Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Cutaneous squamous cell carcinoma — extra information
Cutaneous squamous cell carcinoma
Author: Honorary Associate Professor Amanda Oakley, Dermatologist, Hamilton, New Zealand, 1997. Updated December 2015.
Introduction
Demographics
Causes
Clinical features
Types
Classification by risk
Staging
Diagnosis
Treatment
Advanced and metastatic treatment
Prevention
Outlook
What is cutaneous squamous cell carcinoma?
Cutaneous squamous cell carcinoma (SCC) is a common type of keratinocyte cancer, or non-melanoma skin cancer. It is derived from cells within the epidermis that make keratin — the horny protein that makes up skin, hair and nails.
Cutaneous SCC is an invasive disease, referring to cancer cells that have grown beyond the epidermis. SCC can sometimes metastasise and may prove fatal.
Intraepidermal carcinoma (cutaneous SCC in situ) and mucosal SCC are considered elsewhere.
Who gets cutaneous squamous cell carcinoma?
Risk factors for cutaneous SCC include:
- Age and sex: SCCs are particularly prevalent in elderly males. However, they also affect females and younger adults.
- Previous SCC or another form of skin cancer (basal cell carcinoma, melanoma) are a strong predictor for further skin cancers.
- Actinic keratoses
- Outdoor occupation or recreation
- Smoking
- Fair skin, blue eyes, and blond or red hair
- Previous cutaneous injury, thermal burn, disease (eg, cutaneous lupus, epidermolysis bullosa, leg ulcer)
- Inherited syndromes: SCC is a particular problem with xeroderma pigmentosum, albinism, and epidermodysplasia verruciformis
- Other risk factors include ionising radiation, exposure to arsenic, immune suppression due to disease (eg, chronic lymphocytic leukaemia) or medicines, and use of some other medicines such as hydrochlorothiazide.
- Organ transplant recipients have an increased risk of developing SCC.
What causes cutaneous squamous cell carcinoma?
More than 90% of cases of SCC are associated with numerous DNA mutations in multiple somatic genes. Mutations in the p53 tumour suppressor gene are caused by exposure to ultraviolet radiation (UV), especially UVB (known as signature 7). Other signature mutations relate to cigarette smoking, ageing and immune suppression (eg, to drugs such as azathioprine). Mutations in signalling pathways affect the epidermal growth factor receptor, RAS, Fyn, and p16INK4a signalling.
Beta-genus human papillomaviruses (wart virus) are thought to play a role in SCC arising in immune-suppressed populations. β-HPV and HPV subtypes 5, 8, 17, 20, 24, and 38 have also been associated with an increased risk of cutaneous SCC in immunocompetent individuals.
What are the clinical features of cutaneous squamous cell carcinoma?
Cutaneous SCCs present as enlarging scaly or crusted lumps. They usually arise within pre-existing actinic keratosis or intraepidermal carcinoma.
- They grow over weeks to months
- They may ulcerate
- They are often tender or painful
- Located on sun-exposed sites, particularly the face, lips, ears, hands, forearms and lower legs
- Size varies from a few millimetres to several centimetres in diameter.
