Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Malini Sivasaththivel, Resident Medical Officer, Eastern Health, Melbourne, Australia; Dr Martin Keefe, Consultant Dermatologist, Christchurch, New Zealand. Copy edited by Gus Mitchell. February 2022
Introduction Demographics Causes Clinical features Variation in skin types Complications Diagnosis Differential diagnoses Treatment Outcome
A comedo naevus (comedo nevus), also known as naevus comedonicus, is a rare, benign, cutaneous anomaly consisting of grouped, dilated follicular openings containing soft, dark keratin that resemble comedones.
Some authorities consider it to be a hamartoma arising from pilosebaceous follicles; others consider it to be an epidermal naevus involving hair follicles. They are usually solitary but may be part of a comedo naevus syndrome with associated skeletal, central nervous system, ocular, and other cutaneous abnormalities.

Comedo naevus
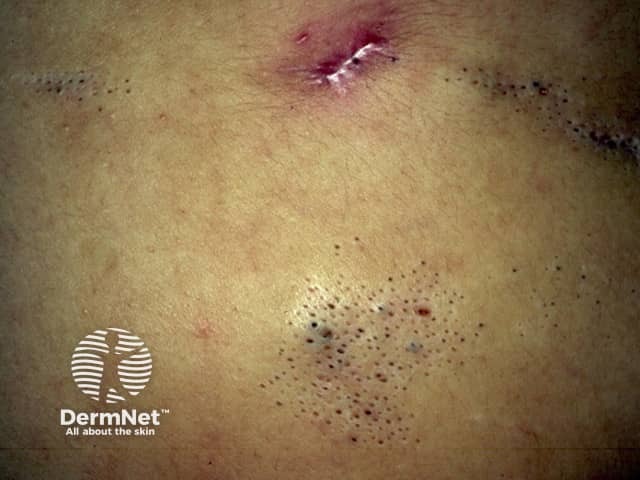
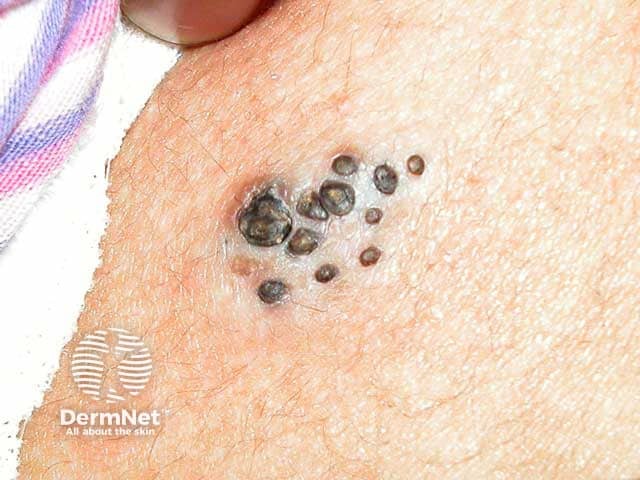
Comedo naevus
Comedo naevus on the abdomen
This epidermal naevus is rare. The true incidence is unknown but there are no sex or ethnic differences. Approximately 50% of cases present at birth and the remainder usually present before 10 years of age.
Adult onset is also described, even as late as the 7th decade, usually following trauma or a dermatosis such as herpes zoster, lichen planus, and pyoderma.
Comedo naevus is a mosaic disorder (some cells have the abnormal gene whilst others do not) resulting from somatic mutations in embryonic development. Mutations in FGFR2 are thought to be important, with increased expression of IL-1 alpha.
Recently, somatic mutations in the NEK9 gene have been described. This leads to activation of NEK9 kinase and disruption of normal follicular differentiation. Whilst these DNA changes have been found in follicular and non-follicular tissue, a follicle- specific effect of NEK9 has been hypothesised in the pathogenesis of comedo nevi.
More recently, upregulation of ABCA12 has been described. Germline mosaicism has also been postulated, where the earlier the errors occur in development, the more comedo naevi an individual is likely to develop.
Comedo naevi usually presents as a single group of dark hyperkeratotic papules and horny plugs with a honeycomb appearance. Comedo naevi are found most commonly on the face, trunk, neck, and upper extremities, but can affect any part of the body.
Multiple comedo naevi may be seen and the distribution pattern may be:
Two specific subtypes are seen:
Additional abnormalities associated with comedo naevus syndrome may affect the:
There are no differences in clinical features seen amongst different ethnic groups.
The complications often manifest during adolescence and include:
Comedo naevus is usually a clinical diagnosis. Dermoscopy may be helpful to highlight the typical appearance.
Histopathological evaluation is rarely required and will show epidermal invaginations with moderate atrophy resembling enlarged hair follicles. The invaginations contain lobes of sebaceous glands and have associated acanthosis and concentric laminae due to keratin production.
Comedo naevus is benign and asymptomatic so treatment is often unnecessary. Treatment may be considered for cosmetic reasons or for complications such as cysts and abscesses.
Topical therapies may show modest benefit:
Oral therapies:
Procedural therapies:
Comedo naevi remain unchanged over a person’s lifetime unless treated. As previously described, they may be subject to complications.