Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Hidradenitis suppurativa — extra information
Hidradenitis suppurativa
Authors: Vanessa Ngan, Staff Writer, Dr Amanda Oakley, Dermatologist, New Zealand, 1997. Updated December 2015. Revised by: Dr Abdulhadi Jfri, PGY-5 Dermatology Resident, Division of Dermatology, McGill University, Montreal, Canada. Dr Elizabeth O’Brien, Assistant Professor of Dermatology, McGill University, Montreal, Canada, January 2021. Minor amendment by Ian Coulson, Dermatologist, Feb 2025
Introduction
Demographics
Causes
Clinical features
Assessment
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
See Management of hidradenitis suppurativa: an Australasian consensus statement
What is hidradenitis suppurativa?
Hidradenitis suppurativa (HS), also called acne inversa, is a chronic inflammatory skin condition that affects apocrine gland-bearing skin in the axillae, groin, and under the breasts. It is characterised by persistent or recurrent boil-like nodules and abscesses that culminate in a purulent discharge, sinuses, and scarring.
HS can have a significant psychological impact, and many patients suffer from anxiety, depression, and impairment of body image.
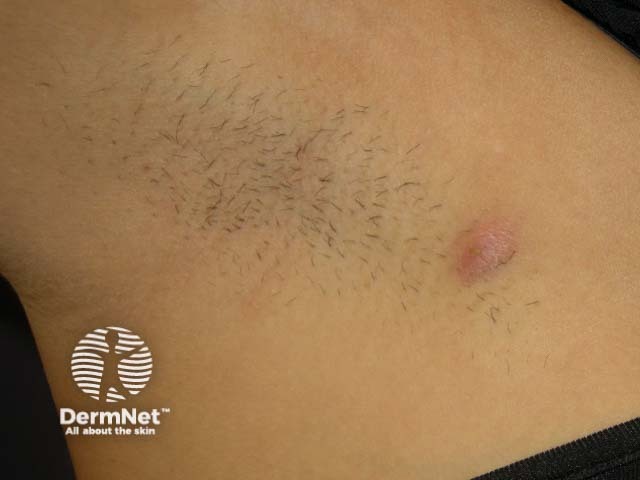
Hurley Stage I hidradenitis suppurativa
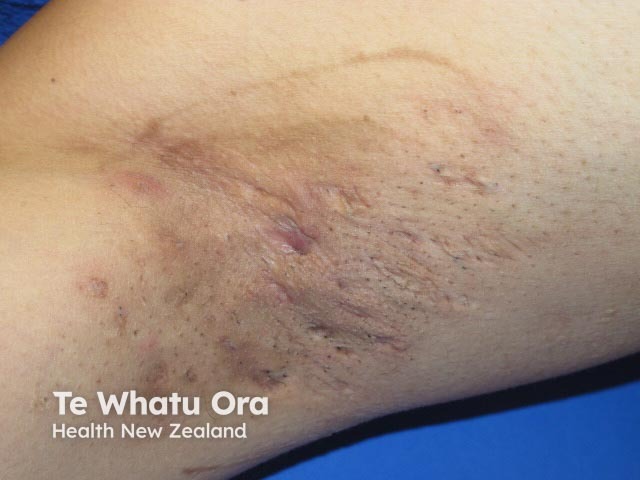
Hurley Stage II hidradenitis suppurativa
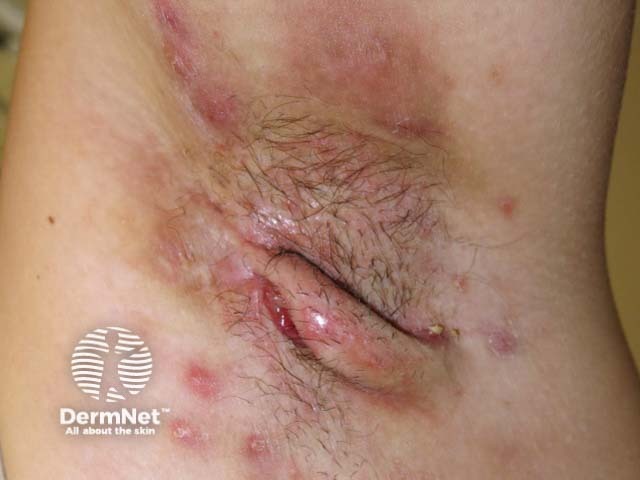
Hurley Stage III hidradenitis suppurativa
Who gets hidradenitis suppurativa?