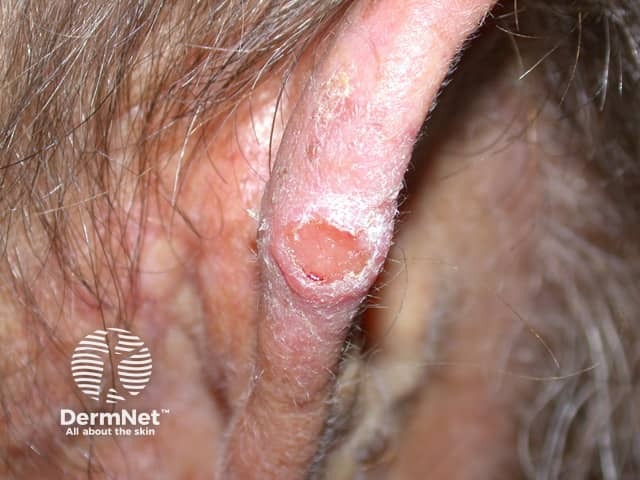
Squamous cell carcinoma
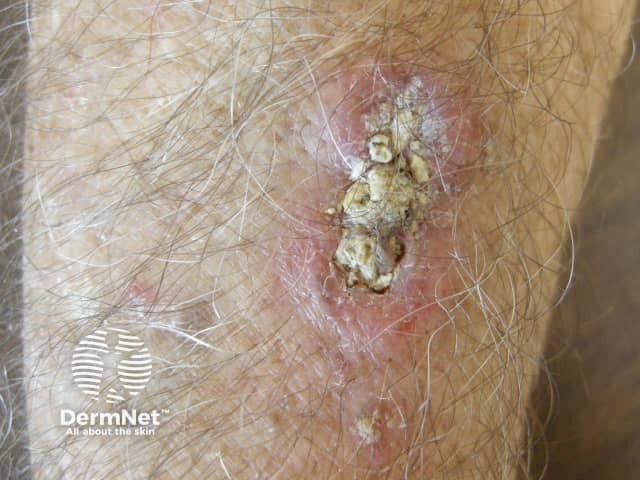
Squamous cell carcinoma
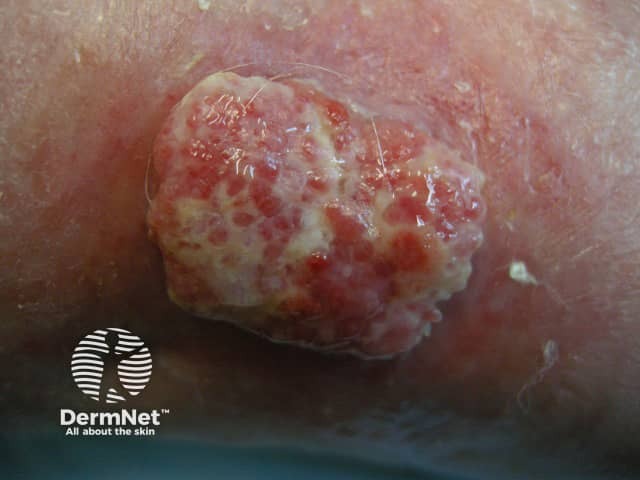
Squamous cell carcinoma
See more images of squamous cell carcinoma:
Cutaneous squamous cell carcinoma images
Types of cutaneous squamous cell carcinoma
Distinct clinical types of invasive cutaneous SCC include:
- Cutaneous horn — the horn is due to excessive production of keratin
- Keratoacanthoma (KA) — a rapidly growing keratinising nodule that may resolve without treatment
- Carcinoma cuniculatum (‘verrucous carcinoma’), a slow-growing, warty tumour on the sole of the foot
- Marjolin ulcer - a cutaneous SCC that has developed in a scar or chronic ulcer
- Multiple eruptive SCC/KA-like lesions arising in syndromes, such as multiple self-healing squamous epitheliomas of Ferguson-Smith and Grzybowski syndrome.
The pathologist may classify a tumour as well differentiated, moderately well differentiated, poorly differentiated or anaplastic cutaneous SCC. There are other variants.
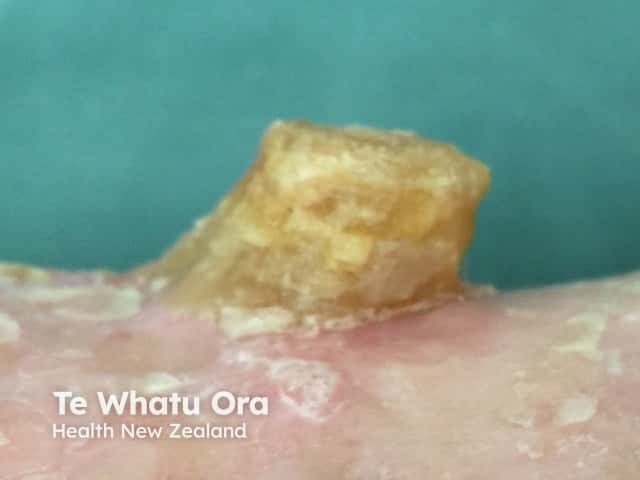
Cutaneous horn
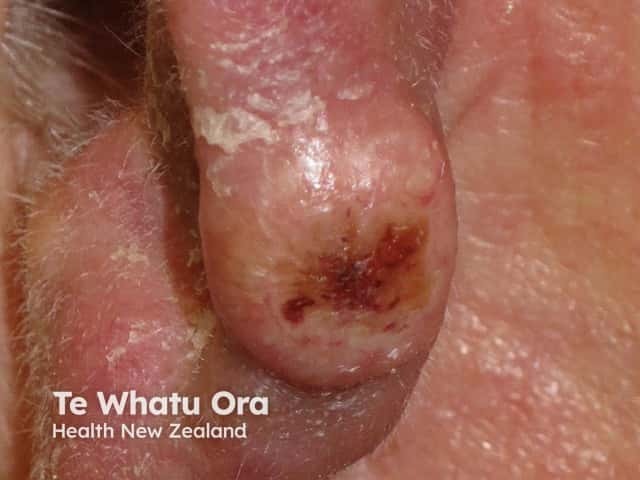
Keratoacanthoma
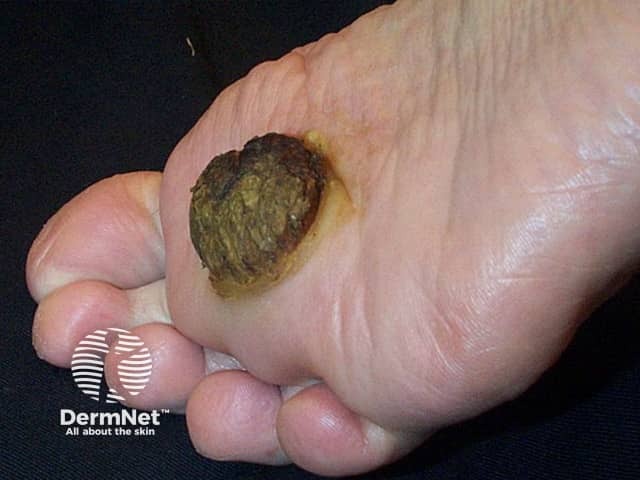
Carcinoma cuniculatum
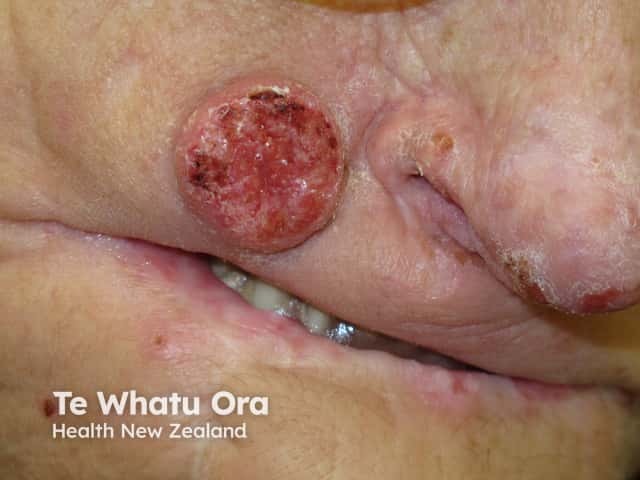
Squamous epithelioma of Ferguson-Smith
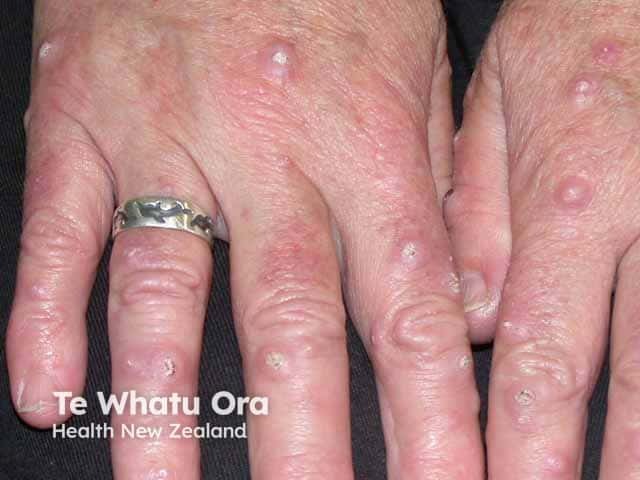
Grzybowski syndrome (GEKA-patient1)
Classification of squamous cell carcinoma by risk
Cutaneous SCC is classified as low-risk or high-risk, depending on the chance of tumour recurrence and metastasis. Characteristics of high-risk SCC include:
High-risk cutaneous squamous cell carcinoma has the following characteristics:
- Diameter greater than or equal to 2 cm
- Location on the ear, vermilion of the lip, central face, hands, feet, genitalia
- Arising in elderly or immune suppressed patient
- Histological thickness greater than 2 mm, poorly differentiated histology, or with the invasion of the subcutaneous tissue, nerves and blood vessels.
Metastatic SCC is found in regional lymph nodes (80%), lungs, liver, brain, bones and skin.
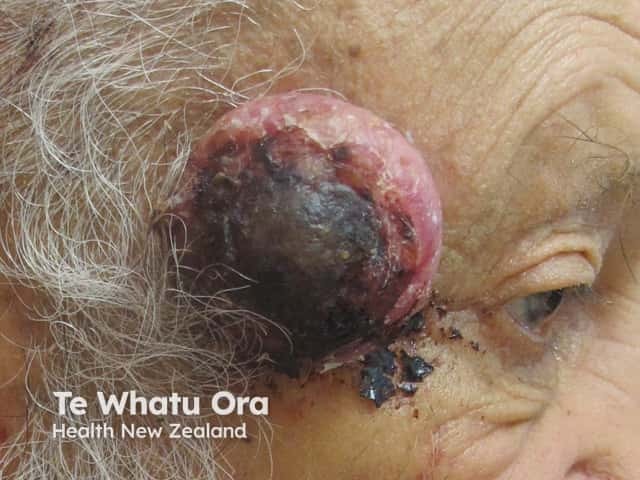
High-risk cutaneous squamous cell carcinoma
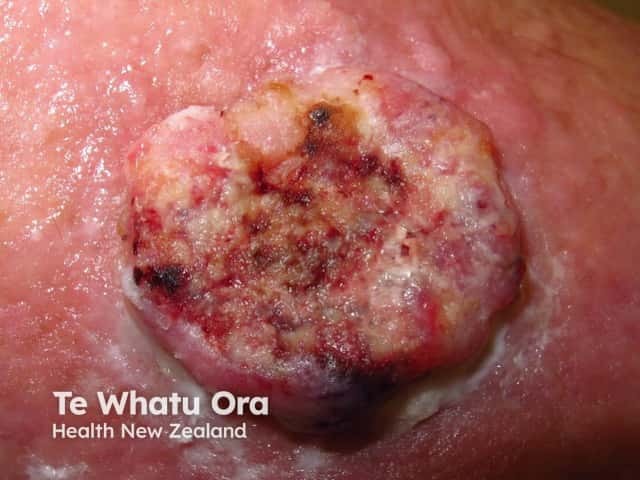
High-risk cutaneous squamous cell carcinoma
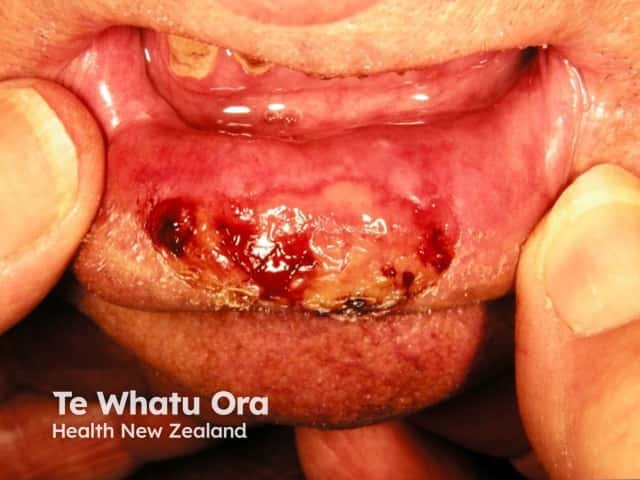
High-risk cutaneous squamous cell carcinoma
Staging cutaneous squamous cell carcinoma
