Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Allergic contact dermatitis — extra information
Introduction Demographics Causes Clinical features Differential diagnoses Complications Diagnosis Treatment Outcome
What is allergic contact dermatitis?
Allergic contact dermatitis is a form of dermatitis/eczema caused by an allergic reaction to a material, called an allergen, in contact with the skin. The allergen is harmless to people that are not allergic to it. Allergic contact dermatitis is also called contact allergy.
Who gets allergic contact dermatitis?
Allergic contact dermatitis is common in the general population and in specific employment groups.
- It is more common in women than men, mainly due to nickel allergy and, recently, to acrylate allergy associated with nail cosmetics.
- Many young children are also allergic to nickel.
- Contact allergy to topical antibiotics is common in patients over the age of 70 years old.
- Allergic contact dermatitis is especially common in metal workers, hairdressers, beauticians, health care workers, cleaners, painters, and florists.
What causes allergic contact dermatitis?
Allergic contact dermatitis is a type 4 or delayed hypersensitivity reaction and occurs 48–72 hours after exposure to the allergen. The mechanism involves CD4+ T-lymphocytes, which recognise an antigen on the skin surface, releasing cytokines that activate the immune system and cause the dermatitis. Note:
- Contact allergy occurs predominantly from an allergen on the skin rather than from internal sources or food.
- Only a small number of people react to the specific allergen, which is harmless to those who are not allergic to it.
- They may have been in contact with the allergen for years without it causing dermatitis.
- Contact with tiny quantities of an allergen can induce dermatitis.
- Patients with impaired barrier function of the skin are more prone to allergic contact dermatitis, eg patients with leg ulcers, perianal dermatitis, or chronic irritant contact dermatitis.
- Patients with atopic dermatitis associated with defective filaggrin (a structural protein in the stratum corneum) have a high risk of also developing allergic contact dermatitis.
What are the clinical features of allergic contact dermatitis?
Allergic contact dermatitis arises some hours after contact with the responsible material. It settles down over some days providing the skin is no longer in contact with the allergen.
Allergic contact dermatitis is generally confined to the site of contact with the allergen, but it may extend outside the contact area or become generalised.
- Transmission from the fingers can lead to dermatitis on the eyelids and genitals.
- Dermatitis is unlikely to be due to a specific allergen if the area of skin most in contact with that allergen is unaffected.
- The affected skin may be red and itchy, swollen and blistered, or dry and bumpy.
Some typical examples of allergic contact dermatitis include:
- Eczema in the skin in contact with jewellery items, due to contact allergy to nickel
- Reactions to fragrances in perfumes and household items
- Eczema under adhesive plaster, due to contact allergy to rosin
- Swelling and blistering of face and neck in reaction to permanent hair dye, due to allergy to paraphenylenediamine
- Hand dermatitis caused by rubber accelerator chemicals used in the manufacture of rubber gloves
- Itchy red face due to contact with methylisothiazolinone, a preservative in wash-off hair products and baby wipes
- Fingertip dermatitis due to acrylates used in hair extensions and nail cosmetics.
- Reactions after dental implants containing acrylates
- Localised blistering at the site of topical medications such as antibiotics
- Swelling and blistering on exposed sites (eg face and hands) due to contact with plants such as poison ivy or, in New Zealand, the Japanese wax tree Toxicodendron succedaneum.
There is a very long list of materials that have caused contact allergy in a small number of individuals.
