Main menu
Common skin conditions

NEWS
Join DermNet PRO
Read more
Quick links
Author: A/Prof Amanda Oakley, Dermatologist, Hamilton, New Zealand, February 2016.
Introduction Contributing factors Immediate causes Common causes Inflammatory causes
A chronic leg ulcer is defined as full thickness skin loss for > 3 months. At times, it can be difficult to determine the correct diagnosis of a leg ulcer. At least 15% of leg ulcers are of mixed aetiology. It is essential to take a thorough medical history and to examine the patient carefully, looking for local and systemic clues to the diagnosis.
Whatever the primary cause of the ulcer, there are often other factors that contribute to the poor healing of ulcers. These include:
An ulcer often begins with:
Chronic infection can also be responsible for ulceration, particularly:
Infection is identified by swabs and biopsy samples sent for bacterial and fungal microscopy and culture.
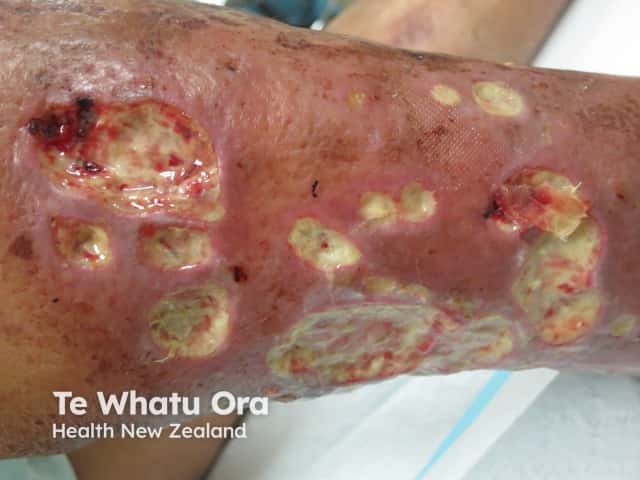
Atypical mycobacteria
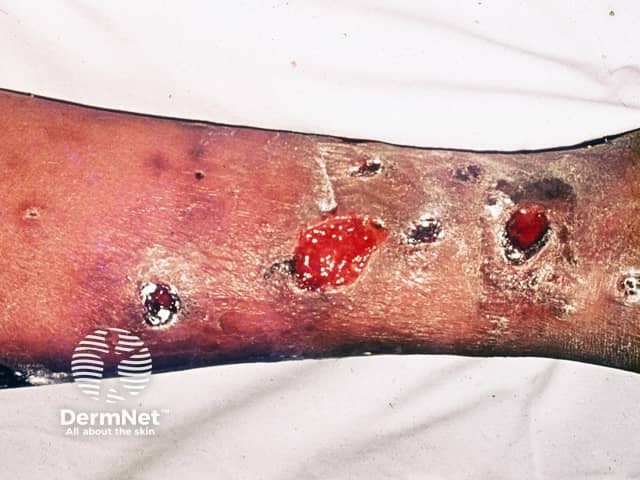
Leprosy
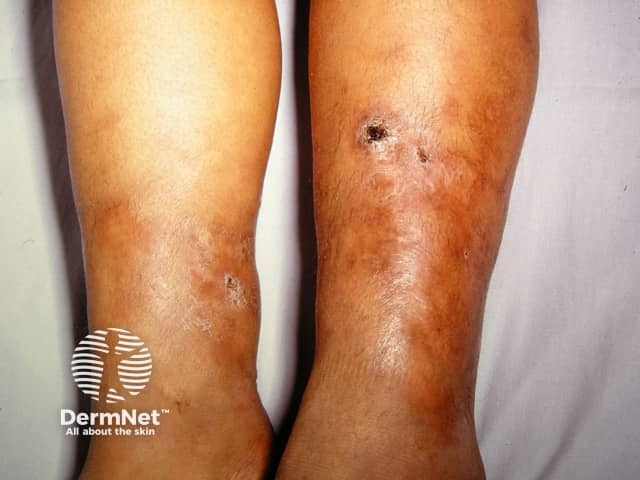
Tuberculosis
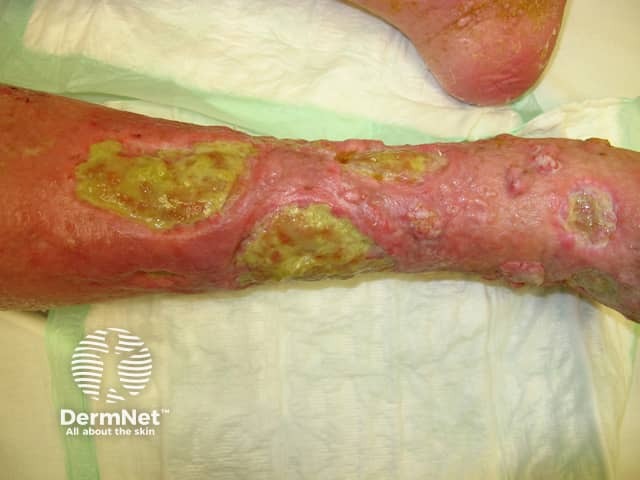
Venous ulceration
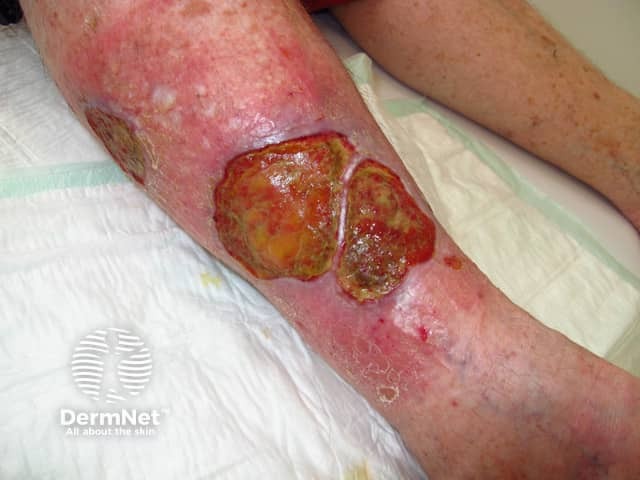
Venous ulceration
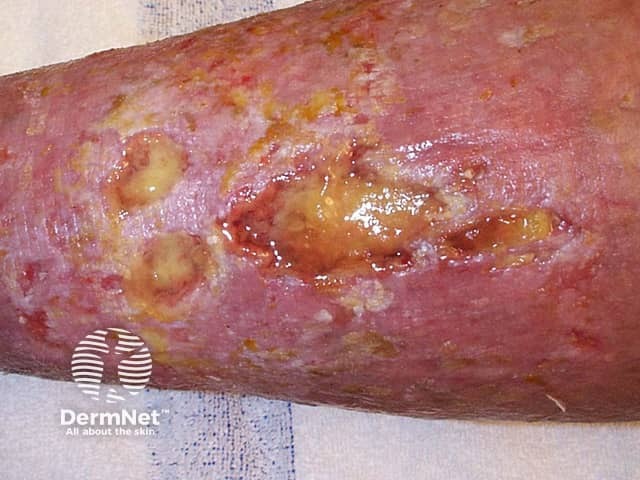
Venous ulceration
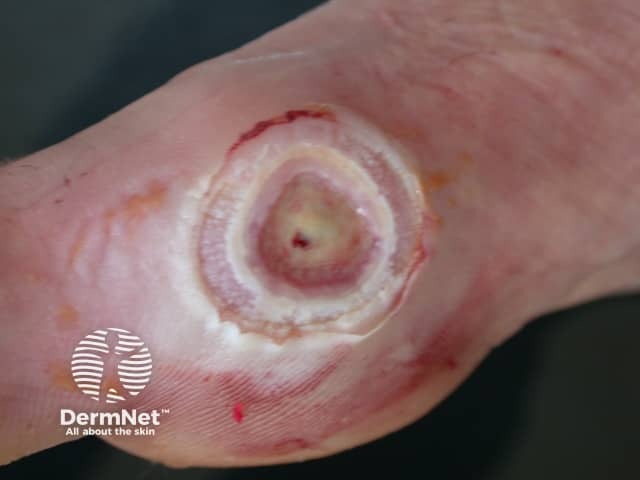
Neuropathic ulcer