In 2011, the American Joint Committee on Cancer (AJCC) published a new staging systemic for cutaneous SCC for the 7th Edition of the AJCC manual. This evaluates the dimensions of the original primary tumour (T) and its metastases to lymph nodes (N).
Tumour staging for cutaneous SCC
TX: Th Primary tumour cannot be assessed
T0: No evidence of a primary tumour
Tis: Carcinoma in situ
T1: Tumour ≤ 2cm without high-risk features
T2: Tumour ≥ 2cm; or; Tumour ≤ 2 cm with high-risk features
T3: Tumour with the invasion of maxilla, mandible, orbit or temporal bone
T4: Tumour with the invasion of axial or appendicular skeleton or perineural invasion of skull base
Nodal staging for cutaneous SCC
NX: Regional lymph nodes cannot be assessed
N0: No regional lymph node metastasis
N1: Metastasis in one local lymph node ≤ 3cm
N2: Metastasis in one local lymph node ≥ 3cm; or; Metastasis in >1 local lymph node ≤ 6cm
N3: Metastasis in lymph node ≥ 6cm
How is squamous cell carcinoma diagnosed?
Diagnosis of cutaneous SCC is based on clinical features. The diagnosis and histological subtype are confirmed pathologically by diagnostic biopsy or following excision. See squamous cell carcinoma – pathology.
Patients with high-risk SCC may also undergo staging investigations to determine whether it has spread to lymph nodes or elsewhere. These may include:
- Imaging using ultrasound scan, X-rays, CT scans, MRI scans
- Lymph node or other tissue biopsies.
