Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Systemic lupus erythematosus — extra information
Systemic diseases Autoimmune/autoinflammatory
Systemic lupus erythematosus
Author: Hon A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, February 2015.
Introduction
Causes
Demographics
Cutaneous features
Systemic features
Diagnosis
Treatment
Outlook
Introduction
Lupus erythematosus (LE) is a group of diverse, persistent autoimmune inflammatory diseases.
Systemic lupus erythematosus (SLE) affects several organs (such as skin, joints and kidneys) and blood tests reveal circulating autoantibodies. The clinical features of SLE are highly variable and may overlap with other diseases and conditions. Skin involvement or cutaneous lupus (CLE) affects 80% of patients with SLE.
SLE is sometimes called acute lupus erythematosus, and the cutaneous features may be described as acute cutaneous lupus.
What causes systemic lupus erythematosus?
Factors leading to SLE include:
- Genetic predisposition, including haplotype HLA-B8, -DR3
- Exposure to sunlight
- Viral infection, particularly Epstein-Barr virus
- Hormones
- Toxins such as cigarette smoke
- Drugs in drug-induced LE
- Emotional upset.
The manifestations of SLE are due to loss of regulation of the patient's immune system.
- Nuclear proteins are not processed properly.
- Nuclear debris accumulates within the cell.
- This leads to the production of autoantibodies against nuclear proteins.
- Immune complexes are not removed.
- The complement system is activated.
- Inflammation leads to cell and tissue injury.
Who gets systemic lupus erythematosus?
SLE can affect males and females of any age. Every year about 2–7 new cases are diagnosed in a population of 100,000 people. SLE is much more common in females than males, and onset is most often between the ages of 15 and 45 years.
SLE is more prevalent and more severe in smokers. Smoking also reduces the effectiveness of antimalarials and other therapies.
Autoantibodies can be present in people that have no manifestation of the disease.
What are the cutaneous features of systemic lupus erythematosus?
About 80% of patients with SLE have skin involvement (cutaneous LE), and it is the first sign of SLE in about one-quarter of them. It can present as LE-specific or LE-nonspecific manifestations. LE-specific lesions tend to be induced or aggravated by exposure to ultraviolet radiation and are localised in sun-exposed sites such as the face, neck, V of the neck and upper back.
Specific cutaneous SLE
Cutaneous lupus (CLE) has specific acute, subacute and chronic manifestations.
- Typically, SLE presents with acute CLE.
- About half of patients with subacute cutaneous LE develop mild SLE
- Only 5% of patients with chronic CLE have SLE, as CLE presents as a skin problem without the involvement of other organs.
Acute CLE
- Central face malar or "butterfly" violaceous erythema with a sharp cutoff at lateral margins, resolves without scarring (may result in persistent telangiectasia)
- Bullous systemic lupus erythematosus: a blistering rash, if severe, this may resemble toxic epidermal necrolysis
- A maculopapular rash resembling morbilliform drug eruption
- Mucosal erosions and ulcerations (lips, nose, mouth, genitals)
- Photosensitivity: lupus rashes are mainly on sun-exposed sites. Photosensitivity can be mild to very severe with the rash appearing after minimal light exposure.
