Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Dr Leah Jones, Medical Registrar, Christchurch, New Zealand. DermNet Editor in Chief: Adjunct A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. Copy edited by Gus Mitchell. July 2020. Updated October 2020.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Perifolliculitis capitis abscedens et suffodiens is an uncommon cause of scarring alopecia characterised by perifollicular and follicular pustules and nodules.
It is also known as dissecting cellulitis of the scalp and Hoffman disease.
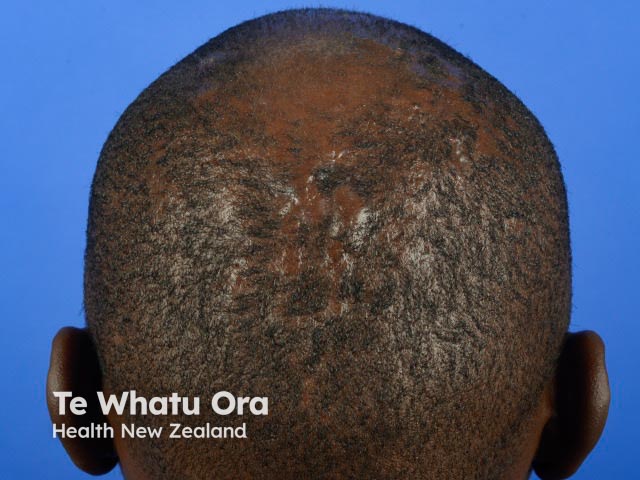
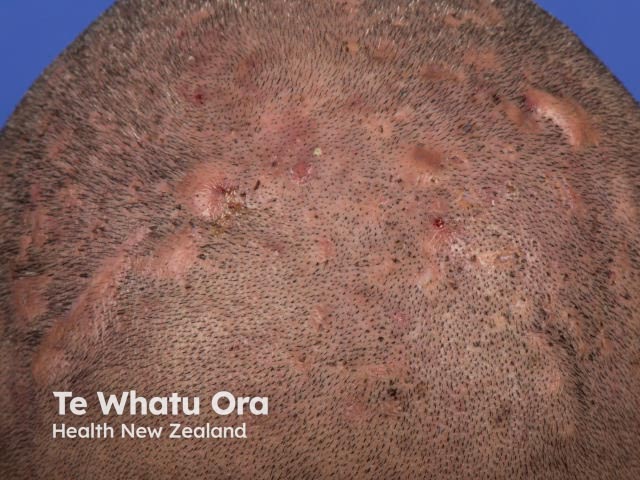
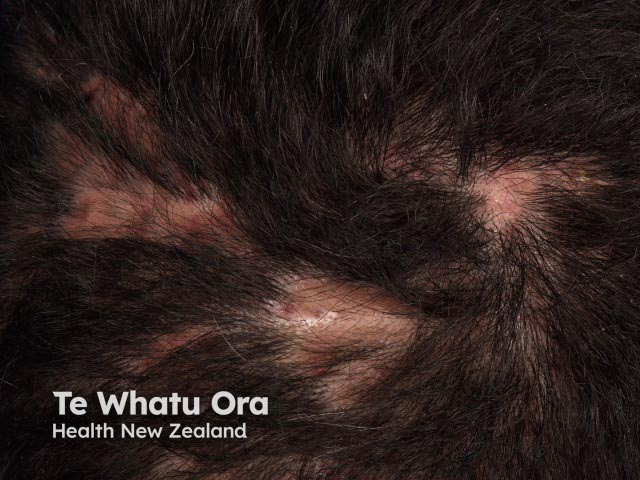
Perifolliculitis capitis abscedens et suffodiens is most commonly seen in men of African descent in the third, fourth and fifth decades of life. African women, Caucasians and other ethnicities, and occasionally children, can also present with this condition.
Perifolliculitis capitis abscedens et suffodiens sometimes occurs in people who have other forms of follicular occlusion syndrome.
A defect in follicular keratinisation causes occlusion and subsequent inflammatory destruction of the follicle. An aberrant immune to response to commensal bacteria may be involved with the pathogenesis, particularly coagulase-negative staphylococci.
Perifolliculitis capitis abscedens et suffodiens can affect single or multiple areas of the scalp, with a predilection for the vertex and posterior scalp. It is typically painful.
Signs can include:
Patients with perifolliculitis capitis abscedens et suffodiens may also have hidradenitis suppurativa, nodulocystic acne and/or pilonidal disease.
Perifolliculitis capitis abscedens et suffodiens is also associated with arthritis and spondyloarthropathy. Sacroiliitis is reported in three-quarters of sufferers.
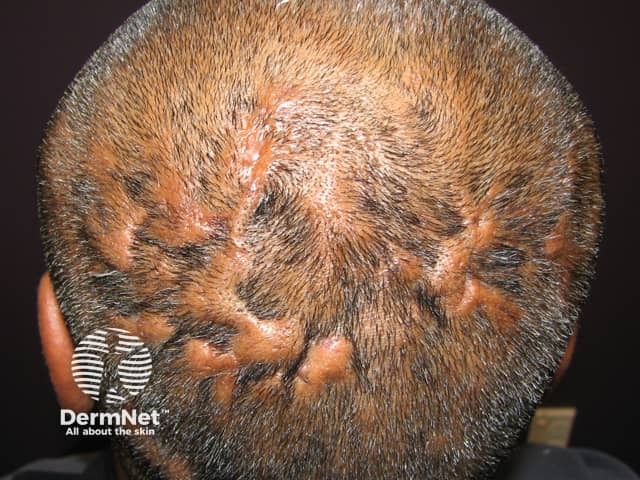
Dissecting cellulitis
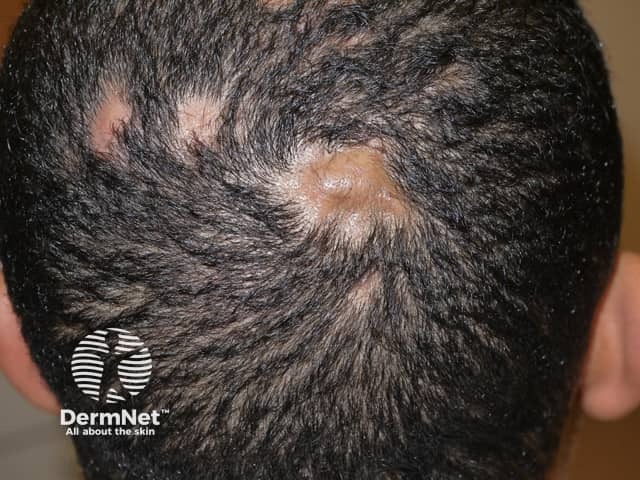
Dissecting cellulitis
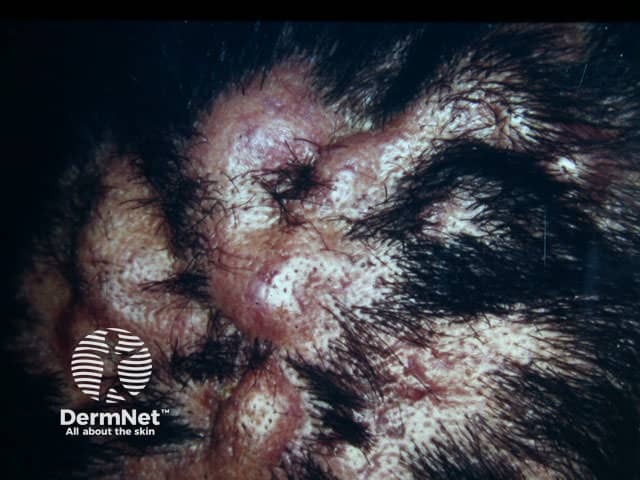
Dissecting cellulitis
Three stages of disease progression have been described on dermoscopy.
Pain during acute inflammatory flares, together with the hair loss, has a major impact on quality of life.
Perifolliculitis capitis abscedens et suffodiens can be complicated by secondary bacterial infection due to Staphylococcus aureus, Pseudomonas, and anaerobic bacteria.
Hair loss is temporary initially, but the deep inflammation eventually leads to patchy cicatricial alopecia, which can be very extensive.
Cutaneous squamous cell carcinoma has been reported.
Perifolliculitis capitis abscedens et suffodiens is a clinical diagnosis.
A swab of the exudate for culture is recommended to identify secondary bacterial infection. However the swab is often sterile.
A skin biopsy may show perifollicular mixed inflammatory infiltrate, abscess, and granuloma formation. Fibrosis is common.
Perifolliculitis capitis abscedens et suffodiens can be confused with other inflammatory conditions of the scalp including:
Treatment of perifolliculitis capitis abscedens et suffodiens often requires a multi-pronged approach, especially initially and during acute flares.
Perifolliculitis capitis abscedens et suffodiens usually follows a chronic course with variable relapses. The subsequent scarring alopecia results in permanent, patchy hair loss.