What is the treatment for cutaneous squamous cell carcinoma?
Cutaneous SCC is nearly always treated surgically. Most cases are excised with a 3–10 mm margin of normal tissue around a visible tumour. A flap or skin graft may be needed to repair the defect.
Other methods of removal include:
- Shave, curettage, and electrocautery for low-risk tumours on trunk and limbs
- Aggressive cryotherapy for very small, thin, low-risk tumours
- Mohs micrographic surgery for large facial lesions with indistinct margins or recurrent tumours
- Radiotherapy for an inoperable tumour, patients unsuitable for surgery, or as adjuvant.
What is the treatment for advanced or metastatic squamous cell carcinoma?
Locally advanced primary, recurrent or metastatic SCC requires multidisciplinary consultation. Often a combination of treatments is used.
- Surgery
- Radiotherapy
- Cemiplimab
- Experimental targeted therapy using epidermal growth factor receptor inhibitors
Many thousands of New Zealanders are treated for cutaneous SCC each year, and more than 100 die from their disease.
How can cutaneous squamous cell carcinoma be prevented?
There is a great deal of evidence to show that very careful sun protection at any time of life reduces the number of SCCs. This is particularly important in ageing, sun-damaged, fair skin; in patients that are immune suppressed; and in those who already have actinic keratoses or previous SCC.
