Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Splinter haemorrhage — extra information
Splinter haemorrhage
Author(s): Dr Alice Manley, Core Medical Trainee, Southmead Hospital, North Bristol Trust, United Kingdom. DermNet Editor in Chief: A/Prof. Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. February 2019.
Introduction Demographics Causes Clinical features Complications Diagnosis Treatment Outcome
What is a splinter haemorrhage?
A splinter haemorrhage is a longitudinal, red-brown haemorrhage under a nail and looks like a wood splinter. Seen end-on, the haemorrhage is in the lower part of the nail plate or underneath it.
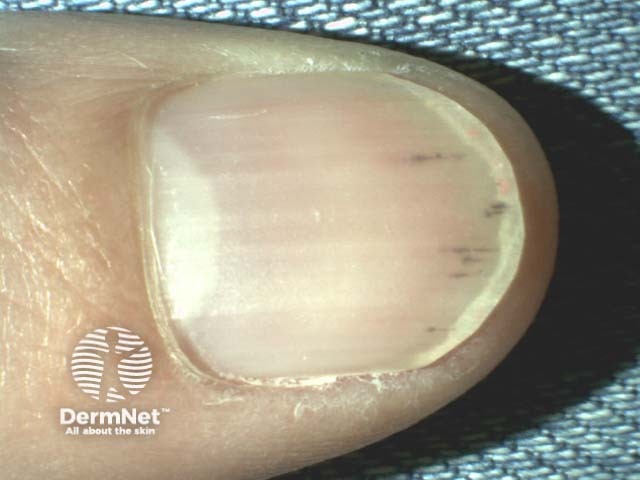
Splinter haemorrhages
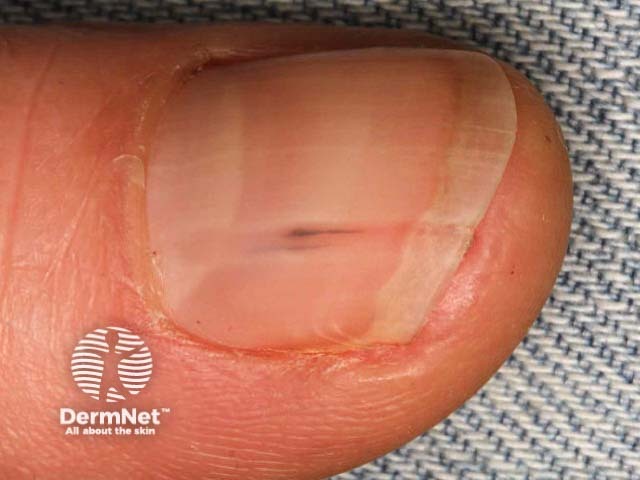
Splinter haemorrhages
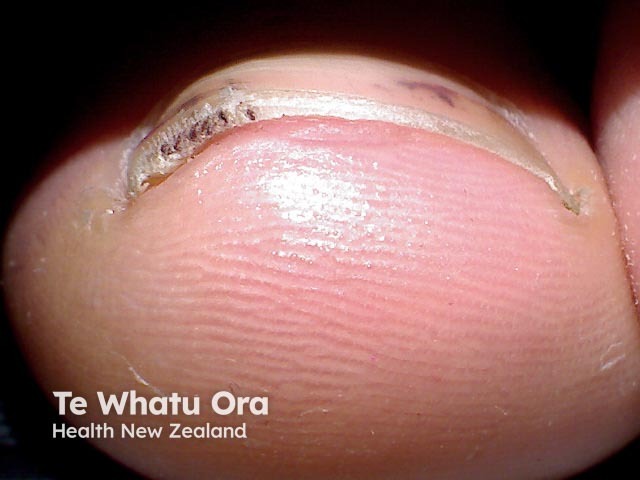
Splinter haemorrhages seen end on
Who gets splinter haemorrhages?
Splinter haemorrhages can occur at any age; however, they are more common in older people [1,2].
- In healthy individuals, splinter haemorrhages occur more frequently in men than women.
- Splinter haemorrhages are more frequent in dark-skinned people than in light-skinned people.
- The characteristics of patients who develop splinter haemorrhages relate to their underlying cause.
What causes splinter haemorrhages?
The most common cause of a splinter haemorrhage is trauma, including the application of an acrylic nail [3]. The longitudinal nature of splinter haemorrhages is explained by the orientation of the capillaries in the nail bed.
Infection
Splinter haemorrhages are present in 15–33% of patients with infective endocarditis in association with Osler nodes and Janeway lesions [3]. They may be due to septic emboli in the small vessels of the nail bed and the increased fragility of the vessel walls in sepsis [2,3].
Other infective causes include:
- Meningococcal disease
- Psittacosis
- Disseminated histoplasmosis.
Skin disease
Splinter haemorrhages are common signs of psoriatic nail disease and nail disease due to lichen planus [3]. They can also be associated with a tumour.
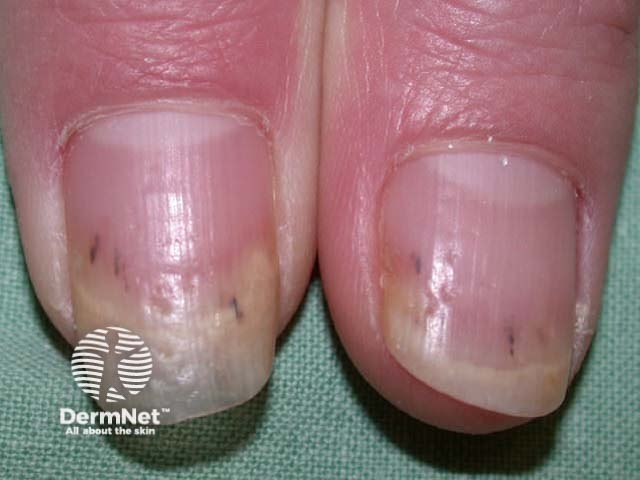
Psoriasis
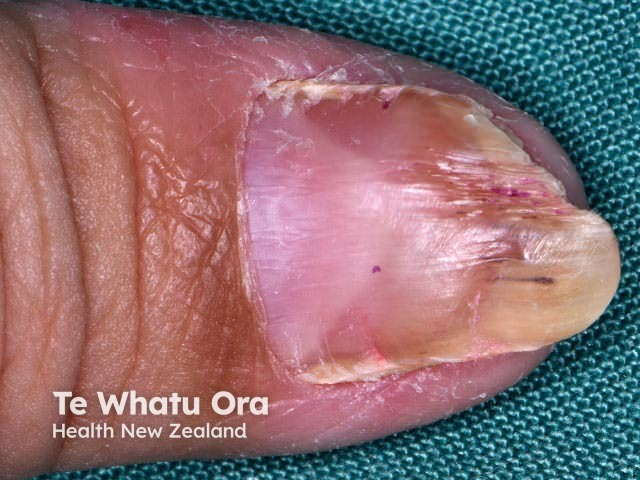
Psoriasis
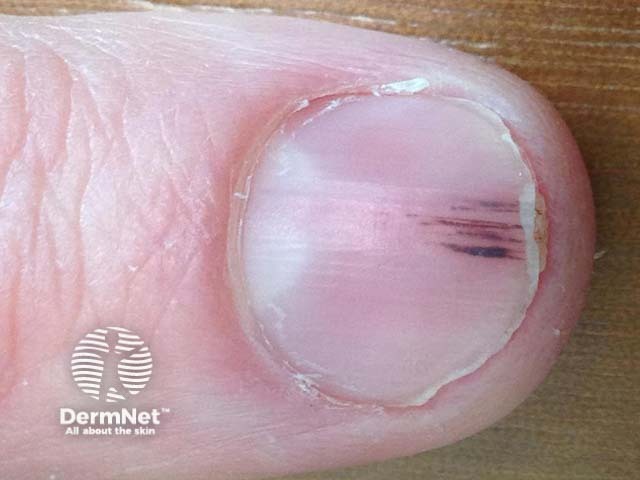
Onychopapilloma
Systemic diseases
Splinter haemorrhages may be due to microemboli or injury to vessel walls associated with vasculitis, including systemic diseases such as [3]:
- Primary antiphospholipid syndrome
- Systemic lupus erythematosus
- Raynaud disease
- Behcet disease
- Cutaneous vasculitis
- Scurvy.
Splinter haemorrhages are observed in patients with chronic kidney disease on haemodialysis or post-renal transplant, and may be explained by abnormal coagulation [3].
Drugs
Medications associated with splinter haemorrhages include [3]:
- Tyrosine kinase inhibitors (seen in 60–70% of patients taking sunitinib and sorafenib)
- Nitrofurantoin
- Ganciclovir
- Terbinafine
- Tetracyclines.
What are the clinical features of splinter haemorrhages?
Splinter haemorrhages present as longitudinal 1–3 mm red lines under the nail plate [2,3].
- They can be single or multiple.
- They may be asymptomatic or tender.
- The red line moves distally with time (weeks to months).
- Haemorrhages under the distal third of the nail plate are frequent and are usually a result of trauma such as a sports injury. They may be associated with subungual haematoma and nail splitting.
