Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Drug-induced immunosuppression — extra information
Drug-induced immunosuppression
Author: Dr Leah Jones, Medical Registrar, Christchurch, New Zealand. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. July 2020.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Treatment
Outcome
What is drug-induced immunosuppression?
Drug-induced immunosuppression, also known as medication-induced immune suppression, is impaired immune system function due to medications used in the treatment of systemic diseases. This typically manifests as recurrent, severe, unusual, or opportunistic infections [1].
Medications used to treat dermatological conditions can affect the immune system to a variable extent.
Chronic drug-induced immunosuppression for other reasons (for example, to prevent rejection in organ transplantation patients) can be associated with dermatological complications [2].
Who gets drug-induced immunosuppression?
The main medications used in dermatology that cause significant drug-induced immunosuppression include [3]:
- Azathioprine
- Ciclosporin
- Mycophenolate mofetil
- Cyclophosphamide
- Systemic corticosteroids, such as prednisone.
Prednisone tablets
Azathioprine tablets
Mycophenolate capsules
Other medications that result in a milder impairment of immune function, especially if in conjunction with other agents, include:
- Methotrexate
- Janus kinase (JAK) inhibitors (baricitinib, tofacitinib)
- Phosphodiesterase (PD) E4 inhibitors (apremilast)
- Biological agents [4].
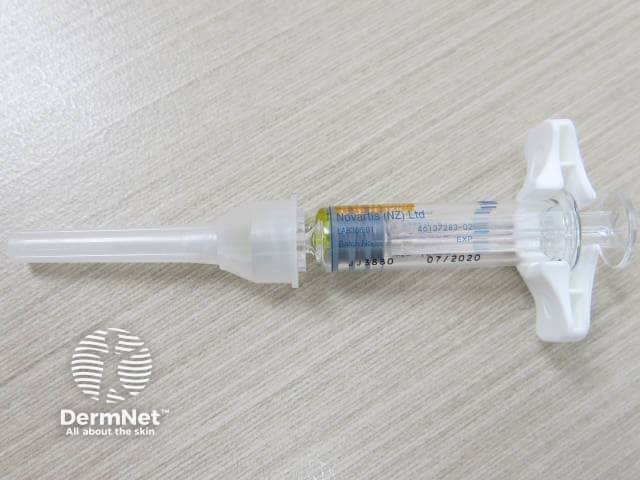
Methotrexate injection
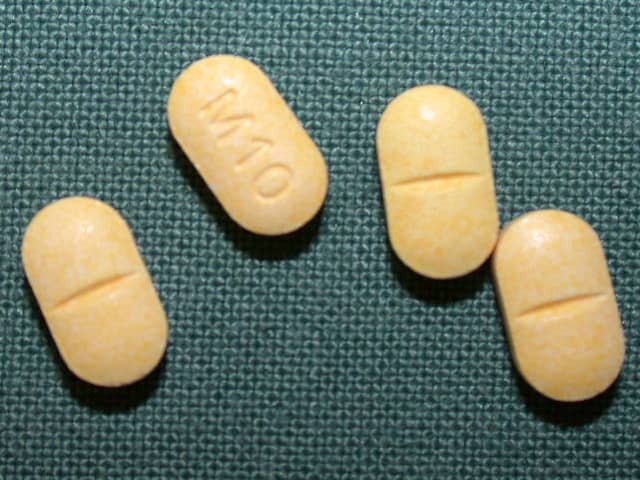
Methotrexate tablets
Examples of biological agents are:
- Tumour necrosis factor (TNF) alpha antagonists (infliximab, etanercept, adalimumab)
- Interleukin (IL) 12/23 antibodies (ustekinumab)
- IL 17 antibodies (secukinumab, ixekizumab, brodalumab)
- IL 13 antibodies (lebrikizumab)
- IL 4 receptor antibodies (dupilumab)
- Immunoglobulin (Ig) E antibodies (omalizumab).
