Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Mark Duffill, Department of Dermatology, Waikato Hospital, Hamilton, New Zealand, 2001. Updated by A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, February 2016. Minor update November 2025.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Prevention
Outlook
Erosive pustular dermatosis presents with localised areas of pustules, lakes of pus, or crusts, which overlie eroded plaques or nodules and mainly affects the sun damaged, bald scalp of older individuals.
Erosive pustular dermatosis is also known as erosive pustulosis and erosive pustular dermatosis of the scalp.
Erosive pustular dermatosis occurs in males and females; most affected individuals are over the age of 80 years and have actinic keratoses and a history of squamous cell carcinoma or (less often) basal cell carcinoma of the scalp. Typically, it affects areas of scarring such as arise after injury, skin cancer surgery or shingles. Like other neutrophilic dermatoses, it may be more common in association with immune suppression, rheumatoid arthritis and myeloid haematological disorders.
Erosive pustular dermatosis has been reported as an adverse effect of epidermal growth-factor receptor inhibitors, such as gefitinib.
The cause of erosive pustular dermatosis of the scalp is unknown. However, it appears to relate to sun damage. It is often triggered by a minor injury to the affected skin (including a surgical procedure) (pathergy), and faulty wound healing may be involved. Infection is not thought to be the primary cause, as the lesions do not clear with antibiotics alone.
When it affects lower legs, venous stasis and oedema may be involved.
Rarely, drug-induced disease has been reported eg, latanoprost, minoxidil, and EGRF antagonists.
Erosive pustular dermatosis usually starts with tiny pustules on the scalp, forehead, or temples. It has also been reported to affect the lower legs.
The pustules evolve into lakes of pus or yellow-brown or greenish crusts. If these are removed, the skin underneath is red and moist. Extensive disease can itself result in scarring and extensive balding.
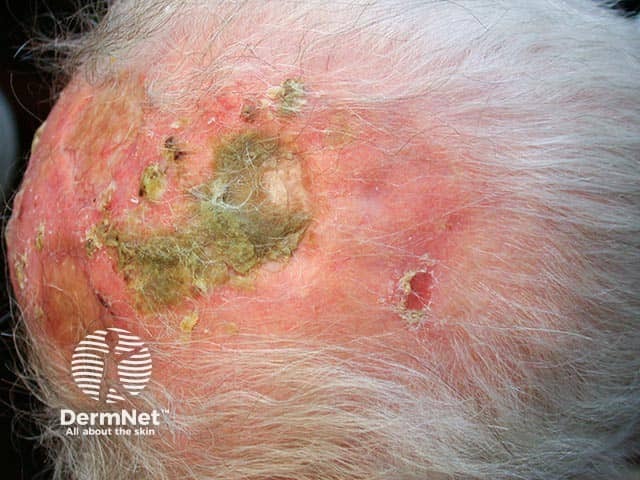
A thick crust overlying a large erosion on a bald scalp in erosive pustular dermatosis
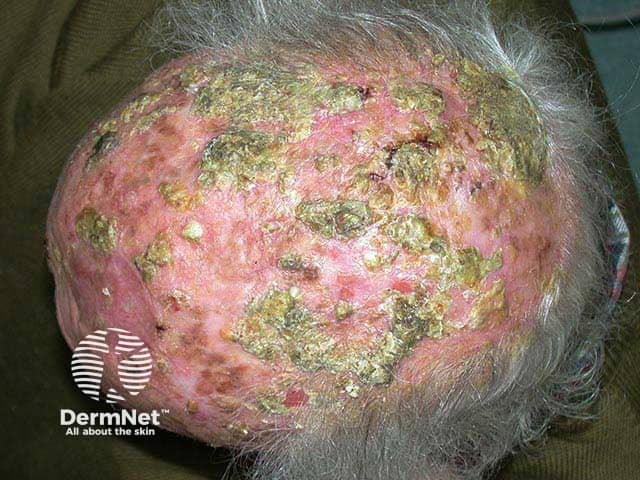
Multiple thick crusts overlying large erosions on a bald scalp in erosive pustular dermatosis
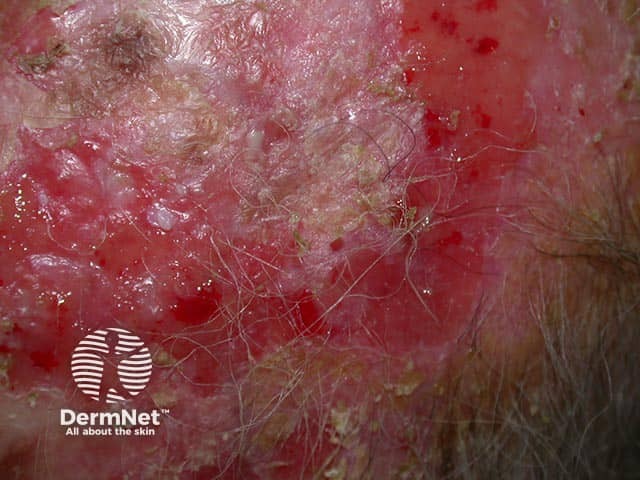
A large erosion revealed after removing the overlying crust in erosive pustular dermatosis
The main complications of erosive pustular dermatosis are:
Erosive pustular dermatosis is diagnosed by its characteristic clinical appearance. Culture of bacterial swabs may reveal Staphylococcus aureus. Scrapings may be undertaken for mycology, to rule out tinea capitis and kerion.
The underlying eroded skin frequently undergoes biopsy, as it is often difficult to determine clinically whether there is an underlying skin cancer. Multiple and deep biopsies may be useful. Histopathology shows subcorneal and non-follicular pustules, epidermal hypertrophy, or atrophy and erosions. There is a mixed dermal inflammatory infiltrate. which includes plasma cells and neutrophils. The findings are often non-specific.
Other conditions that should be considered in the differential diagnosis of erosive pustular dermatosis include:
The crusting should be removed by gentle soaking, perhaps using potassium permanganate (Condy's crystals) or acetic acid solution (dilute vinegar) as antiseptic astringent. A bland wound dressing is then applied.
Secondary bacterial infection should be treated with oral anti-Staphylococcal antibiotics such as flucloxacillin or erythromycin.
Erosive pustular dermatosis of the scalp improves with potent or ultrapotent topical steroids applied once or twice daily to the affected areas for a couple of weeks, then repeated as necessary if and when the skin disorder recurs. If long-term topical steroid is required, a calcineurin inhibitor such as tacrolimus ointment may be more suitable.
Other treatments that are reported to be helpful include:
Patients diagnosed with erosive pustular dermatosis should protect from the sun (wear a broad brimmed hat when outdoors), and be vigilant to recognise the early signs of recurrence, which should be treated as previously.
New actinic keratoses and skin cancers, especially squamous cell carcinoma, may arise in the affected areas and should be diagnosed and treated promptly. They may be difficult to distinguish from erosive pustular dermatosis of the scalp so repeated biopsies may be necessary.
Erosive pustular dermatosis usually clears up with treatment but may recur. The same treatment should be restarted, after carefully re-examining the skin to identify underlying skin cancers, if present.