Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Authors: Dr Ian Coulson, Consultant Dermatologist, Burnley, Lancashire, UK. April 2022. Previous author: Dr Amanda Oakley, Dermatologist, New Zealand, 1997. Copy edited by Gus Mitchell.
Introduction
Demographics
Clinical features
Variation in skin types
Types
Differential diagnosis
Investigation
Treatment
E-lecture
Dermatitis refers to a group of itchy inflammatory conditions characterised by epidermal changes.
Dermatitis can be classified in a variety of ways. It may be classified by:
In many cases, various factors may all act as underlying triggers together (allergic, irritant, and endogenous factors, especially in hand dermatitis).
The terms dermatitis and eczema are often used interchangeably. All eczema is a dermatitis, but not all dermatitis is eczema.
The term dermatitis is sometimes mistakenly attributed to mean an eczema induced by an occupational factor; this is erroneous.
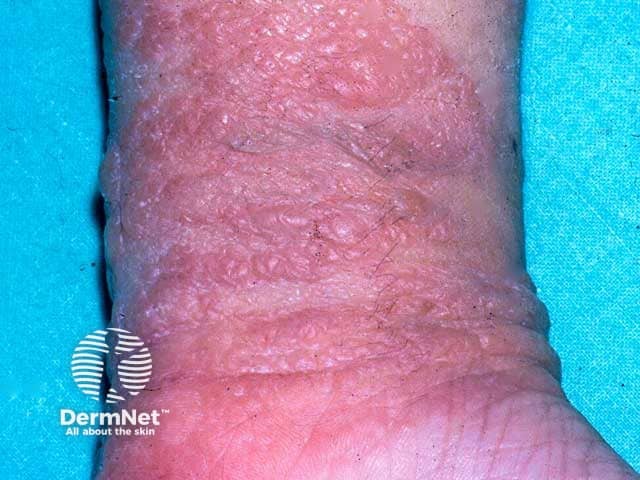
Acute weepy contact dermatitis due to sticking plaster allergy
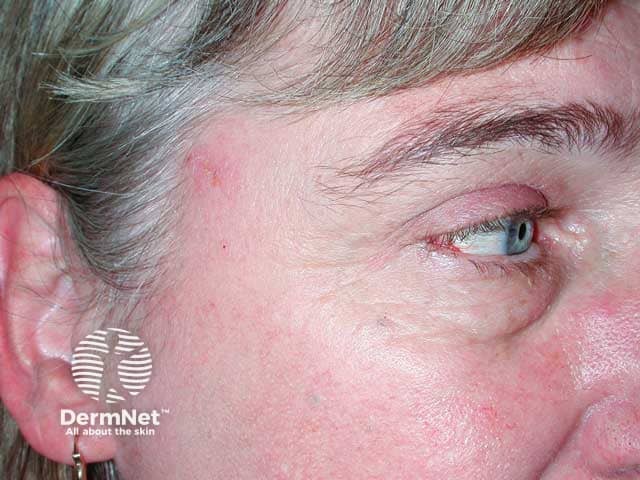