Hidradenitis suppurativa often starts at puberty, is most active between the ages of 20 and 40 years, and in women can resolve at menopause. It is three times more common in females than in males. Associations and risk factors include:
- Family history of HS; 30–40% report at least one other family member affected
- Obesity and insulin resistance (metabolic syndrome)
- Cigarette smoking
- African ethnicity
- Follicular occlusion syndrome: acne conglobata, dissecting cellulitis, pilonidal sinus
- Inflammatory bowel disease, particularly Crohn disease
- Other skin disorders: psoriasis, acne, hirsutism
- Comorbidities: hypertension, diabetes mellitus, dyslipidaemia, thyroid disorders, arthropathies, polycystic ovary syndrome, adverse cardiovascular outcomes
- Drugs: lithium, sirolimus, biologics
- Syndromes
- PAPA syndrome
- PASH syndrome (pyoderma gangrenosum, acne, suppurative hidradenitis)
- PAPASH syndrome (pyogenic arthritis, pyoderma gangrenosum, acne, suppurative hidradenitis).
Hidradenitis developing at a young age in childhood or early adolescence may be an indicator of underlying precocious puberty.
What causes hidradenitis suppurativa?
Although ‘hidradenitis’ implies an inflammatory disease of the sweat glands, we now know that HS is an autoinflammatory syndrome. The exact pathogenesis is not yet understood. Factors involved in the development of acne inversa include:
- Follicular occlusion