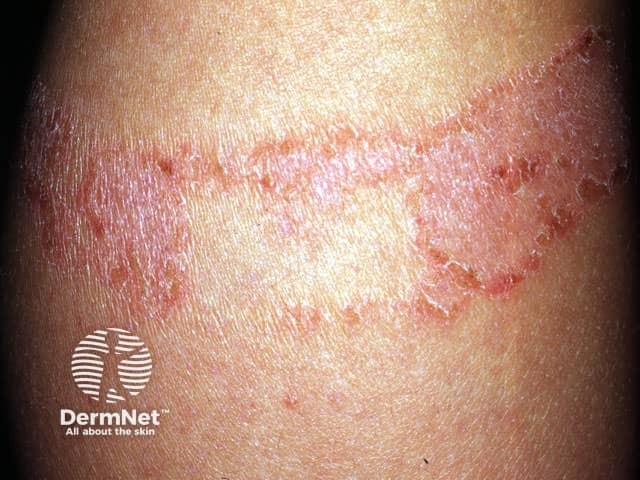
Adhesive plaster reaction
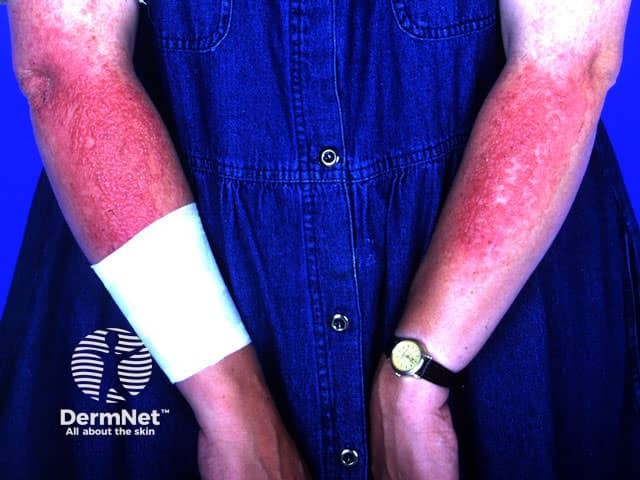
Sunscreen reaction
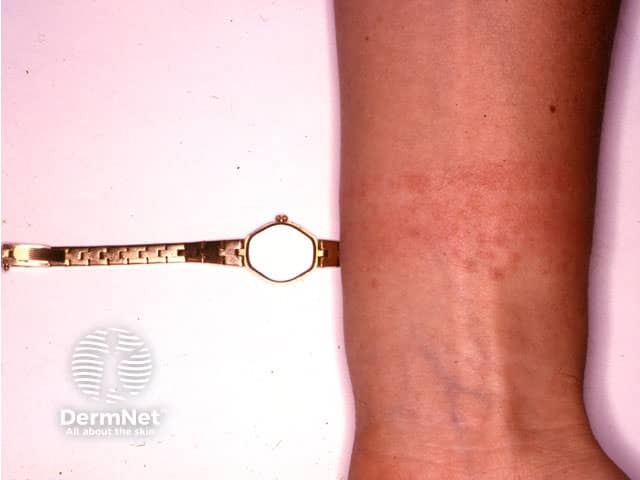
Watch strap reaction
See more images of allergic contact dermatitis
Specific allergic contact dermatitis images.
- Facial dermatitis images
- Hand dermatitis images
- Limb dermatitis images
- Truncal dermatitis images
- Patch test results images
What is the differential diagnosis of allergic contact dermatitis?
Allergic contact dermatitis should be distinguished from:
- Irritant contact dermatitis, which is due to irritation or repetitive injury to the skin. Irritants include water, soaps, detergents, solvents, acids, alkalis, and friction. Irritant contact dermatitis may affect anyone, providing they have had enough exposure to the irritant, but those with atopic dermatitis are particularly sensitive. Most cases of hand dermatitis are due to contact with irritants. Irritant contact dermatitis can occur immediately after a single injury or develop slowly after repeated exposure to an irritant.
- Other forms of dermatitis, which may mimic allergic contact dermatitis.
- Contact urticaria, in which a rash appears within minutes of exposure and fades away within minutes to hours. The allergic reaction to latex is the best-known example of allergic contact urticaria.
- Fungal infections; tinea corporis may present as a unilateral rash.
What are the complications of allergic contact dermatitis?
Allergic contact dermatitis starts as a localised reaction to an allergen in contact with the skin, but severe reactions may generalise due to autoeczematisation and can lead to erythroderma.
Ingestion of a contact allergen may rarely lead to baboon syndrome or generalised systemic contact dermatitis.
Photoallergy
Sometimes contact allergy arises only after the skin has been exposed to ultraviolet light. The rash is confined to sun-exposed areas even though the allergen may have been in contact with covered areas. This is called photocontact dermatitis.
Examples of photoallergy include:
- Dermatitis due to a sunscreen chemical, affecting the top but not the under the surface of the arm
- Dermatitis of face, neck, arms and hands due to antibacterial soap.
How is allergic contact dermatitis diagnosed?