- Diffuse hair loss (nonscarring alopecia) with brittle hair shafts
Subacute cutaneous LE
- Flat, scaly patches resembling psoriasis, often in a network pattern
- Annular (ring-shaped) polycyclic (overlapping circular) lesions
- Lesions resolve with minimal scarring
- Affects trunk and arms
- Flares on exposure to the sun, but usually spares face and hands
Chronic CLE
- Chronic CLE affects 25% of patients with SLE
- Classic discoid lupus is most common: indurated hyperpigmented plaques
- Localised (above the neck in 80%) or generalised (above and below the neck in 20%)
- Hypertrophic (warty) lupus
- Tumid lupus
- Lupus panniculitis/profundus
- Mucosal lupus (lips, nose, mouth, genitals)
- Chilblain lupus erythematosus
- Discoid lupus/lichen planus overlap
- Discoid lesions and panniculitis resolve with scarring
Acute cutaneous lupus erythematosus
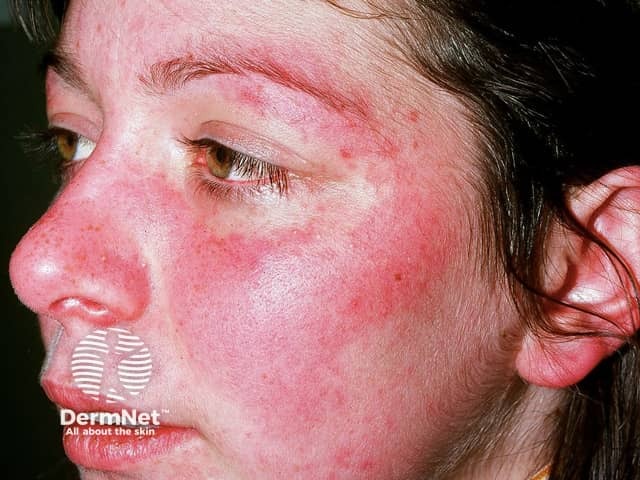
Butterfly rash
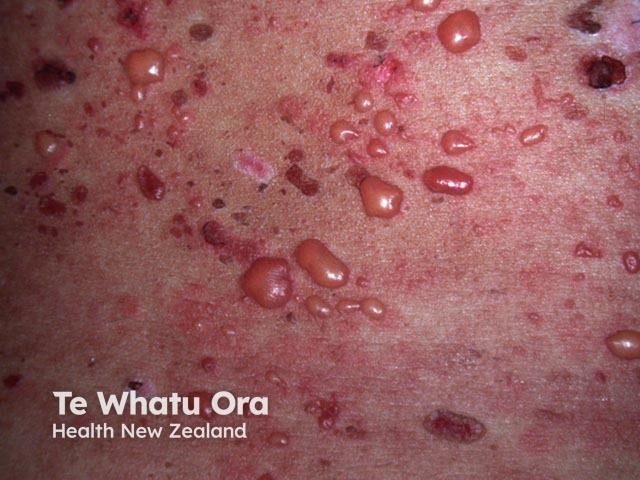
Bullous LE
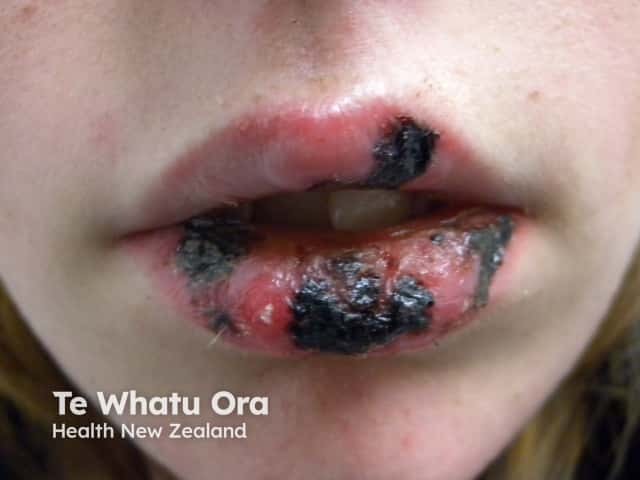
Mucosal ulceration
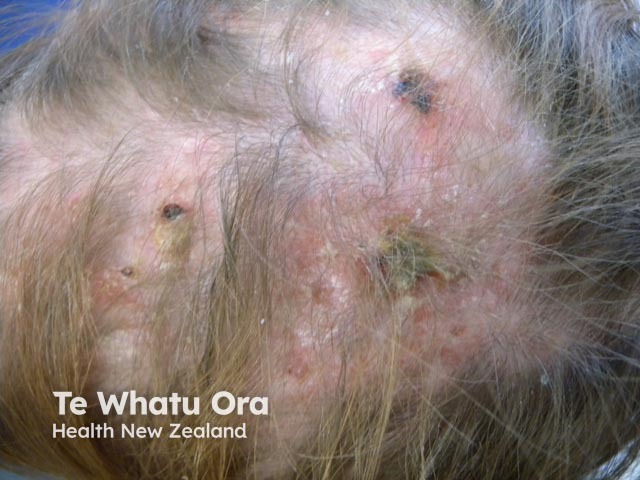
Diffuse hair loss
Subacute cutaneous lupus in SLE
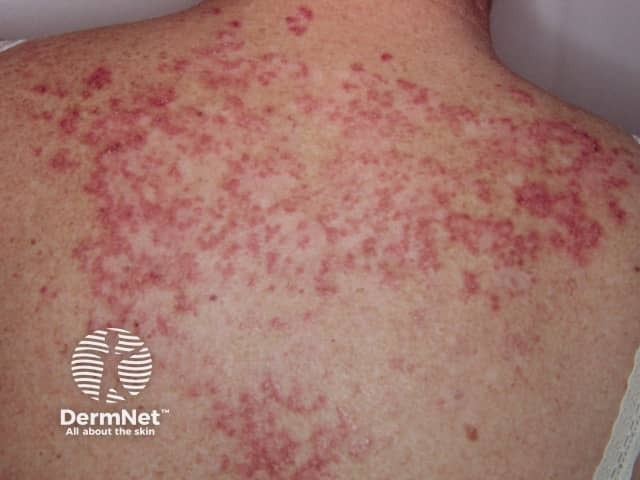
Systemic lupus erythematosus
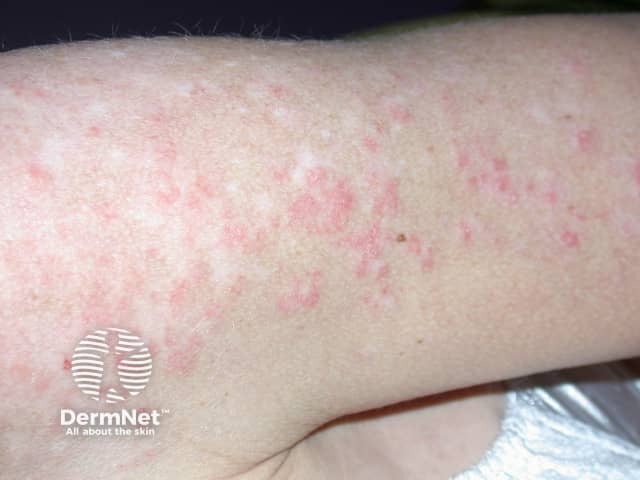
Systemic lupus erythematosus
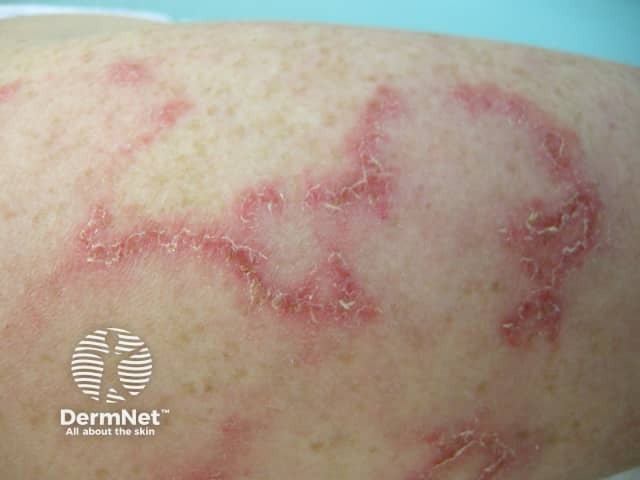
Systemic lupus erythematosus
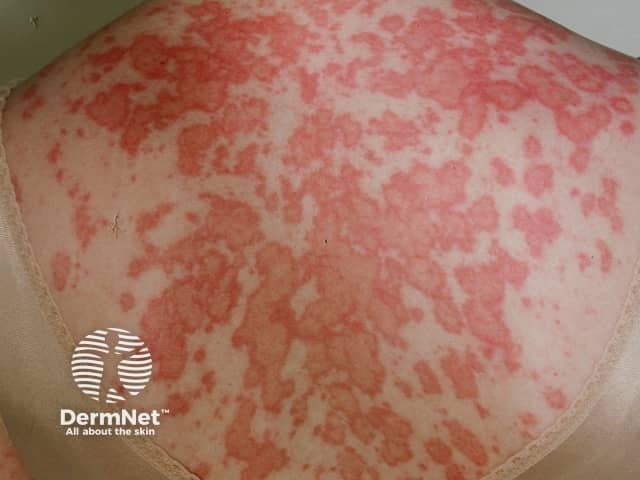
Systemic lupus erythematosus
See more images of cutaneous lupus erythematosus.
