jones proteins, and peripheral flow cytometry may be undertaken to further exclude underlying plasma cell dyscrasia.
The differential diagnosis of plasma cell mucositis is broad and dependent on both oral mucosal distribution and morphologic characteristics. It may include consideration of:
There is no consensus on the treatment for plasma cell mucositis.
First-line therapy is often:
Other treatments that have been used in recalcitrant cases include:
Given the often synchronous or metachronous presentation with other aerodigestive tract involvement, referral for nasendoscopy/bronchoscopy should be considered for any patient with phonation or breathing difficulties to exclude airway involvement.
Plasma cell mucositis is generally considered to be a benign condition with a favourable prognosis and no significant complications. Spontaneous resolution has been described, although this is slow and protracted.
Treatment is aimed at stabilisation of the disease; close clinical follow up is recommended.