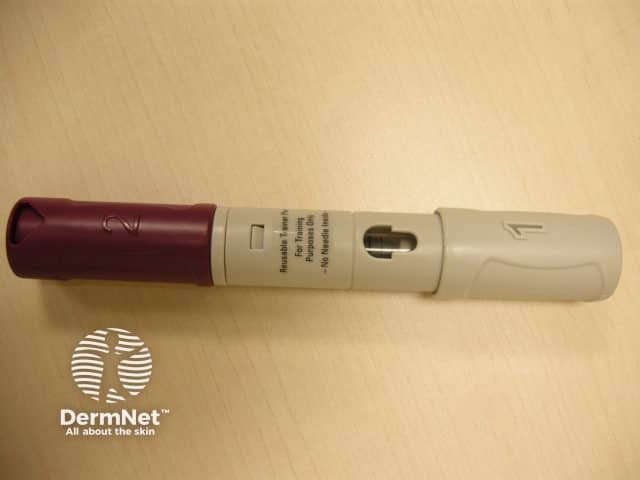
Adalimumab pen

Ustekinumab injection
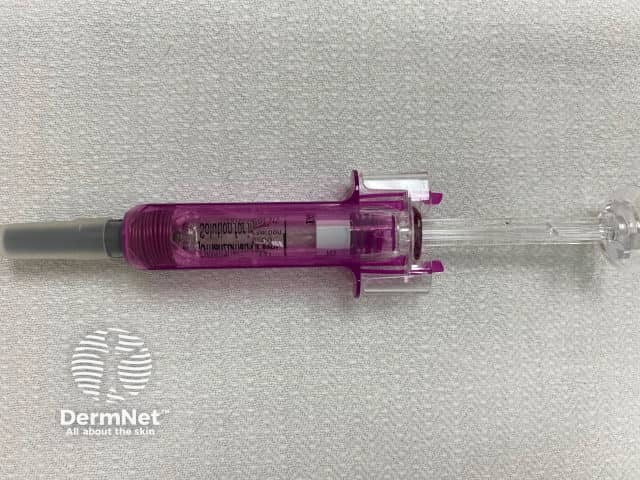
Omalizumab syringe
Immunosuppressive therapy is used in a variety of dermatological conditions, including psoriasis, atopic dermatitis, autoimmune bullous diseases, and cutaneous lupus erythematosus [3,4]. In some patients, drug-induced immunosuppression involves multiple agents with synergistic effects on the immune system [5,6].
What causes drug-induced immunosuppression?
Drug-induced immunosuppression can occur by one or more mechanisms, including [1,5]:
- T-cell inhibition — with ciclosporin, and to a lesser extent, corticosteroids
- Cytokine inhibition — with corticosteroids (their main mechanism) and biological agents
- Antimetabolite impairment of immune cell function and production — with azathioprine, mycophenolate mofetil, and to a lesser extent, methotrexate
- Alkylating agents that impair immune cell function and production — such as cyclophosphamide.
What are the clinical features of drug-induced immunosuppression?
High-dose chronic drug-induced immunosuppression is associated with non-infectious dermatological problems, such as acne, gingival enlargement, hypertrichosis, and induction of skin cancer, particularly cutaneous squamous cell carcinoma [2].
Drug-induced immunosuppression can lead to bacterial, viral, fungal, or parasitic infections, with different medications predisposing to specific types of organisms [6]. Some of these result in cutaneous disease, notably bacterial abscesses, herpes zoster, herpes simplex, cytomegalovirus, and viral warts [2].
Bacterial infections
Bacterial infections associated with drug-induced immunosuppression include [6]:
- Mycobacterium species
- Listeria species
- Staphylococcus species
- Nocardia species
- Escherichia coli
- Salmonella species
- Legionella pneumophilia
- Clostridium (Clostridioides) difficile.
Viral infections
Viral infections associated with drug-induced immunosuppression include [6]:
- Hepatitis B virus
- Hepatitis C virus
- Human immunodeficiency virus (HIV)
- Influenza
- Varicella-zoster virus (VZV) (chickenpox, herpes zoster)
- Herpes simplex virus (HSV)
- Epstein-Barr virus (EBV)
- Human papillomavirus (HPV) which can be sexually acquired (genital warts) or nonsexually acquired (viral warts)
- Cytomegalovirus.
Fungal and parasite infections
Fungal and parasitic infections associated with drug-induced immunosuppression include [6]:
- Candida species
- Histoplasmosis
- Aspergillus species
- Cryptococcus species
- Coccidioides immitis
- Blastomycoses
- Pneumocystis jiroveci
- Toxoplasma gondii.
What are the complications of drug-induced immunosuppression?
Infections associated with drug-induced immune suppression can cause serious morbidity and potentially mortality, particularly in those with a poor functional state at baseline [6,7]. Immunosuppressive therapy can also change the clinical features of an infection, making it more difficult to diagnose [6].
The development of a serious infection can lead to complex clinical management decisions regarding the immunosuppressive treatment of the underlying condition [5,6].
Drug-induced immunosuppression prevents the administration of live vaccines and limits the efficacy of other vaccines [6]. If practical, it is best to have any recommended vaccinations prior to initiating immunosuppressive drug treatment [5,6]. [see Immunisation in immunosuppressed dermatology patients]
How is drug-induced immunosuppression diagnosed?
Drug-induced immunosuppression is a clinical diagnosis based on the known effects of the patient’s medications.