- Proximal haemorrhages, especially affecting multiple fingernails, are more likely due to a systemic disease, especially in women.
What are the complications of splinter haemorrhages?
There are no complications of splinter haemorrhages themselves; complications arise as a consequence of the underlying disease process.
How is a splinter haemorrhage diagnosed?
A careful history and physical examination are required to determine the underlying cause.
The diagnosis of splinter haemorrhages is made clinically or with the aid of dermatoscopy [1].
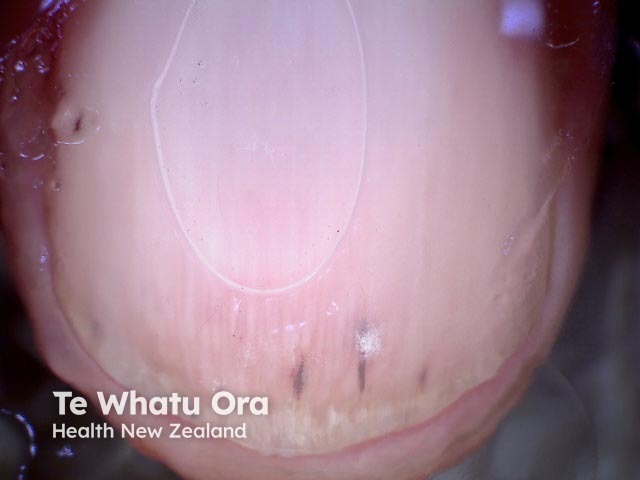
Splinter haemorrhage dermoscopy
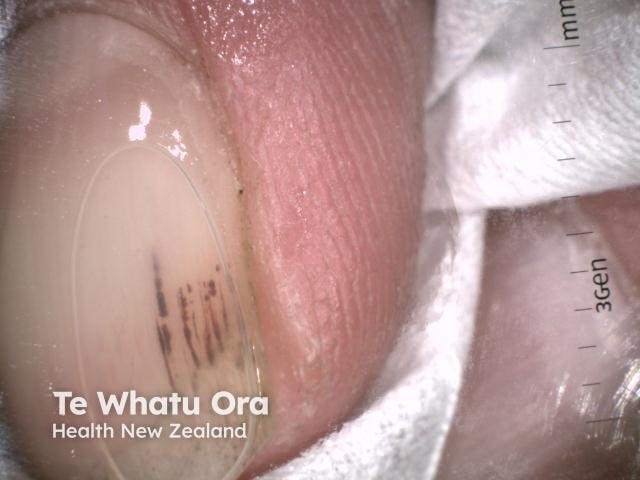
Splinter haemorrhage dermoscopy
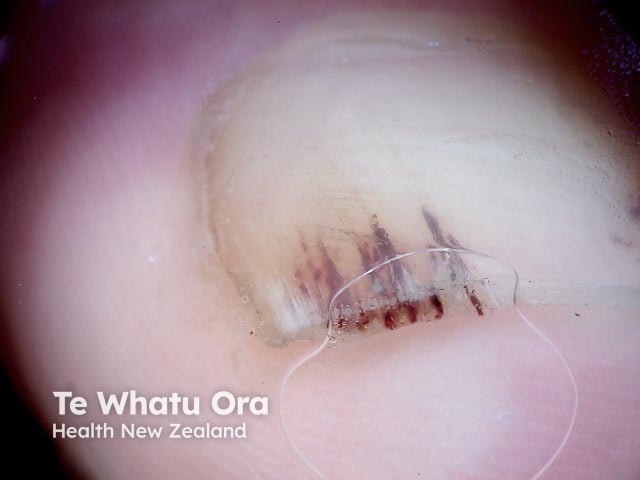
Splinter haemorrhage dermoscopy
What is the treatment for a splinter haemorrhage?
There is no specific treatment for a splinter haemorrhage.
Any treatment is targeted at an underlying systemic condition or at discontinuing a causative drug.
What is the outcome for a splinter haemorrhage?
If caused by trauma, a splinter haemorrhage grows out and disappears. Haemorrhages may continue to recur if the underlying cause remains.
References
- Tosti A, Piraccini BM. Nail disorders. Dermatology, 71, 1203–19
- Baran R, Dawber RPR. Diseases of the nails and their management, 4th edn. Chichester: John Wiley & Sons, 2012.
- Haber R, Khoury R, Kechichian E, Tomb R. Splinter haemorrhages of the nails: a systematic review of clinical features and associated conditions. Int J Dermatol 2016; 55: 1304–10. PubMed
On DermNet
- Bleeding and bruising
- Subungual haemorrhage
- Subungual haemorrhage images
- Psoriatic nail dystrophy
- Lichen planus
- Nail disorders