- An abnormal cutaneous or follicular microbiome
- Release of pro-inflammatory cytokines
- Inflammation causing rupture of the follicular wall, destroying sebaceous and apocrine glands and ducts.
What are the clinical features of hidradenitis suppurativa?
Acne inversa can affect single or multiple areas in the axillae, neck, inframammary fold, and inner upper thighs. Anogenital involvement most commonly affects the groin, mons pubis, vulva, scrotum, perineum, buttocks, and perianal folds.
HS is characterised clinically by:
- Open double-headed comedones
- Painful firm papules and nodules
- Pustules, fluctuant pseudocysts, and abscesses
- Draining sinuses linking inflammatory lesions
- Hypertrophic and atrophic scars.
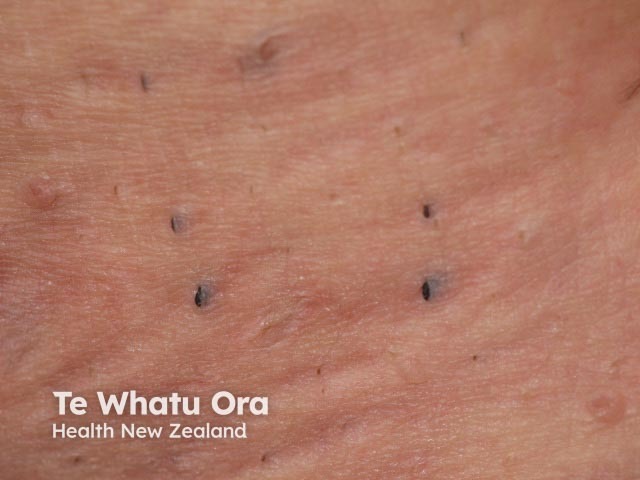
Comedones in hidradenitis suppurativa
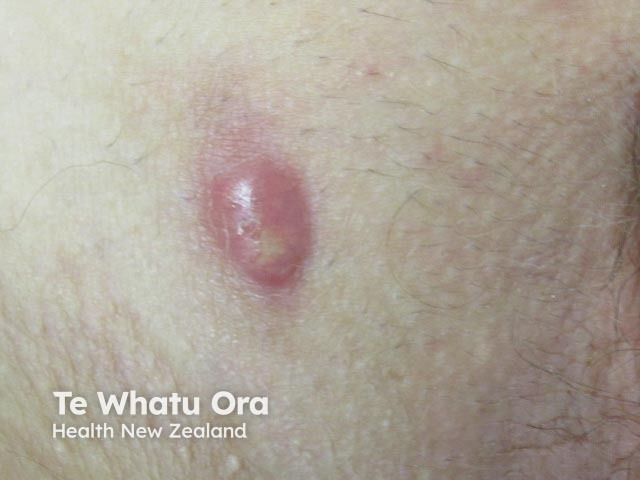
Inflammatory lesion in hidradenitis suppurativa
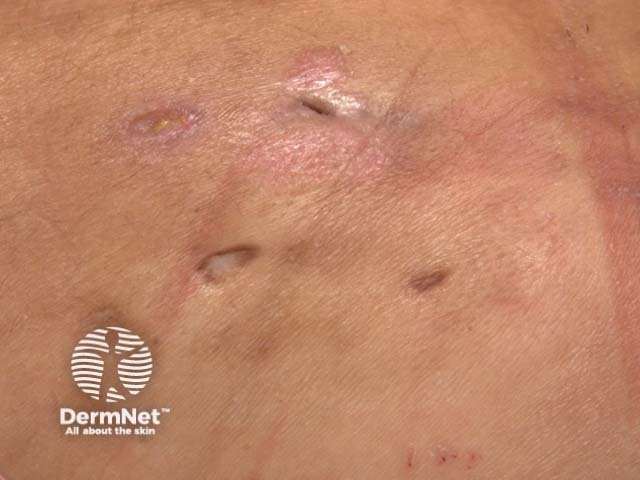
Scarring in hidradenitis suppurativa
Clinical phenotypes of hidradenitis suppurativa (HS)
Phenotype |
Clinical features |
Regular HS |
|
Frictional furuncle |
|
Scarring folliculitis |
|
Conglobata |
|
Syndromic |
|
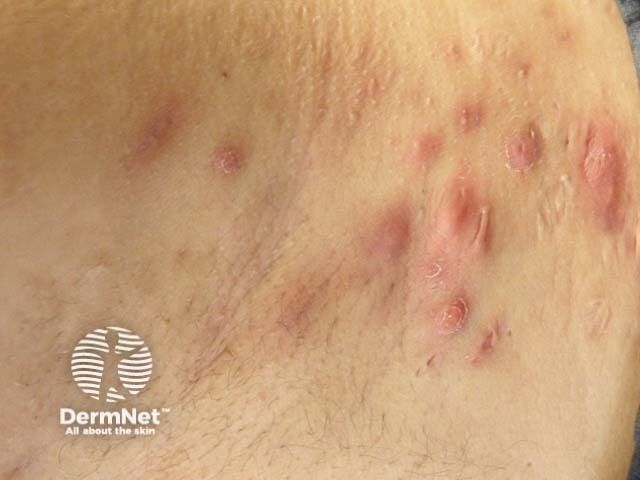
Regular hidradenitis suppurativa
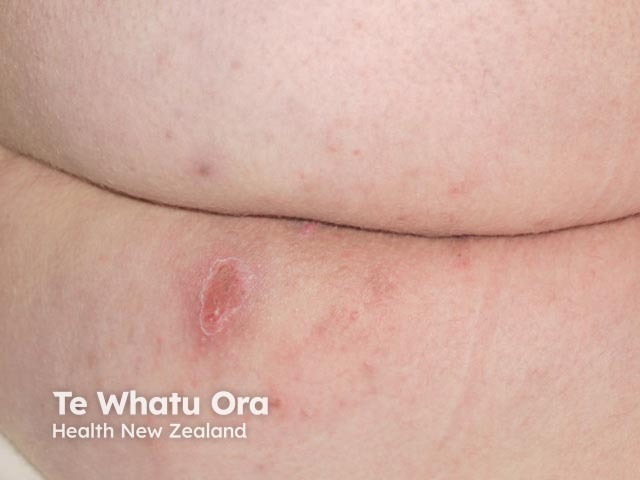
Frictional furuncle on the buttock
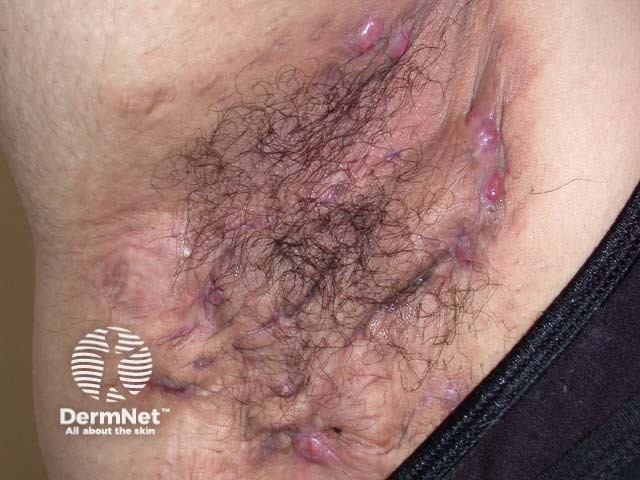
Scarring folliculitis
View more pictures of hidradenitis suppurativa
How is the severity of hidradenitis suppurativa assessed?
Disease severity and extent is measured by clinical and ultrasound assessment at the time of diagnosis and when monitoring response to treatment. There are a number of severity scales for HS [see guidelines for Hidradenitis suppurativa: severity assessment].
The Hurley system, the most widely used assessment tool, describes three clinical stages.
- Stage I: solitary or multiple isolated abscess formation without sinus tracts or scarring.
- Stage II: Recurrent abscesses, single or multiple widely spaced lesions, with sinus tract formation.
- Stage III: Diffuse involvement of an area with multiple interconnected sinus tracts and abscesses.
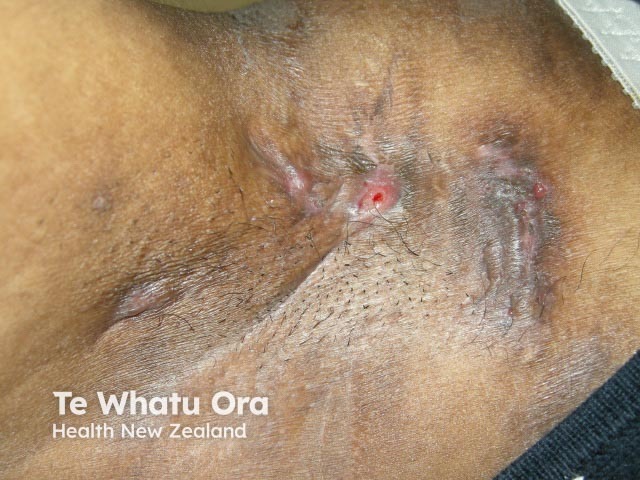
Hidradenitis suppurativa of axilla
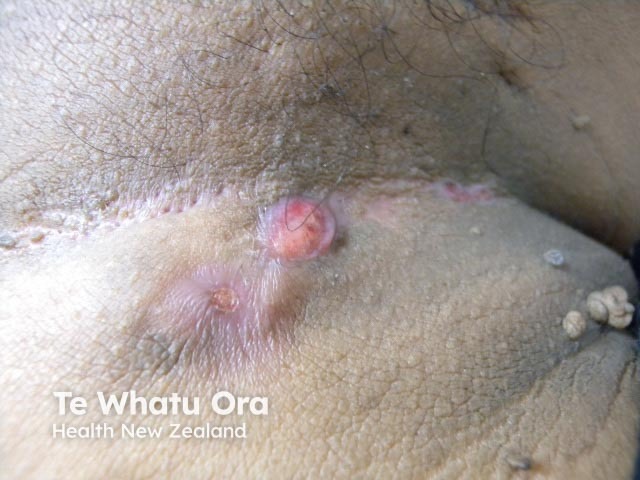
Hidradenitis suppurativa of groin
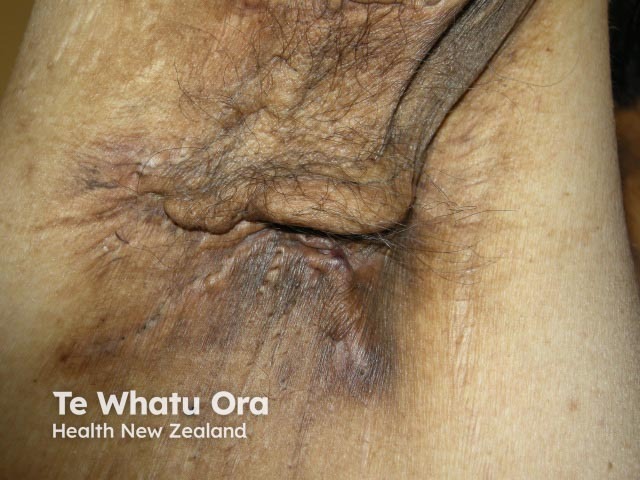
Hidradenitis suppurativa of axilla
What are the complications of hidradenitis suppurativa?
Complications of HS can include:
- Secondary infection
- Psychological effects and negative impact on quality-of-life
- Pyogenic granuloma
- Lymphoedema— female genital
- Squamous cell carcinoma— male anogenital
- Anaemia of chronic disease
- Small increased incidence of abdominal aortic aneurysm.
How is hidradenitis suppurativa diagnosed?
The diagnosis of acne inversa requires all three components of the triad to be met:
- Characteristic lesions
- Typical distribution
- Presence and recurrence of lesions.
Swabs for bacteriology are typically negative, which is a clue to diagnosis. Extensive investigations are rarely required. Investigations may be indicated to exclude a differential diagnosis, for possible complications, to identify comorbidities, or for planned treatment.
What is the differential diagnosis for hidradenitis suppurativa?
Differential diagnoses for hidradenitis suppurativa can include the following conditions.
- Staphylococcal skin infections, including abscesses, carbuncles, and furuncles.
- Cysts, like Bartholin cyst or epidermoid cyst.
- Cutaneous Crohn disease.
- Anogenital Crohn disease.
What is the treatment for hidradenitis suppurativa?
For a detailed evidence-based review of treatment for HS, see Management of hidradenitis suppurativa: an Australasian consensus statement. The following provides important general measures and additional medical treatments.
General measures
General measures for treating patients with hidradenitis suppurativa include:
- Weight loss
- Smoking cessation
- Loose fitting clothing
- Absorbent dressings
- Analgesics
- Management of anxiety and depression; including reassurance that the condition is not infectious or a result of poor hygiene.
Specific medical measures
Specific medical measures for treating hidradenitis suppurativa include:
Topical treatments
- Triclosan/benzoyl peroxide wash
- Topical clindamycin phosphate 1% with benzoyl peroxide
- Topical antibiotics: fusidic acid, dapsone, metronidazole.
Systemic treatments
Antibiotics for bacterial infections
- Short oral course for acute staphylococcal abscess
- Tetracyclines as a single agent
- Prolonged courses of at least three months of combination antibiotics: clindamycin plus rifampicin; tetracyclines plus rifampicin; fluoroquinolone plus metronidazole plus rifampicin
- Intravenous ertapenem - it is possible to home administer via an indwelling catheter for 12 weeks with improvement in both pain and HS severity index.
Other oral treatments
- Hormonal therapies: oestrogens, anti-androgen therapy, leuprolide acetate
- Immunomodulatory treatments: systemic steroids for acute flares, and steroid-sparing agents including ciclosporin, methotrexate, and azathioprine
- Biologics: adalimumab is the only biologic approved in Australia and New Zealand for treating hidradenitis suppurativa [see Tumour necrosis factor inhibitors]
- Others are under investigation in clinical trials
- Adalimumab and other biologics have been reported to paradoxically trigger acne inversa
- In several European countries, sekukinumab has received licencing
- Other systemic medical treatments used off-label: metformin, acitretin, dapsone, colchicine, and zinc gluconate.
Surgical and other procedural measures
- Incision and drainage of acute abscesses
- Local excision of persistent nodules, abscesses, and sinuses
- Deroofing and curettage of persistent abscesses and sinuses
- Radical excisional surgery of an entire affected area
- Laser ablation (CO2) of nodules, abscesses, and sinuses
- Laser/light hair removal.
What is the outcome for hidradenitis suppurativa?
Hidradenitis suppurativa tends to improve in pregnancy in those who usually have flares during menstruation. Normal vaginal delivery is possible unless the patient has extensive painful genital lesions.
HS is a chronic scarring condition. Spontaneous remission may occur with time, but scarring persists.
Early diagnosis and treatment are required to minimise lasting damage.
Bibliography
- Faivre C, Villani AP, Aubin F, et al. Hidradenitis suppurativa (HS): an unrecognized paradoxical effect of biologic agents (BA) used in chronic inflammatory diseases. J Am Acad Dermatol. 2016;74(6):1153–9. doi:10.1016/j.jaad.2016.01.018. PubMed
- Goldburg SR, Strober BE, Payette MJ. Hidradenitis suppurativa: epidemiology, clinical presentation, and pathogenesis. J Am Acad Dermatol. 2020;82(5):1045–58. doi:10.1016/j.jaad.2019.08.090. PubMed
- Goldburg SR, Strober BE, Payette MJ. Hidradenitis suppurativa: current and emerging treatments. J Am Acad Dermatol. 2020;82(5):1061–82. doi:10.1016/j.jaad.2019.08.089. PubMed
- Kimball AB, Jemec GBE, Alavi A, et al. Secukinumab in moderate-to-severe hidradenitis suppurativa (SUNSHINE and SUNRISE): week 16 and week 52 results of two identical, multicentre, randomised, placebo-controlled, double-blind phase 3 trials [published correction appears in Lancet. 2024 Feb 17;403(10427):618]. Lancet. 2023;401(10378):747-61. PubMed
- Kohorst JJ, Baum CL, Otley CC, et al. Surgical management of hidradenitis suppurativa: outcomes of 590 consecutive patients. Dermatol Surg. 2016;42(9):1030–40. doi:10.1097/DSS.0000000000000806. PubMed
- Lee JH, Kwon HS, Jung HM, Kim GM, Bae JM. Prevalence and comorbidities associated with hidradenitis suppurativa in Korea: a nationwide population-based study. J Eur Acad Dermatol Venereol. 2018;32(10):1784–90. doi:10.1111/jdv.15071. PubMed
- Lim SYD, Oon HH. Systematic review of immunomodulatory therapies for hidradenitis suppurativa. Biologics. 2019;13:53–78. doi:10.2147/BTT.S199862. PubMed
- Mastacouris N, Midgette B, Strunk A, Garg A. Precocious Puberty Among Children and Adolescents With Hidradenitis Suppurativa. JAMA Dermatol. 2024;160(11):1245–1246. PubMed
- Nosrati A, Ch'en PY, Torpey ME, et al. Efficacy and Durability of Intravenous Ertapenem Therapy for Recalcitrant Hidradenitis Suppurativa. JAMA Dermatol. 2024;160(3):312–8. PubMed
- Ring HC, Thorsen J, Saunte DM, et al. The follicular skin microbiome in patients with hidradenitis suppurativa and healthy controls. JAMA Dermatol. 2017;153(9):897–905. doi:10.1001/jamadermatol.2017.0904. PubMed
- Schrader AM, Deckers IE, van der Zee HH, Boer J, Prens EP. Hidradenitis suppurativa: a retrospective study of 846 Dutch patients to identify factors associated with disease severity. J Am Acad Dermatol. 2014;71(3):460–7. doi:10.1016/j.jaad.2014.04.001. PubMed
- van der Zee HH, Boer J, Prens EP, Jemec GB. The effect of combined treatment with oral clindamycin and oral rifampicin in patients with hidradenitis suppurativa. Dermatology. 2009;219(2):143–7. doi:10.1159/000228337. PubMed
- Vossen AR, van Straalen KR, Prens EP, van der Zee HH. Menses and pregnancy affect symptoms in hidradenitis suppurativa: a cross-sectional study. J Am Acad Dermatol. 2017;76(1):155–6. doi:10.1016/j.jaad.2016.07.024. PubMed
-
Wendland, Z., Rypka, K., Herzog, C., Greenlund, L., Fulk, T., Gravely, A., Westanmo, A., Garg, A., & Goldfarb, N. (2025). Prevalence of abdominal aortic aneurysm in patients with hidradenitis suppurativa in the Veterans Affairs Health Care System. British Journal of Dermatology, 192(1), 160–162. doi:10.1093/bjd/ljae325. Journal
On DermNet
- Hidradenitis suppurativa images
- Follicular occlusion syndrome
- Hidradenitis suppurativa: severity assessment
- Management of hidradenitis suppurativa: an Australasian consensus statement
- Smoking and its effects on the skin
Other websites
- Global HS COVID-19 Registry — Health professionals complete de-identified case histories of patients with hidradenitis suppurativa with confirmed or suspected COVID-19
- HS-Online for NZ
- Hidradenitis suppurativa US National Library of Medicine Genetics Home Reference
- Hidradenitis Suppurativa — Medline Plus
- HS-online
- The Hidradenitis Suppurativa Trust
- HS-USA Support Group
- Hidradenitis Suppurativa Foundation, Inc
- Hidradenitis Suppurativa Awareness — Facebook Group — Australia
- Hidradenitis Suppurativa Australia/New Zealand Facebook group
- Dermatologic Manifestations of Hidradenitis Suppurativa — Medscape
- Hidradenitis Suppurativa — British Association of Dermatologists
- Adalimumab for treating moderate to severe hidradenitis suppurativa — NICE technology appraisal guidance, June 2016
- Hidradenitis suppurativa and diet: What's recommended? — Mayo Clinic
- Hidradenitis suppurativa, diet, and PCOS — PCOS Nutrition Center
- Hidradenitis suppurativa — American Academy of Dermatology
- Systematic reviews on hidradenitis suppurativa — University of Nottingham