Chronic cutaneous lupus
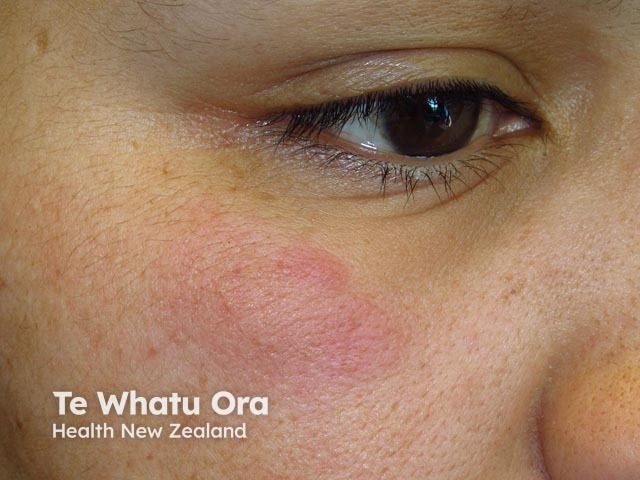
Tumid CLE
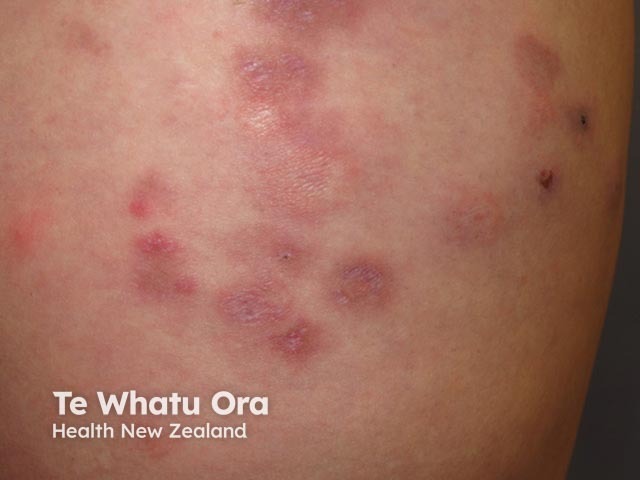
Lupus profundus
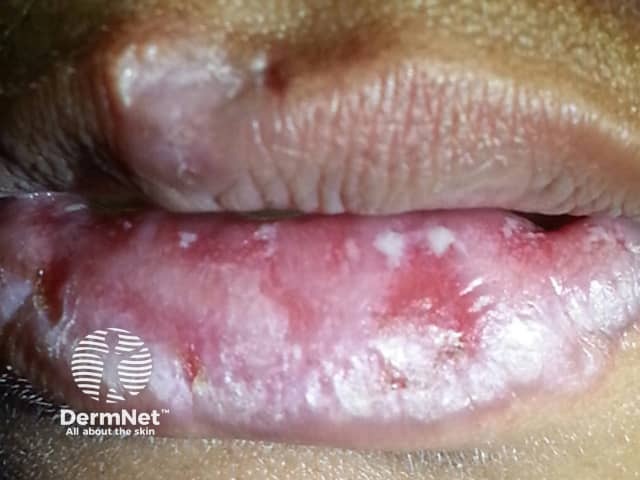
Mucosal CLE
Nonspecific cutaneous SLE
Nonspecific cutaneous SLE refers to features relating to underlying illness rather than an autoimmune attack. These features may occur in other connective tissue and autoimmune diseases.
