Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Last Reviewed: October, 2025
Author(s): Dr Kate Kylie Velasco; Honorary Associate Professor Paul Jarrett, Dermatologist, Middlemore Hospital, Auckland, New Zealand (2024)
Peer reviewed by: Hunjung Choi, University of Missouri-Columbia School of Medicine, United States (2025)
Reviewing dermatologist: Dr Ian Coulson
Edited by the DermNet content department.
Introduction
Demographics
Causes
Clinical features
Variation in skin types
Complications
Diagnosis
Differential diagnoses
Treatment
Prevention
Outcome
Cutaneous plasmacytosis is a rare skin disorder characterised by red-brown lesions resulting from a benign cutaneous proliferation of mature plasma cells.
In isolated skin disease, the condition is referred to as ‘primary cutaneous plasmacytosis’ (PCP). In the presence of systemic involvement, the condition is referred to as ‘cutaneous and systemic plasmacytosis’ (CSP).
Cutaneous plasmacytosis is a rare condition that typically affects middle-aged individuals, but it can occur at any age. There is no gender predilection.
Cutaneous plasmacytosis has been predominantly documented in Asian populations, specifically Japanese, Chinese, Korean, and Thai populations. However, instances of this condition have also been observed among individuals of Māori, Pacific, and Caucasian descent.
The pathogenesis of cutaneous plasmacytosis is unknown; however, it is considered a reactive rather than malignant process.
Elevated interleukin-6 (IL-6) levels have been reported in some patients; IL-6 promotes antibody production and is involved in the differentiation of B-cells into mature plasma cells.
While infectious associations have been reported in some patients (eg, human herpes virus, Epstein-Barr virus, and hepatitis C virus), a causal relationship has not been established.
Cutaneous features:
Extracutaneous features:
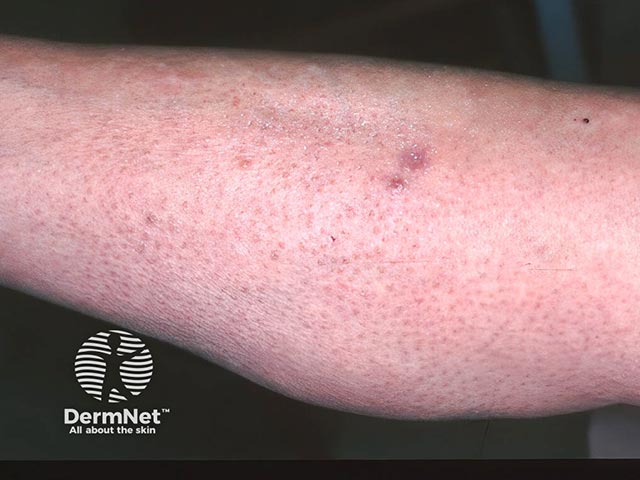
The violaceous nodule at the top of the shin was an area of plasmacytosis — the follicular eruption elsewhere was follicular cutaneous T cell lymphoma
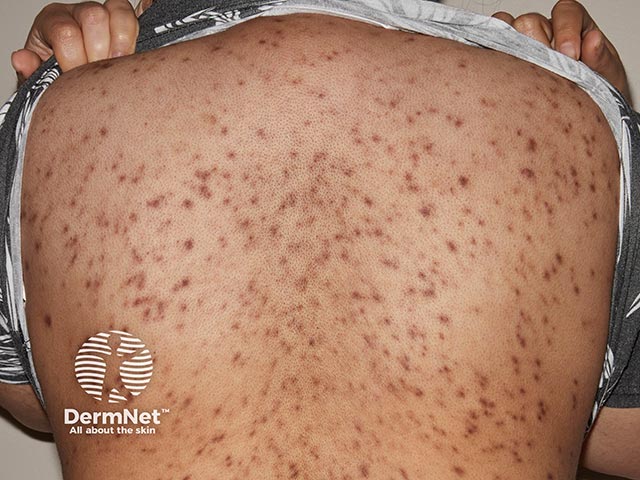
Extensive nodules of plasmacytosis over the back (PCP-patient1)
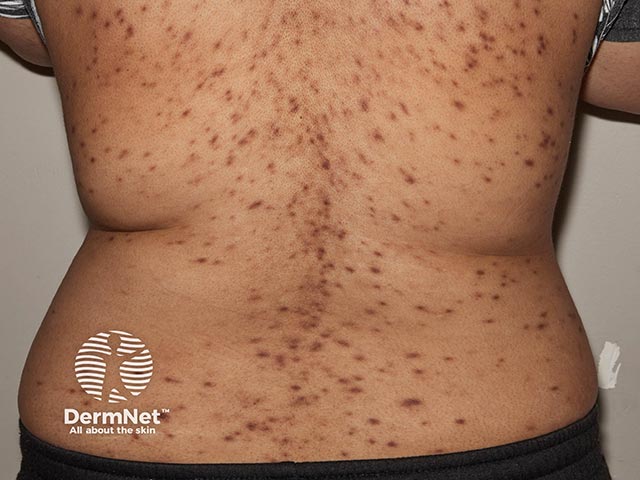
Plasmacytosis over the lower back (PCP-patient1)
Hyperpigmentary changes are more pronounced in skin of colour.
There are isolated reports of cutaneous plasmacytosis developing into T-cell lymphoma, non-Hodgkin lymphoma, and leukaemia. However, the incidence of malignant transformation is unknown.
Cutaneous plasmacytosis is typically diagnosed clinically based on characteristic cutaneous features and confirmed by biopsy.
Histopathology reveals perivascular and perineural plasma cell infiltrates in the dermis.
For more information, see: cutaneous plasmacytosis pathology.
Clonality studies (eg, with kappa or lambda immunohistochemistry) may be performed to exclude monoclonality — a feature of malignant neoplastic processes.
Serology may be helpful to rule out an infectious differential eg, syphilis or Lyme disease.
There is no definitive treatment for cutaneous plasmacytosis, and treatment may not be required for asymptomatic cases.
Treatments reported in literature include:
There are currently no known prevention strategies for cutaneous plasmacytosis.
Cutaneous plasmacytosis has a chronic, benign, and non-remitting course. Most patients remain well with no systemic concerns. Spontaneous resolution of asymptomatic cases has also been rarely reported.
Long-term follow-up should be considered to monitor for systemic involvement or malignant transformation, as this condition remains poorly understood.