- Stay indoors or under the shade in the middle of the day
- Wear covering clothing
- Apply high protection factor SPF50+ broad-spectrum sunscreens generously to exposed skin if outdoors
- Avoid indoor tanning (sun beds, solaria)
Oral nicotinamide (vitamin B3) in a dose of 500 mg twice daily may reduce the number and severity of SCCs in people at high risk.
Patients with multiple squamous cell carcinomas may be prescribed an oral retinoid (acitretin or isotretinoin). These reduce the number of tumours but have some nuisance side effects.
Emerging evidence suggests that standard HPV vaccination may reduce the burden of actinic keratoses in immunocompetent individuals with multiple lesions. This may in turn reduce the incidence of future SCCs.
What is the outlook for cutaneous squamous cell carcinoma?
Most SCCs are cured by treatment. A cure is most likely if treatment is undertaken when the lesion is small. The risk of recurrence or disease-associated death is greater for tumours that are > 20 mm in diameter and/or > 2 mm in thickness at the time of surgical excision.
About 50% of people at high risk of SCC develop a second one within 5 years of the first. They are also at increased risk of other skin cancers, especially melanoma. Regular self-skin examinations and long-term annual skin checks by an experienced health professional are recommended.
References
- Keohane SG, Botting J, Budny PG, et al. British Association of Dermatologists guidelines for the management of people with cutaneous squamous cell carcinoma 2020. Br J Dermatol. 2021;184(3):401–14. doi:10.1111/bjd.19621. Journal
- Parikh SA, Patel VA, Ratner D. Advances in the management of cutaneous squamous cell carcinoma. F1000Prime Reports 2014; 6: 70. doi: 10.12703/P6-70. PubMed Central
- Chahoud J, Semaan A, Chen Y, et al. Association between β-genus human papillomavirus and cutaneous squamous cell carcinoma in immunocompetent individuals-a meta-analysis. JAMA Dermatol. 2016;152(12):1354–64. doi:10.1001/jamadermatol.2015.4530. Journal
- Wenande E, Hastrup A, Wiegell S, et al. Human Papillomavirus Vaccination and Actinic Keratosis Burden: The VAXAK Randomized Clinical Trial. JAMA Dermatol. Published online March 06, 2025. doi:10.1001/jamadermatol.2025.0531. Journal
- Whiteman DC, Thompson BS, Thrift AP, et al. A model to predict the risk of keratinocyte carcinomas. J Invest Dermatol. 2016;136(6):1247–54. doi:10.1016/j.jid.2016.02.008. Journal
- Work Group; Invited Reviewers, Kim JYS, et al. Guidelines of care for the management of cutaneous squamous cell carcinoma. J Am Acad Dermatol. 2018;78(3):560–78. doi:10.1016/j.jaad.2017.10.007. Journal
On DermNet
- Squamous cell carcinoma – pathology
- Squamous cell carcinoma in skin of colour
- Intraepidermal SCC (Bowen disease)
- Vulval intraepithelial neoplasia
- Penile intraepithelial neoplasia
- Bowenoid papulosis
- Vulval cancer
- Oral cancer
- Squamous cell carcinoma — common skin lesions course
- Skin signs of rheumatic disease
- Ultraviolet radiation
- Targeted therapy
- Cemiplimab
Other websites
- Skin cancers and precancers — DermNet e-lecture [Youtube]
- Cancer Council Australia
- Clinical practice guidelines for keratinocyte cancer — Cancer Guidelines wiki
- Head and Neck Squamous Cell Carcinoma — Medscape Reference
- Squamous Cell Carcinoma — British Association of Dermatologists
- Optimal care pathway for people with basal cell carcinoma or squamous cell carcinoma — Cancer Council of Australia, June 2016
- Squamous cell carcinoma — American Academy of Dermatology
- riSCC (risk stratification app for cutaneous SCC) — The Skin Cancer Outcomes Consortium (SCOUT)
