Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: Brendon WH Lee, Medical Student, Faculty of Medicine, University of New South Wales, Sydney, NSW, Australia. DermNet New Zealand Editor-in-chief: A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand. August 2017. Copy editors: Maria McGivern/Gus Mitchell. October 2017.
Introduction Demographics Causes Symptoms Clinical features Diagnosis Differential diagnoses Treatment
Autoimmune disease (bullous) diseases usually present with blistering and erosions of the skin. They can also involve mucous membranes including the eye, mouth and gastrointestinal system.
Ocular involvement in autoimmune blistering diseases has been reported to occur both before and after the onset of skin lesions [1,2].
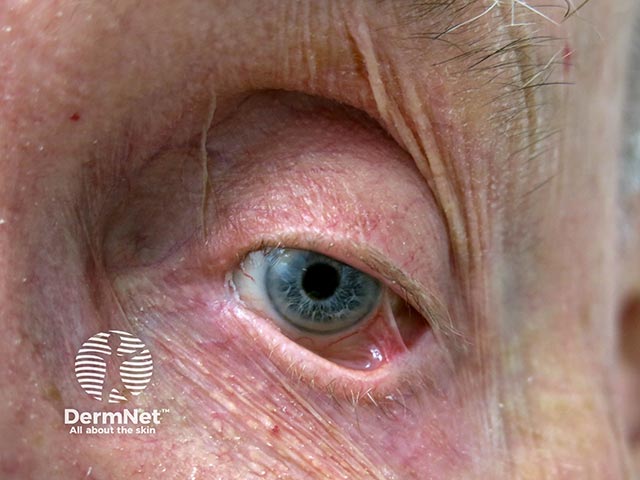
Symblepharon due to cicatricial pemphigoid
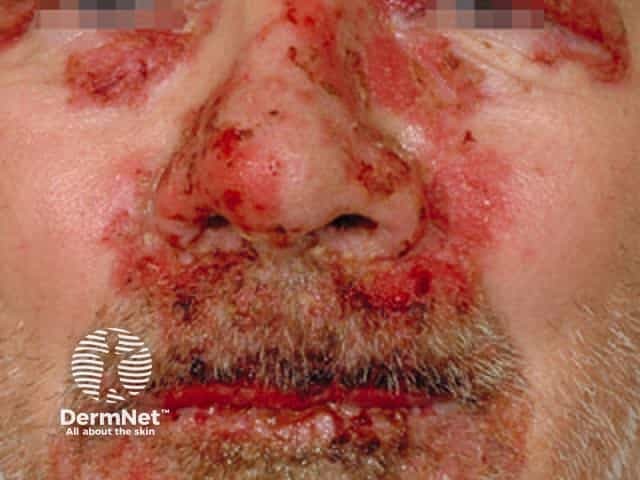
Pemphigus
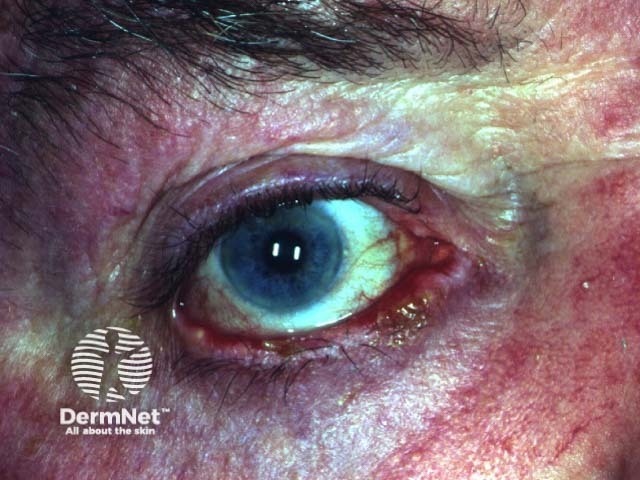
Blepharoconjunctivitis due to pemphigus vulgaris
Eye involvement affects people with autoimmune blistering skin diseases to a varying degree. It is seen most commonly in:
While ocular involvement in bullous pemphigoid, pemphigus foliaceus, and dermatitis herpetiformis has also been reported, it is much less common.
Autoimmune disease arises from a combination of environmental triggers and genetic susceptibility. Ocular involvement is thought to be due to biochemical and ultrastructural similarities common to the skin and cornea [3], which are both embryonically derived from the surface ectoderm [4].
The initial stage of ocular involvement is autoimmune-induced conjunctival inflammation.
Complications vary in frequency and severity among the different types of autoimmune blistering diseases, but all have the potential for serious morbidity and can threaten sight.
Blistering diseases mainly affect the eyelids, conjunctiva, and cornea. The disease may initially arise in one eye but generally progresses to affect both eyes. Patients may experience:
Patients may be asymptomatic even with advanced ocular signs [6].
The clinical signs of autoimmune blistering diseases affecting the eye are due to progressive chronic cicatrising (scarring) conjunctivitis.
Other common signs in early disease include:
Common eyelid complications include:
Epithelial defects of the cornea may progress to ulceration, scarring, and secondary bacterial infection. End-stage ocular involvement is characterised by:
The clinical findings and complications of ocular involvement often overlap between the different types of autoimmune blistering skin diseases. Spontaneous remissions are rare.
Ocular involvement should be suspected in patients with autoimmune blistering diseases. Early detection and management are vital to prevent sequelae such as irreversible vision loss.
Evaluation by an ophthalmologist is highly recommended as part of routine multidisciplinary care. This will usually involve a thorough history, and:
Clinical diagnosis is usually confirmed by immunopathology.
Diseases that may have similar ocular manifestations to autoimmune bullous diseases include:
These can be differentiated from ocular involvement in autoimmune bullous diseases by a careful history, a complete review of the patient's system, an examination and immunopathological investigations [9].
Treatment of ocular autoimmune blistering diseases is individualised, based on age, disease severity, and other sites of involvement [7]. The primary aim of treatment is to control ocular inflammation and prevent complications or progression to irreversible scarring and blindness. Once controlled, the goal is to taper doses of medication until a minimal maintenance dose or drug-free remission can be attained. Close collaboration between the treating dermatologist and ophthalmologist is critical.
Systemic corticosteroids (eg, oral prednisone or prednisolone) are the first-line therapy for treating ocular involvement in autoimmune blistering skin diseases [11]. Due to the significant toxicity of corticosteroids at the high doses required, other immune-suppressive/regulatory therapies are added, such as:
Tetracyclines are used to treat secondary corneal infections and blepharoconjunctivitis.
Treatments are continued long term and may require regular monitoring, due to potential side effects.
Surgery is rarely indicated in early disease and can induce exacerbation or progression when performed on inflamed eyes [13]. Surgical intervention should be delayed until the eyes are no longer inflamed and progression has stabilised.