Sometimes it is easy to recognise contact allergy and no specific tests are necessary. Taking a very good history including information on the work environment, hobbies, products in use at home and work and sun exposure will enhance the chances of finding a diagnosis. The rash usually (but not always) completely clears up if the allergen is no longer in contact with the skin, but recurs even with slight contact with it again.
The open application test is used to confirm contact allergy to a cosmetic, such as a moisturiser. The product under suspicion is applied several times daily for several days to a small area of sensitive skin. The inner aspect of the upper arm is suitable. Contact allergy is likely if dermatitis arises in the treated area.
Dermatologists will perform patch tests in patients with suspected contact allergy, particularly if the reaction is severe, recurrent or chronic. The tests can identify the specific allergen causing the rash.
Fungal scrapings of skin for microscopy and culture can exclude fungal infection.
Dimethylgloxime test is available to ‘spot test’ if a product contains nickel.
What is the treatment for allergic contact dermatitis?
It is important to recognise how you are in contact with the responsible substance so that, where possible, you can avoid it.
- Find out precisely what you are allergic to by having comprehensive patch tests.
- Identify where the allergen is found, thus read labels of all products before use.
- Carefully study your environment to locate the allergen. Note: many chemicals have several names, and cross-reactions to similar chemicals with different names are common.
- Wear appropriate gloves to protect hands from touching materials to which you react and remove gloves in the appropriate way. Some chemicals will penetrate certain gloves; seek a safety expert's advice.
- Ask your dermatologist to help.
Active dermatitis is usually treated with the following:
- Emollient creams
- Topical steroids
- Topical or oral antibiotics for secondary infection
- Oral steroids, usually short courses, for severe cases
- Phototherapy or photochemotherapy.
- Azathioprine, ciclosporin or another immunosuppressive agent.
- Tacrolimus ointment and pimecrolimus cream are immune-modulating calcineurin inhibitors and may prove helpful for allergic contact dermatitis.
What is the outcome for allergic contact dermatitis?
Contact allergy often persists lifelong so it is essential to identify the allergen and avoid touching it. Dermatitis may recur on re-exposure to the allergen.
- Some allergens are more difficult to avoid than others, with airborne allergens being a particular problem (eg epoxy resin, compositae pollen).
- The longer a person suffers from severe allergic contact dermatitis, the longer it will take to clear after the diagnosis is made and the cause detected.
- Dermatitis may clear up on avoidance of contact with the allergen, but sometimes it persists indefinitely, for example, chromate allergy.
Prognosis depends on patient education and compliance in avoiding allergens and appropriate skin care.
References
- Guidelines for care of Contact Dermatitis (J Bourke, I Coulson, J English) BJD, Vol. 160, No. 5, May 2009 (p946–54) — British Association of Dermatologists
- Fisher’s Contact Dermatitis, Ed Rietschel RL, Fowler JF. 6th edition, B.C Decker. 2008.
- Gaspari, A. Basic mechanisms and pathophysiology of allergic contact dermatitis. In: UpToDate, Fowler J (Ed). (Accessed on September 27, 2016.)
- Yiannias, J. Clinical features and diagnosis of allergic contact dermatitis. In: UpToDate, Fowler J (Ed). (Accessed on September 27, 2016.)
On DermNet
- Contact dermatitis
- Contact allergens
- Contact stomatitis
- Cosmetics allergy
- Aeroallergens
- Irritant contact dermatitis
- Photocontact dermatitis
- Consort allergic contact dermatitis
- Dermatitis
- Patch tests
- Open application test
- Pompholyx
- Hand dermatitis
- Hand care in healthcare workers
- Baboon syndrome
- Dermatitis online course for health professionals
- Sensitive skin
- Allergies explained
- Occupational dermatitis among construction workers
- Occupational skin disorders in homemakers
Other websites
- T.R.U.E. Tests: This site provides a wide range of information on contact dermatitis and contact allergy testing.
- Allergy New Zealand
- Occupational Dermatology Research and Education Centre, Australia
- Allergic contact dermatitis — Medscape Reference
- Contact Dermatitis — emedicine consumer health
- Contact Allergen Database
- Contact Dermatitis — British Association of Dermatologists
- Hand dermatitis — British Association of Dermatologists
- How to care for your hands — British Association of Dermatologists