Allergic contact dermatitis due to nickel in the sides of her spectacle frame
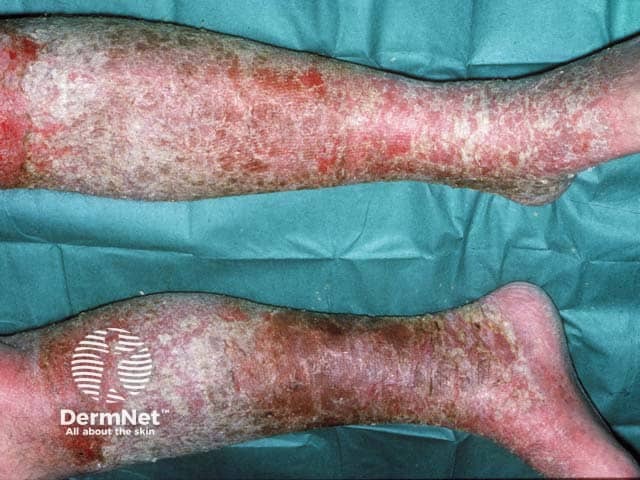
Gravitational eczema compounded by a contact allergy to a bandage constituent
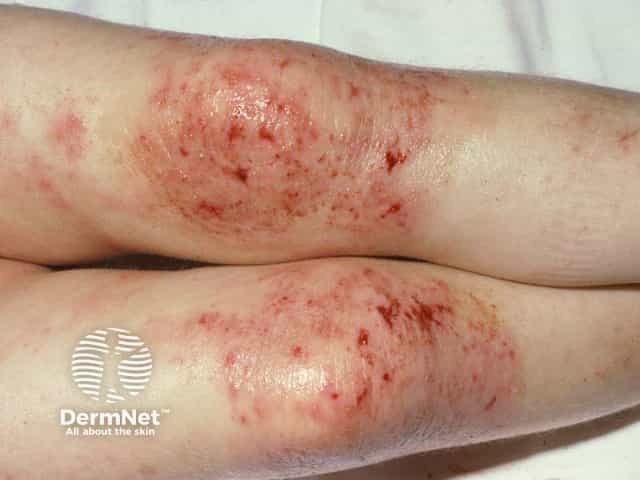
Excoriated acute eczema on the extensor aspects of the knees (reverse pattern)
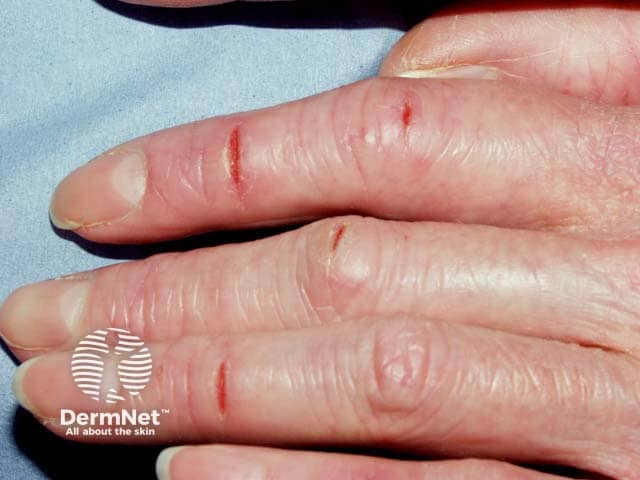
Fissuring over the knuckles in atopic dorsal hand eczema
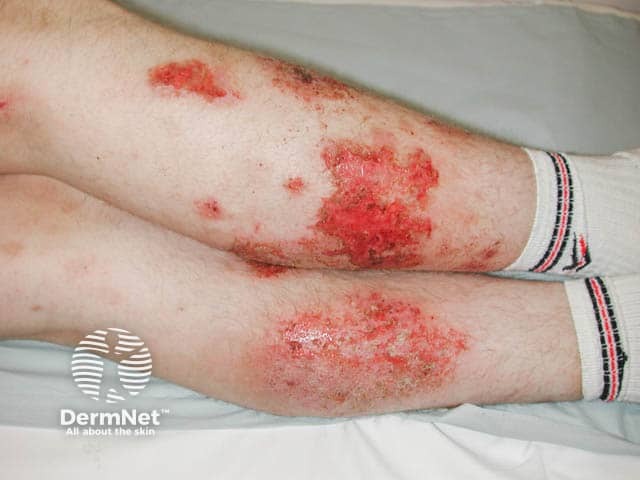
Weepy lesions of discoid eczema on the legs
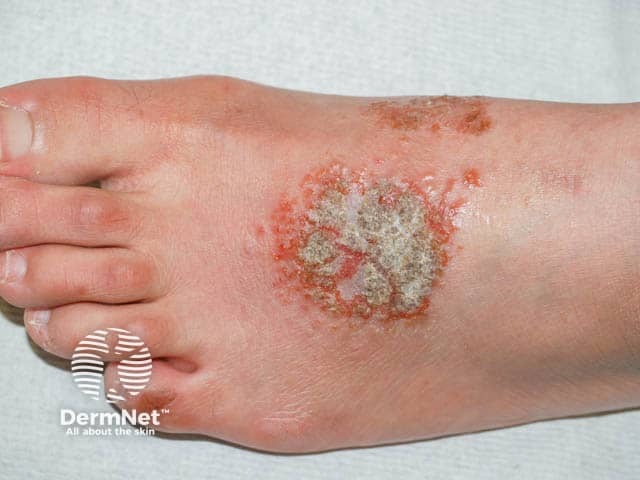
Weepy and impetigenised discoid eczema on the foot
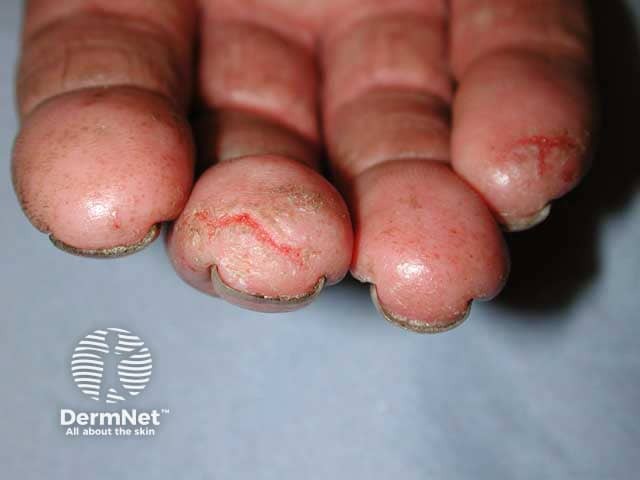
Fissuring, hyperkeratosis and vesiculation in chronic fingertip dermatitis
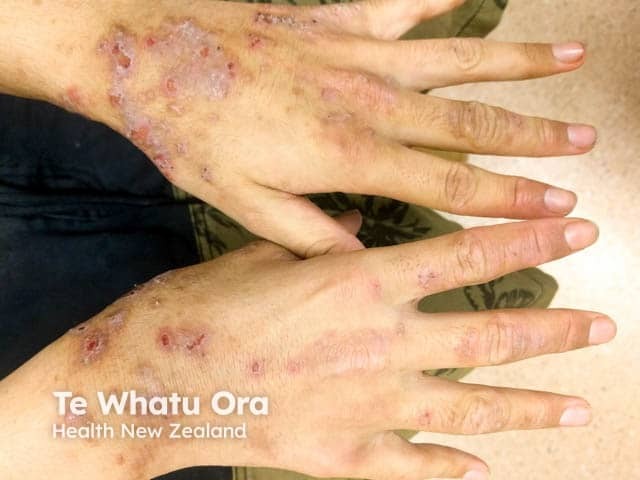
Discoid pattern of eczema on the dorsal hands

Hand eczema on the back of the hand - mixture of irritant factors in this atopic person
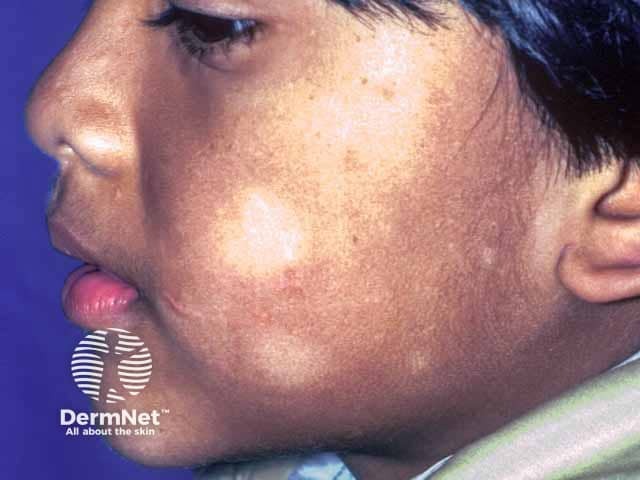
Hypopigmentation and fine scale on the cheeks in pityriasis alba
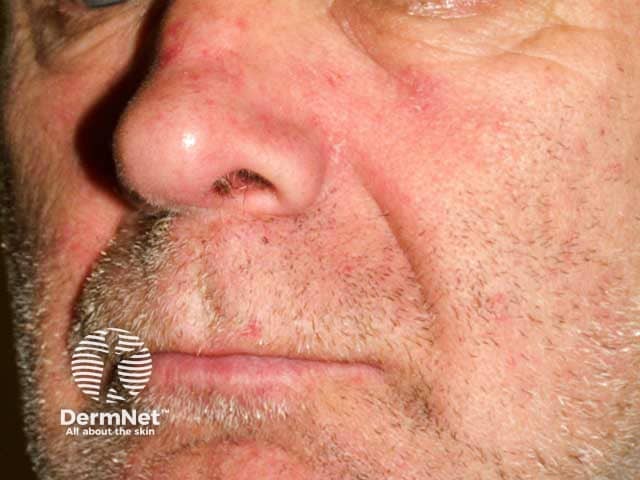
Cheek and nasolabial fold redness and scaling in seborrhoeic dermatitis
Dermatitis is common, affecting about one in every five persons at some stage in their life.
Different types of dermatitis are more frequent at different stages of life, for example:
There are no consistent racial factors influencing disease frequency.
Dermatitis may be either acute or chronic, and although the mechanism by which the dermatitis develops may be the same, the appearances may be starkly different.
Redness may be more difficult to appreciate in darker skin types.
Post-inflammatory hypo- and hyperpigmentation are more frequent in darker skin types.
Exogenous dermatitis is the result of an external factor or insult that induces skin inflammation. Common causes include:
Endogenous dermatitis occurs because of often ill-understood internal factors. Common types include:
A detailed history and examination may be all that is required to make an accurate diagnosis.
The following investigations may sometimes be needed:
General principles are covered here. Specific management of specific types of dermatitis are detailed on the relevant pages.