Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Stephen Thomas, Medical Registrar, Gold Coast, and Honorary Dermatology Registrar and Research Fellow, Princess Alexandra Hospital, Brisbane, Australia; Dr Priyam Sobarun, Dermatology Registrar, Queensland Institute of Dermatology, Brisbane, Australia. DermNet Editor in Chief: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. December 2016.
Madarosis refers to loss of the eyelashes or eyebrows. It can be:
In non-scarring madarosis, follicular structures are retained and it is potentially reversible. Scarring madarosis is due to deeper inflammation and fibrosis, and it is more likely to result in permanent lash and hair loss.
Loss of the eyelashes alone is also known as milphosis.
Madarosis can be found in both sexes and in any age group but, depending on the underlying cause, it is more common in older people.
Madarosis is caused by any process that damages the hair bulb or hair shaft, leading to either temporary or permanent hair loss.
Common causes of madarosis include:
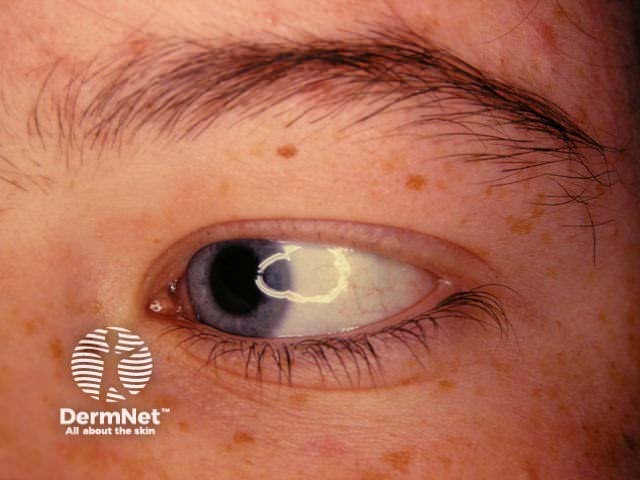
Alopecia areata
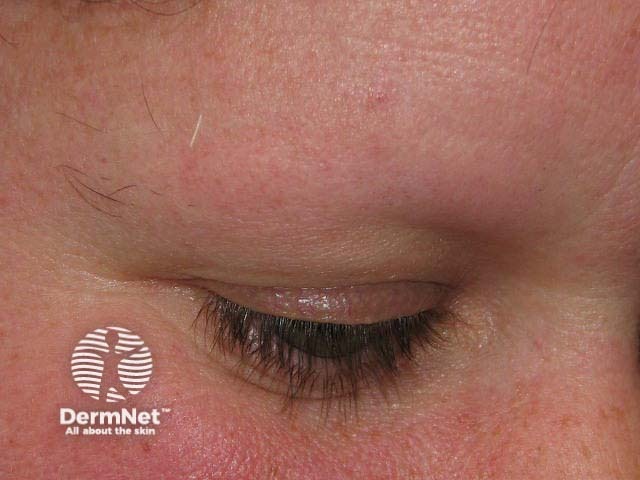
Alopecia areata
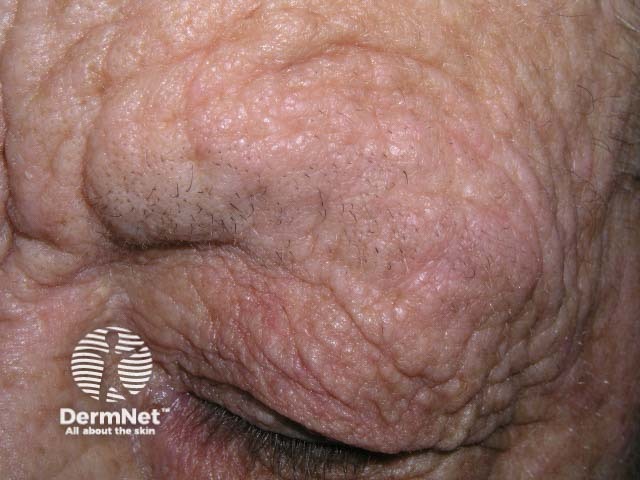
Atopic eczema
Uncommon causes of madarosis include:
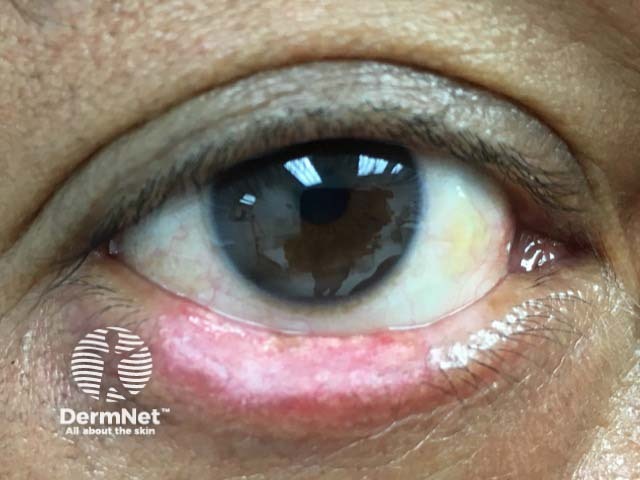
Discoid lupus erythematosus
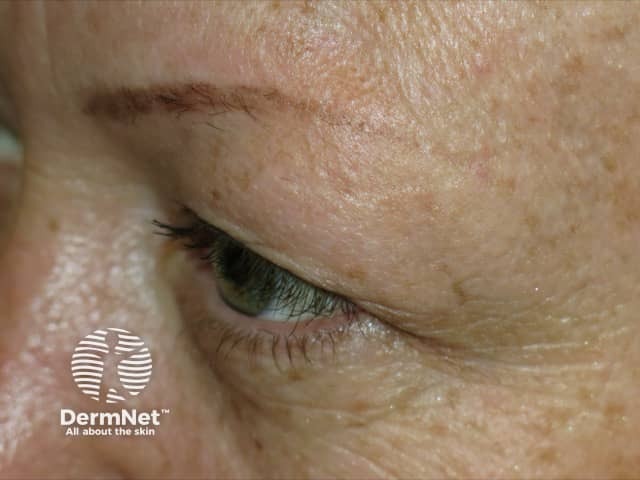
Frontal fibrosing alopecia
Madarosis can be clinically diagnosed based on an adequate history and examination. Useful tests may include:
The specific treatment recommended for madarosis depends on its underlying cause (eg, antibiotics are recommended for madarosis caused by bacterial infection). Non-specific measures that can be used in madarosis include: