Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Autoimmune/autoinflammatory Rashes
Authors: Dr Helen Gordon, Dermatology Registrar, New Zealand. Adjunct A/Prof. Amanda Oakley, Dermatologist, New Zealand. July 2019. Minor update Dr Ian Coulson, Dermatologist, June 2023.
Introduction
Demographics
Causes
Clinical features
Complications
Diagnosis
Differential diagnoses
Treatment
Outcome
Subacute cutaneous lupus erythematosus (SCLE) is a subtype of cutaneous lupus erythematosus. It presents as a widespread non-scarring photosensitive rash.
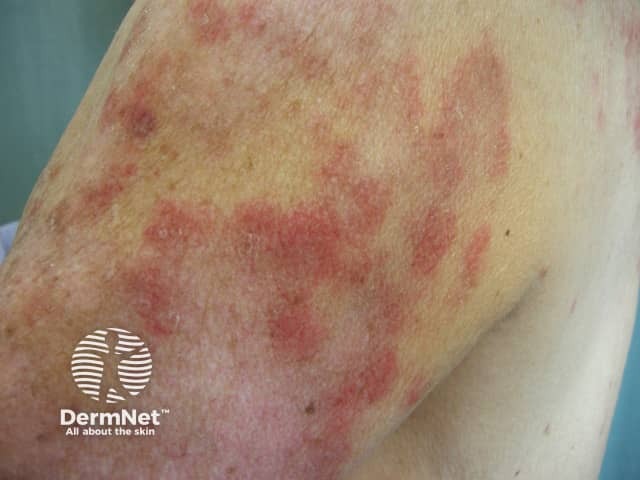
Drug-induced subacute lupus erythematosus
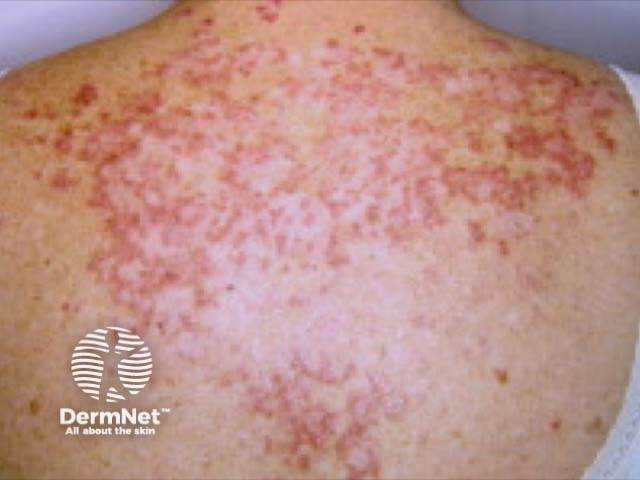
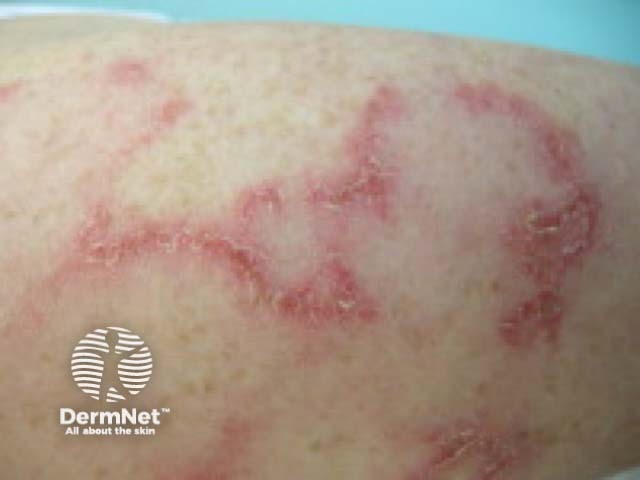
See more images of cutaneous lupus erythematosus.
SCLE affects about 10% of all patients with lupus.
SCLE is due to genetic and environmental factors.
SCLE is associated with the human leukocyte antigen (HLA)-A1-B8-DR3-DQ2-DRw52-C4null ancestral haplotypes. Other genetic associations include:
Immune tolerance is lost or autoimmunity develops through exposure to environmental triggers such as exposure to ultraviolet radiation (UVR) or photosensitising drugs.
Exposure to UVR results in increased expression of the Ro/SSA antigen on the surface of keratinocytes, binding the anti-Ro/SSA antibody and leading to the disease.
It is estimated 20-40% of cases of SCLE are drug-induced. The incubation time widely varies from a few days (such as in the case of the chemotherapy agents capecitabine and paclitaxel) to years before the onset of the rash (eg, a case was reported to arise 5 years after starting a thiazide diuretic).
The drugs most commonly associated with SCLE are:
Other drugs that may cause SCLE include:
Malignancy: there are increasing reports of SCLE being temporally associated with underlying cancers, including carcinoma of the lung, oesophagus, prostate, cholangiocarcinoma, and B-cell lymphoma.
SCLE most often presents as a non-scarring papulosquamous eruption.
Other lupus-associated findings in patients with SCLE include:
Drug-induced lupus can be indistinguishable from the non-drug-induced form of SCLE. Specific features of drug-induced SCLE include:
Around 50% of patients with SCLE meet the American College of Rheumatology criteria for the diagnosis of systemic lupus erythematosus (SLE).
A pregnant woman who is Ro/SSA antibody-positive has a risk of delivering an infant suffering from neonatal lupus erythematosus (8–10%) and congenital heart block (1–2%).
SCLE can be diagnosed clinically, supported by the results of blood tests and a skin biopsy.
The histology on biopsy can resemble other forms of cutaneous lupus.
Drug-induced SCLE and non-drug-induced SCLE cannot be distinguished on histology.
The differential diagnosis for SCLE includes other types of cutaneous lupus, especially:
Other skin conditions that may be considered include:
Sun protection is crucial.
Topical therapy may include:
The main treatment for SCLE is an antimalarial drug, particularly hydroxychloroquine. Antimalarial drugs are less effective in smokers.
In approximately 25% of cases, another agent is required, such as:
SCLE generally responds well to treatment, although it may flare up again each summer.
Approximately 10–15% of patients with SCLE develop SLE, including renal and neurological involvement.
Drug-induced SCLE can be slow to resolve on stopping the causative drug (one study found resolution took a mean of 7 weeks).