- Nail fold capillary telangiectasia
- Raynaud phenomenon (white fingers and toes on exposure to the cold)
- Vasculopathy of tips of digits (occlusion of small blood vessels by thrombus)
- Diffuse hair thinning without brittle hair
- Urticaria, which may be neutrophilic on biopsy
- Cutaneous vasculitis: palpable purpura or urticarial vasculitis
- Livedo reticularis (a network pattern of blood vessels) in 20–30% patients with SLE
- Papular mucinosis (deposits of mucin in the skin)
- Calcinosis cutis (deposits of calcium in the skin)
Nonspecific cutaneous lupus erythematosus
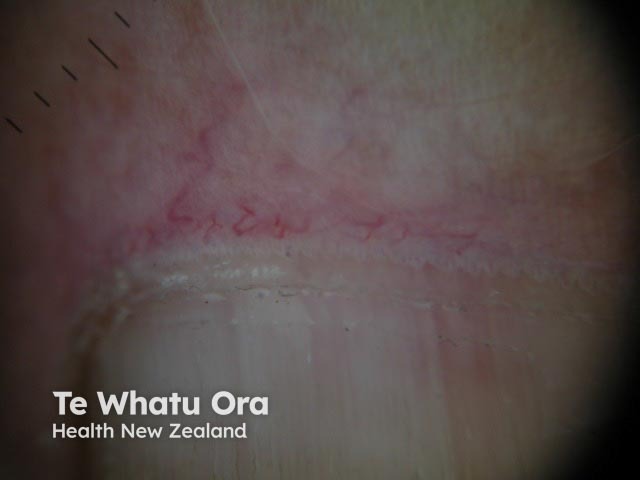
Nail-fold capillaries
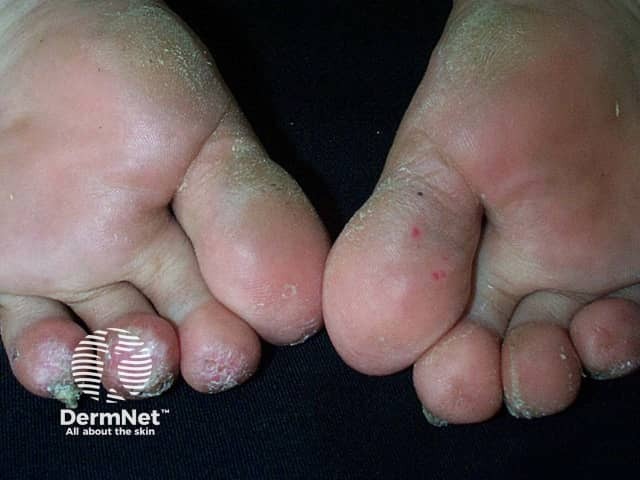
Vasculopathy
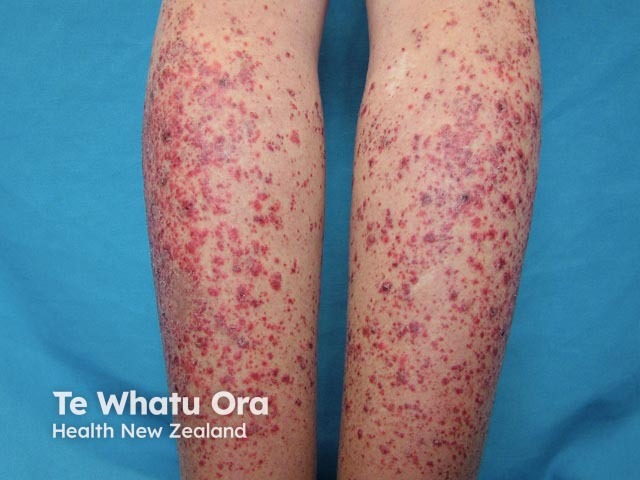
Palpable purpura
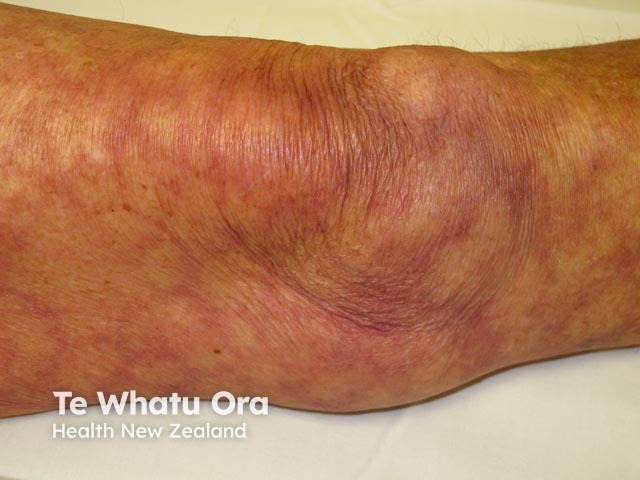
Livedo reticularis
What are the systemic features of systemic lupus erythematosus?
Numerous systemic features may occur in SLE and can result in critical illness.
- General: tiredness, malaise, chronic pain, fever with flares
- Joints: arthritis or synovitis causing swelling, pain and morning stiffness
- Lungs: pleurisy or pleural effusions
- Heart: pericarditis or pericardial effusions
- Kidneys: protein, casts in urine, glomerulonephritis
- Brain: seizures, psychosis, confusion
- Nervous system: mononeuritis multiplex, myelitis, peripheral neuropathy
- Blood: reduced numbers of red cells, white cells and platelets
How is systemic lupus erythematosus diagnosed?
SLE can be difficult to diagnose at times because of the great variety of presentations of the disease, and the presence of similar symptoms in people that do not have the disease. Several attempts have been made to help clinicians reach the diagnosis, including the American College of Rheumatology criteria for the classification of SLE (revised in 1997). In 2012, the criteria were revised by the Systemic Lupus International Collaborating Clinics (SLICC).[1]
Using the SLICC criteria, SLE is diagnosed if the patient has either of the following over time:
- Four criteria including ≥ one clinical criterion and ≥ one immunological criterion
- Biopsy-proven lupus nephritis and antinuclear antibodies or anti-double-stranded DNA antibodies
These criteria depend on history, clinical examination, exclusion of other causes of the symptoms, and the results of investigations—including blood tests and biopsy of the affected tissue. Four of the 17 SLICC criteria relate to the skin.
Clinical criteria
- Acute or subacute cutaneous lupus
- Chronic cutaneous lupus
- Oral ulcers
- Nonscarring alopecia
- Synovitis involving 2 or more joints
- Serositis involving lungs or heart
- Renal involvement
- Neurological involvement
- Haemolytic anaemia
- leukopenia or lymphopenia
- Thrombocytopenia
Immunological criteria
- Raised ANA level
- A raised anti-dsDNA antibody level
- Presence of anti-Sm
- Positive antiphospholipid antibody (lupus anticoagulant, false positive rapid plasma reagin, high-titre anticardiolipin antibody, positive anti–2-glycoprotein I)
- Low complement levels
- Positive direct Coombs’ test
* SLICC Systemic Lupus International Collaborating Clinics; ANA antinuclear antibody; anti-dsDNA anti-double-stranded DNA
Cutaneous Lupus Erythematosus Disease Area and Severity Index (CLASI)
The Cutaneous Lupus Erythematosus Disease Area and Severity Index (CLASI) was developed in an attempt to classify the severity of CLE. [2] A score of activity and damage due to the disease is calculated in each of 12 anatomical locations (refer to the original published paper for details).
The total activity score is made up of:
- The degree of redness (0–3) and scale (0–2)
- Mucous membrane involvement (0–1)
- Recent hair loss (0–1), nonscarring alopecia (0–3)
Total damage score is made up of:
- The degree of dyspigmentation (0–2), and scarring (0–2)
- Persistence of dyspigmentation more than 12 months doubles the dyspigmentation score
- Scalp scarring (0,3,4,5,6)
Biopsy findings
Patients with SLE often undergo skin biopsy.
- Acute CLE: nonspecific dermatitis.
- Subacute CLE: features of lupus noted in the epidermis and superficial dermis
- Chronic discoid CLE: typical features of lupus with atrophy and scarring
- Direct immunofluorescence is positive in sun-protected healthy skin in SLE
Blood tests
Multiple autoantibodies are typically present in SLE, often in high titre (see immunological criteria above). Relating to skin disease in SLE:
- About 70% of patients with subacute CLE have positive extractable nuclear antibodies anti-Ro (also called anti-SSA) and anti-La (also called anti-SSB).
- Anti Ro/La is also associated with Sjögren syndrome and risk of neonatal lupus erythematosus.
- Low serum complement in SLE has been associated with urticarial vasculitis and renal disease.
- Antiphospholipid antibodies are associated with livedo reticularis, thrombosis and pregnancy complications (antiphospholipid syndrome).
- Anti-annexin 1 antibodies may be a diagnostic marker for discoid CLE
Patients with SLE should also have renal, liver and thyroid function and markers of inflammation performed, such as C-reactive protein (CRP), immunoglobulins and rheumatoid factor.
Photoprovocation tests
Photoprovocation tests are sometimes carried out to confirm that a skin eruption is precipitated by exposure to particular wavelengths of ultraviolet or visible radiation.
Other tests
Other tests depend on which organ is affected. They may, for example, include:
- Urine tests for hyaline casts, creatinine, protein and blood
- Blood pressure
- Chest X-ray, ultrasound, CT and MRI scans
- Electrocardiograph (ECG) and echocardiography
- Nerve and muscle testing
- Ophthalmological examination
- Endoscopy of the gastrointestinal tract
- Kidney biopsy.
What is the treatment for systemic lupus erythematosus?
Preventative measures
The following measures are essential to reduce the chance of flares and organ damage.
- Careful protection from sun exposure using clothing, accessories and SPF 50+ broad-spectrum sunscreens. Sunscreens alone are not adequate.
- Smoking cessation
- Rest when needed.
Topical therapy
Intermittent courses of potent topical corticosteroids are important in the treatment of CLE. They should be applied accurately to the skin lesions.
The calcineurin inhibitors tacrolimus ointment and pimecrolimus cream can also be used.
Systemic therapy
Treatment of SLE depends on which are the predominant organs involved in the disease. Typically, any of the following drugs may be used alone or in combination.
- Systemic corticosteroids, such as prednisone or prednisolone. These are the mainstay of treatment in a seriously ill patient with acute LE.
- Hydroxychloroquine and other antimalarials—response rates are about 80% in CLE.
- Methotrexate—best response in subacute CLE and discoid CLE
- Immunosuppressives such as azathioprine, mycophenolate and cyclophosphamide
- Intravenous immunoglobulin
- Aspirin is recommended for antiphospholipid syndrome.
- Targeted biologic therapies under evaluation for SLE include anifrolumab, belimumab (intravenous and subcutaneous formulations were registered by FDA for use in SLE in 2017) and off-label rituximab, abatacept, tocilizumab and eculizumab.[3]
CLE is also sometimes treated with:
- Retinoids (isotretinoin and acitretin)
- Dapsone.
What is the outlook for systemic lupus erythematosus?
SLE leads to a chronic illness with flares and periods of remissions. In some patients, all signs of active disease resolve in time.
References
- Petri M, Orbai AM, Alarcón GS et al. Derivation and validation of the Systemic Lupus International Collaborating Clinics classification criteria for systemic lupus erythematosus. Arthritis Rheum 2012; 64: 2677–86. DOI: 10.1002/art.34473. PubMed PMID: 22553077; PubMed Central
- Albrecht J, Werth VP. Clinical outcome measures for cutaneous lupus erythematosus. Lupus 2010; 19: 1137–43. doi: 10.1177/0961203310370049. Review. PubMed PMID: 20693208; PubMed Central
- Belmont HM. Treatment of systemic lupus erythematosus – 2013 update. Bull Hosp Jt Dis 2013; 71: 208–13. Review. PubMed
- Systemic Lupus Erythematosus. Ferri's Clinical Advisor 2015. Ferri FF. 2015. Mosby.
On DermNet
- Images of systemic lupus erythematosus
- Cutaneous lupus erythematosus
- Subacute cutaneous LE
- Bullous systemic lupus erythematosus
- Chilblain lupus erythematosus
- Images of cutaneous lupus erythematosus
- Discoid lupus erythematosus
- Chilblain lupus erythematosus
- Pathology of discoid lupus erythematosus
- Drug-induced lupus erythematosus
- Connective tissue diseases – a course for health professionals
- Psychological effects of cutaneous lupus erythematosus
- Allergies explained
- Direct immunofluorescence
- Skin signs of rheumatic disease
- Indirect immunofluorescence
- Antimalarial medications in dermatology
- Neonatal lupus erythematosus
Other websites
- Do you have systemic lupus erythematosus (lupus, SLE) and are over 18 years of age? If so, please participate in Ameriderm's SLE symptom survey
- Lupus Foundation of America
- Lupus Support Group (New Zealand)
- Irish Lupus support group
- Lupus UK
- Lupus (Systemic Lupus Erythematosus) — emedicinehealth
- Systemic Lupus Erythematosus — Medscape Drugs & Diseases
- Systemic Lupus Erythematosus and Pregnancy — Medscape Drugs & Diseases
- Pediatric Systemic Lupus Erythematosus — Medscape Drugs & Diseases
- Bullous Systemic Lupus Erythematosus — Medscape Drugs & Diseases
- Genetics of Systemic Lupus Erythematosus — Medscape Drugs & Diseases
- Physical Medicine and Rehabilitation for Systemic Lupus Erythematosus — Medscape Drugs & Diseases
- Lupus — MedlinePlus
- Systemic lupus erythematosus — MedlinePlus
- Lupus — National Institute of Arthritis and Musculoskeletal and Skin Diseases
- Systemic lupus erythematosus — Genetics Home Reference