To quantify the extent of drug-induced immunosuppression, antibody response can be measured before and after vaccination for pneumococcus. However, this predominantly assesses humoral immunity, not cell-mediated immunity, and is rarely performed [8].
What is the treatment for drug-induced immunosuppression?
The effects of drug-induced immunosuppression can be limited by taking preventative measures such as [5,6]:
- Update vaccinations prior to initiation of immune suppression
- Annual influenza vaccination
- Screening for infections or immunity to specific pathogens prior to initiation (eg, tuberculosis, viral hepatitis, HIV) [see Tuberculosis screening]
- Patient education regarding the risk of infections and the need for prompt medical attention
- Specialist consultation and risk management prior to international travel.
Antibiotics, antivirals (such as aciclovir), or antifungals should be prescribed promptly in response to symptoms and signs consistent with infection.
If infections are severe or recurrent, the immunosuppressive therapy may need to be reduced or stopped and alternative treatment options considered [1,6].
What is the outcome for drug-induced immunosuppression?
Drug-induced immunosuppression has a variable prognosis. This can be based on the characteristics of the drug, the patient, and the disease being treated [1,5,7].
Drug characteristics include:
- The type of medication
- The dose of the medication
- The duration of treatment
- Synergistic effect of multiple immunosuppressive medications.
Patient characteristics include:
- Baseline functional state
- Age
- The indication for immunosuppressive therapy
- Co-morbidities and vaccination status
- Adherence to preventative measures and management.
Low-dose, single-agent immunosuppressive therapy for a short duration carries only a minor risk of serious infection and mortality [1,2,9].
Approved datasheets are the official source of information for medicines, including approved uses, doses, and safety information. Check the individual datasheet in your country for information about medicines.
We suggest you refer to your national drug approval agency such as the Australian Therapeutic Goods Administration (TGA), US Food and Drug Administration (FDA), UK Medicines and Healthcare products regulatory agency (MHRA) / emc, and NZ Medsafe, or a national or state-approved formulary eg, the New Zealand Formulary (NZF) and New Zealand Formulary for Children (NZFC) and the British National Formulary (BNF) and British National Formulary for Children (BNFC).
References
- Meyer K, Decker C, Baughman R. Toxicity and monitoring of immunosuppressive therapy used in systemic autoimmune diseases. Clin Chest Med 2010; 31: 565–88. DOI: 10.1016/j.ccm.2010.05.006. PubMed
- Leis-Dosil VM, Prats-Caelles I. Practical management of immunosuppressants in dermatology. Dermatology 2018; 109: 24–34. DOI: 10.1016/j.ad.2017.05.005. PubMed
- Aslam A, Griffiths C. Drug therapies in dermatology. Clin Med 2014; 14: 47–53. doi: 10.7861/clinmedicine.14-1-47. PubMed Central
- Wiseman A. Immunosuppressive medications. Clin J Am Soc Nephrol 2016; 11: 332–43. doi: 10.2215/CJN.08570814. PubMed Central
- Orlicka K, Barnes E, Culver E. Prevention of infection caused by immunosuppressive drugs in gastroenterology. Ther Adv Chronic Dis 2013; 4: 167–185. doi: 10.1177/2040622313485275. PubMed Central
- Schmied E, Dufour JF, Euvrard S. Nontumoral dermatologic problems after liver transplantation. Liver Transpl 2004; 10: 331. DOI: 10.1002/lt.20089. PubMed
- Dixon WG, Kezouh A, Bernatsky S, Suissa S. The influence of systemic glucocorticoid therapy upon the risk of non-serious infection in older patients with rheumatoid arthritis: a nested case-control study. Ann Rheum Dis 2011; 70: 956. DOI: 10.1136/ard.2010.144741. PubMed
- Plotkin SA. Correlates of protection induced by vaccination. Clin Vaccine Immunol 2010; 17: 1055. DOI: 10.1128/CVI.00131-10. PubMed
- Beaugerie L, Kirchgesner J. Balancing benefit vs risk of immunosuppressive therapy for individual patients with inflammatory bowel diseases. Clin Gastroenterol Hepatol 2019; 17: 370–9. DOI: 10.1016/j.cgh.2018.07.013. PubMed
On DermNet
- Monitoring immune-modulating drugs used in dermatology
- Immunisation in immunosuppressed dermatology patients
- Tuberculosis screening
- Skin cancer in transplant recipients
Other websites
- Immunosuppression — Medscape
- Immunisation recommendations for children and adult patients treated with immune-suppressing medicines — British Association of Dermatologists
- Immunisation for adults with immune-mediated inflammatory disease (IMID) — The Immunisation Advisory Centre (New Zealand)
