What is panniculitis?
Panniculitis refers to a group of conditions that involve inflammation of subcutaneous fat. Despite having very diverse causes, most forms of panniculitis have the same clinical appearance. The diagnosis is established by a skin biopsy, as there are characteristic microscopic features depending on the cause. The most common form of panniculitis is erythema nodosum.
Panniculitis is classified as mostly septal panniculitis or mostly lobular panniculitis depending on the site of the most intense microscopic inflammation. Most types of panniculitis have both septal inflammation (early) and lobular inflammation (later). Further classification is based on whether or not there is subcutaneous vasculitis, and the type of inflammation noted (neutrophils, lymphocytes, histiocytes, granulomas).
Classification of panniculitis
Mostly septal panniculitis with vasculitis
- Leukocytoclastic vasculitis
- Superficial thrombophlebitis
- Cutaneous polyarteritis nodosa
- Behcet disease
Mostly septal panniculitis without vasculitis
- Erythema nodosum
- Panniculitis associated with biologic agents
- Lipodermatosclerosis (sometimes)
- Post-irradiation panniculitis
- Necrobiosis lipoidica
- Scleroderma, which may be localised (morphoea profunda)
- Subcutaneous granuloma annulare
- Rheumatoid nodule
- Necrobiotic xanthogranuloma
Mostly lobular panniculitis with vasculitis
- Erythema nodosum leprosum (leprosy)
- Lucio phenomenon (leprosy)
- Erythema induratum of Bazin (associated with tuberculosis)
- Other forms of infective panniculitis (sometimes)
- Neutrophilic lobular panniculitis associated with rheumatoid arthritis
- Crohn disease
- Nodular vasculitis
- By exclusion, nodular panniculitis
Mostly lobular panniculitis without vasculitis
- Sclerosing panniculitis (lipodermatosclerosis)
- Neutrophilic panniculitis/subcutaneous Sweet syndrome
- Eosinophilic panniculitis
- Calciphylaxis
- Oxalosis
- Sclerema neonatorum
- Subcutaneous fat necrosis of the newborn
- Cold panniculitis
- Lupus panniculitis
- Panniculitis in dermatomyositis
- Pancreatic panniculitis
- Alpha-1-antitrypsin deficiency
- Infective panniculitis (sometimes)
- Factitial panniculitis
- Subcutaneous sarcoidosis (Rosai-Dorfman disease)
- Traumatic panniculitis
- Lipomembranous ischaemic panniculitis
- Lipoatrophy
- Panniculitis due to intralesional steroid injection
- Gout panniculitis
- Crystal-storing panniculitis
- Cytophagic histiocytic panniculitis
- Post-irradiation pseudosclerodermatous panniculitis
- Panniculitis associated with halogenodermas (iodides, bromides)
- By exclusion, nodular panniculitis
Neutrophilic panniculitis
- Pancreatic panniculitis
- Alpha-1-antitrypsin deficiency
- Infection — with septic thrombi and emboli
- Panniculitis related to rheumatoid arthritis — with vasculitis
- Panniculitis induced by the BRAF inhibitor, vemurafenib
- Factitial panniculitis
- Erythema induratum (associated with tuberculosis)
- Subcutaneous acute febrile neutrophilic dermatosis (Sweet syndrome) with leukocytoclasis but without true vasculitis
- Early erythema nodosum; this has septal inflammation. Note that later lesions of erythema nodosum have lymphocytic infiltration.
What are the clinical features of panniculitis?
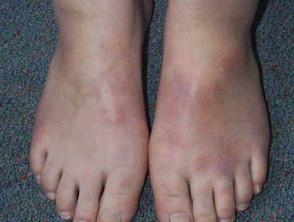
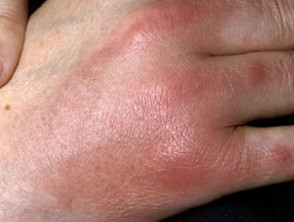
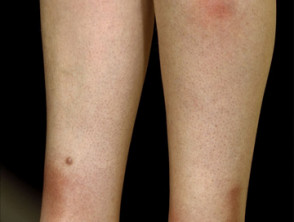
Panniculitis presents typically with:
- Thickened and firm nodules and plaques
- Erythematous or pigmented overlying skin
- Pain and tenderness.
Sometimes, lesions resolve to leave localised subcutaneous atrophy (lipodystrophy).
Panniculitis
Panniculitis with systemic features
Associated symptoms of fever, malaise and arthralgia are common in patients with panniculitis. When these are prominent, diagnoses to consider include:
- Cutaneous vasculitis
- Infective panniculitis
- Subcutaneous acute febrile neutrophilic dermatosis
- Panniculitis associated with pancreatic disease
- Alpha-1-antitrypsin deficiency panniculitis
- Cytophagic histiocytic panniculitis.
How is panniculitis diagnosed?
Panniculitis is diagnosed and classified by a combination of clinical features, biopsy findings and microbiological culture. Sometimes other investigations are necessary (such as chest X-ray in erythema nodosum and alpha-1-antitrypsin levels).
The histopathology may show the inflammation to be lobular, septal or mixed, with or without vascular damage, and predominantly neutrophils, lymphocytes or granulomatous.
What is the treatment of panniculitis?
Treatment of panniculitis includes:
- Treat the underlying cause, if known (eg, stop a medication, treat an infection)
- Rest and elevate the affected area
- Compression hosiery (18–25 mm Hg pressure if these can be tolerated)
- Pain relief using anti-inflammatory medications such as aspirin, ibuprofen or diclofenac
- Systemic steroids (oral or injected) to settle the inflammation
- Anti-inflammatory antibiotics including tetracycline or hydroxychloroquine
- Potassium iodide
- Surgical removal of persistent or ulcerated lesions.
What is the outcome of panniculitis?
The outcome depends on the underlying cause of the inflammation. After an inflammatory phase of weeks to months, panniculitis often settles down. It may recur. Some forms of panniculitis do not leave a mark, but destructive forms of panniculitis tend to leave a permanent dent in the skin.