Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Aoife Daly, Registrar, Radiation Oncology, Christchurch Hospital, Christchurch, New Zealand. DermNet New Zealand Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. November 2016.
Introduction
Demographics
Causes
Etiology
Clinical features
Diagnosis
Differential diagnoses
Treatment
Outcome
Follicular eruptions are skin conditions based on the hair follicle.
Follicular eruptions due to drugs may be acute or chronic eruptions. They present with monomorphic erythematous follicular papules and pustules.
Follicular eruptions due to drugs are also known as acneiform eruptions, papulopustular eruptions, drug-induced folliculitis and drug-induced acne.
Follicular eruptions are relatively uncommon, representing approximately 1% of adverse cutaneous reactions to drugs. They are most likely to occur on certain medications, and in acne-prone patients and age groups such as adolescents, with males thought to be more frequently affected than females.
Follicular eruptions due to drugs are easier to diagnose in age groups that do not typically experience acne vulgaris as this is a much more prevalent disorder and so the diagnosis of drug-induced acne is often not considered initially.
The risk of an eruption developing is proportional to the dose and duration of therapy.
The classes of drugs (and common causative individual medications within these classes) that are best known to cause follicular eruptions are:
There are proposed mechanisms for the ways in which some drugs are likely to cause folliculitis.
The time course of follicular eruptions depend on the responsible drug.
Typical characteristics of drug-induced follicular eruptions include:
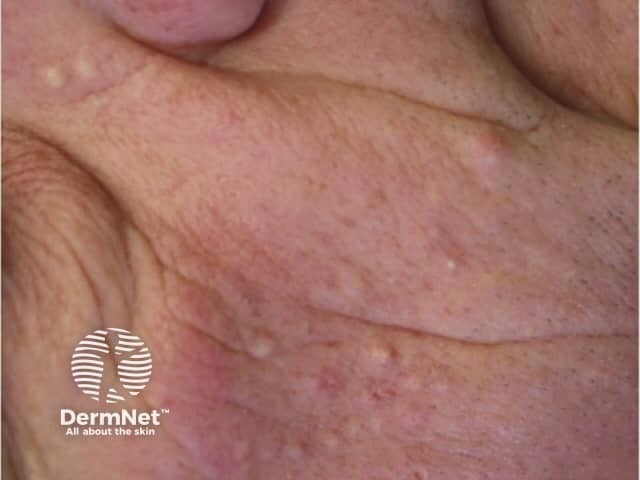
Folliculitis due to vemurafenib
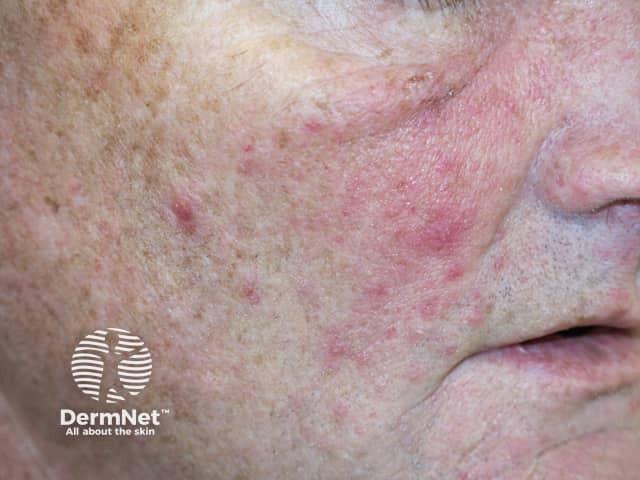
Folliculitis due to sirolimus
A follicular eruption due to a drug is generally diagnosed on the basis of the clinical appearance and a history of exposure to a drug known to be causative.
It may be appropriate to check the levels of suspected drugs where they are measurable (eg, lithium).
If a skin biopsy is taken, histological features may reveal:
Bacterial culture is not usually necessary, and is negative. Microscopy sometimes reveals Malassezia yeasts, particularly when corticosteroids are the cause of the eruption (steroid acne).
Other diagnoses that should be considered in patients with follicular eruptions include:
It is also possible to have a drug-induced folliculitis complicated by an overlying infection, especially in EGFRI-induced folliculitis.
The initial, and most important, management should be to withdraw the offending medication if this is possible.
The evidence for best treatment of persistent follicular eruptions is not robust and is the subject of ongoing research in patients who must continue the causative drugs.
Mild folliculitis may respond to topical treatment for acne:
If required, systemic therapy may include:
Most cases of follicular eruptions due to drugs will resolve within a few weeks of withdrawal of the causative medication. In persistent cases, the advice of a dermatologist should be sought.
Save