Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author(s): Szu-Wen Chen, The University of Auckland; and Honorary Associate Professor Paul Jarrett, Dermatologist, Middlemore Hospital and Department of Medicine, The University of Auckland, Auckland, New Zealand (2023)
Previous contributors: Vanessa Ngan, Staff Writer (2006)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department
Introduction
Demographics
Causes
Clinical features
Variation of skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Prevention
Outcome
Trachyonychia is characterised by brittle nails that show diffuse longitudinal ridging and can be accompanied by pitting, loss of lustre, or a roughened nail plate.
Trachyonychia, also known as ‘rough nails’ or ‘sandpaper nails’, can involve any number of nails. Twenty-nail dystrophy refers to trachyonychia that affects all 20 nails.
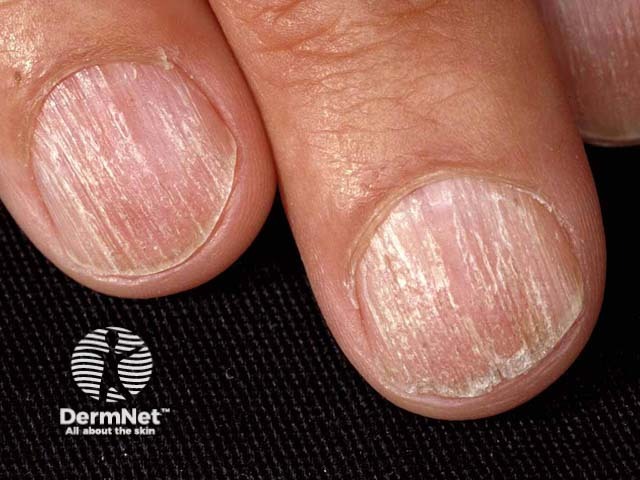
Opaque trachyonychia - there is opacity and longitudinal ridging
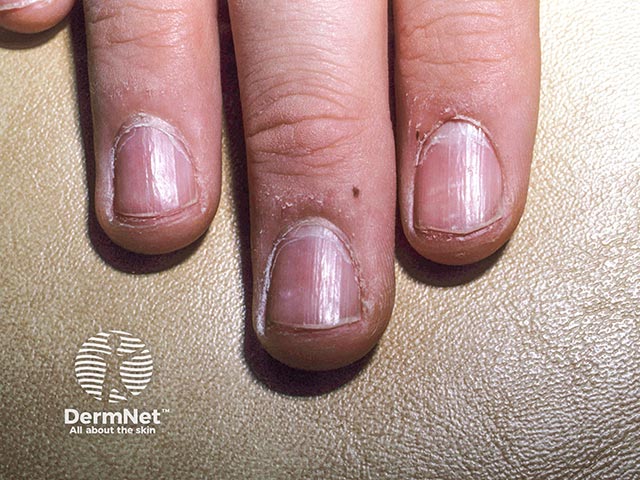
Shiny trachyonychia - the plate is bright and shiny (TND-patient2)
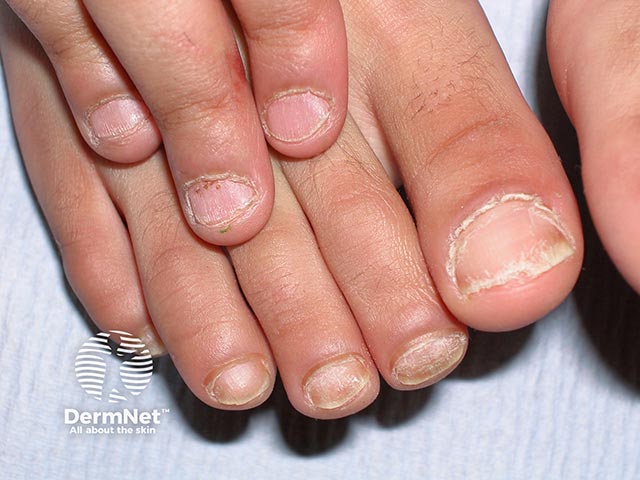
Trachyonychia due to 20 nail dystrophy - all of the nails were affected
Trachyonychia can occur in individuals of all ages, but is predominantly seen in children and young adults, with the peak incidence occurring between 3–12 years of age. It has been reported in both males and females, without a significant gender predilection.
Rare familial cases are described (autosomal dominant) and in identical twins.
The pathogenesis of trachyonychia remains unclear. It is hypothesised that inflammation within the nail matrix is involved in the development of the disease, and the extent of inflammatory activity is believed to influence disease severity.
It can be idiopathic or associated with:
Trachyonychia can be classified into two subtypes based on clinical presentation and severity.
Opaque trachyonychia:
Shiny trachyonychia:
In both opaque and shiny trachyonychia, koilonychia (spoon-shaped nails) can be observed, and fingernails are more commonly involved than toenails.
In twenty-nail dystrophy, all nails are affected.
The severity of the condition can vary between different nails within the same patient, and it is possible for both opaque and shiny varieties to coexist.
There are no variations in the clinical features of trachyonychia between patients with different skin colours.
Trachyonychia is primarily a clinical diagnosis based on history, full skin examination, and characteristic nail changes. However, some tests can assist in the diagnosis.
Treatment may not always be necessary as trachyonychia can improve or resolve spontaneously over time in many patients.
There is a lack of gold-standard evidence-based approaches due to limited data. Numerous treatment modalities have been trialled in small numbers of patients and responses vary.
Topical therapy:
Intralesional therapy:
Systemic therapy:
It is not usually justified to exhibit systemic therapy as most patients find this a cosmetic concern only, but if it is severe enough to have functional effects, the agents below have been advocated.
There are no specific preventive measures known for trachyonychia.
Trachyonychia is a benign but chronic condition. Resolving nail abnormalities without treatment can be a gradual process, often spanning several years.