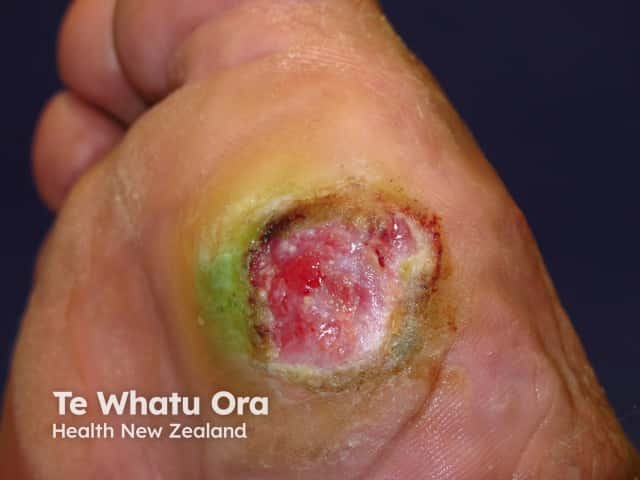
Neuropathic ulcer
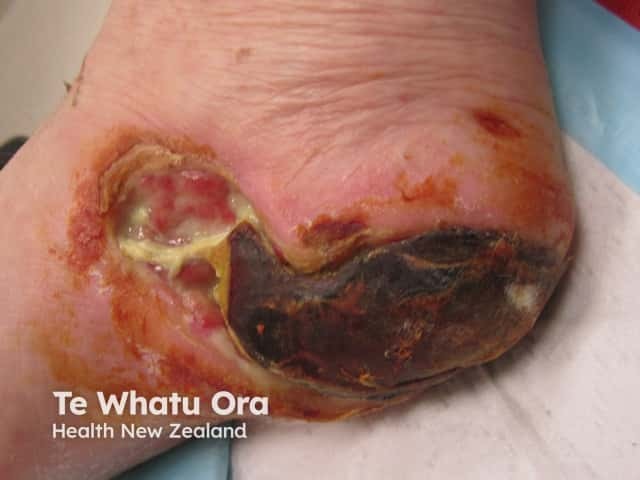
Neuropathic ulcer
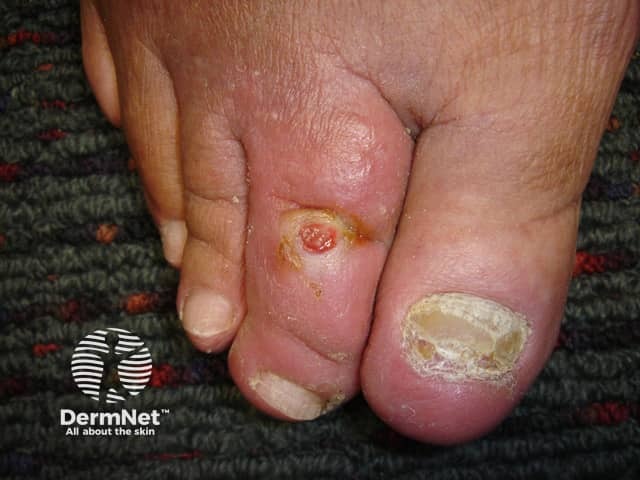
Diabetic ulcer
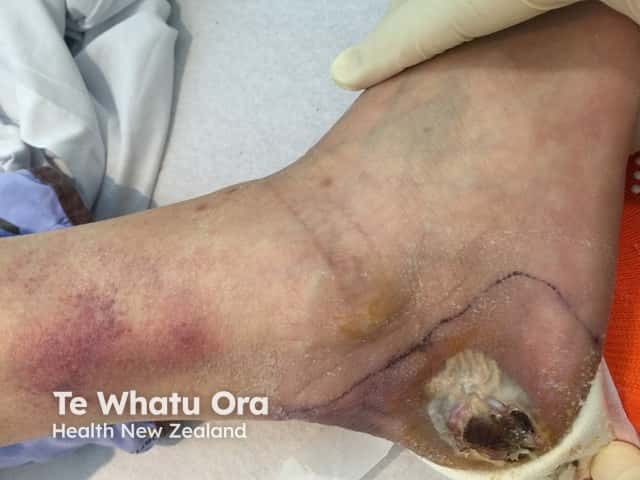
Diabetic ulcer
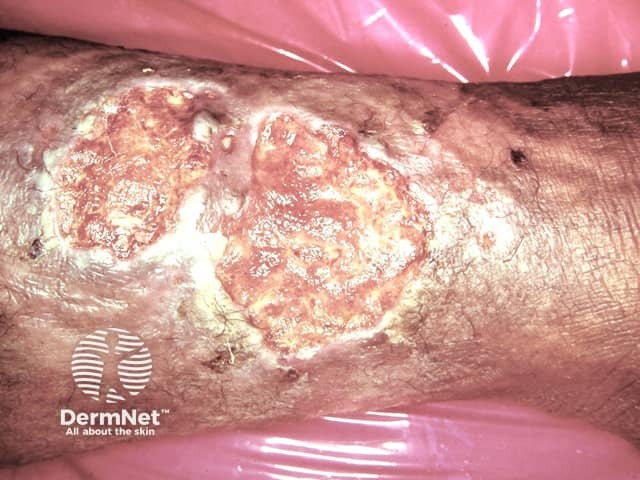
Diabetic ulcer
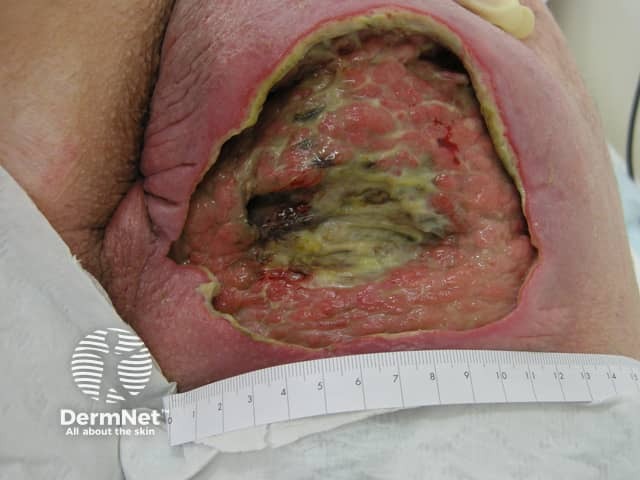
Pressure sore
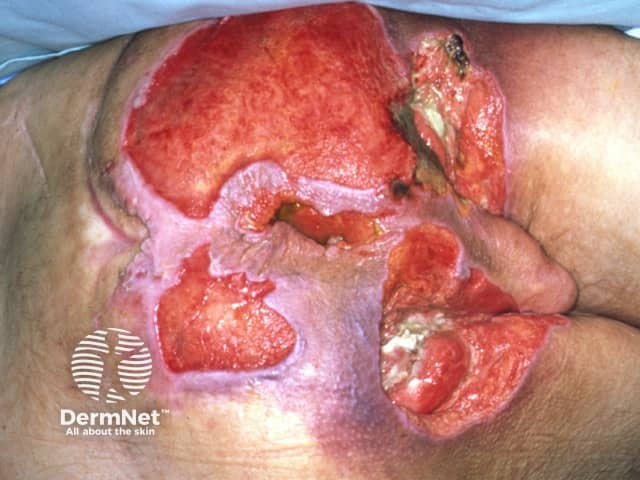
Pressure sore
Pressure sore
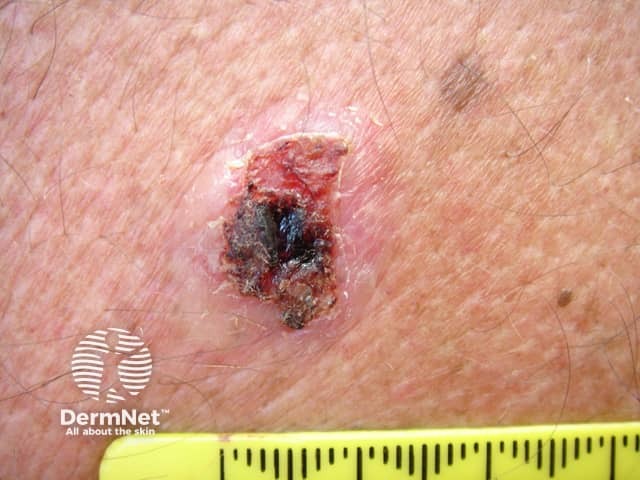
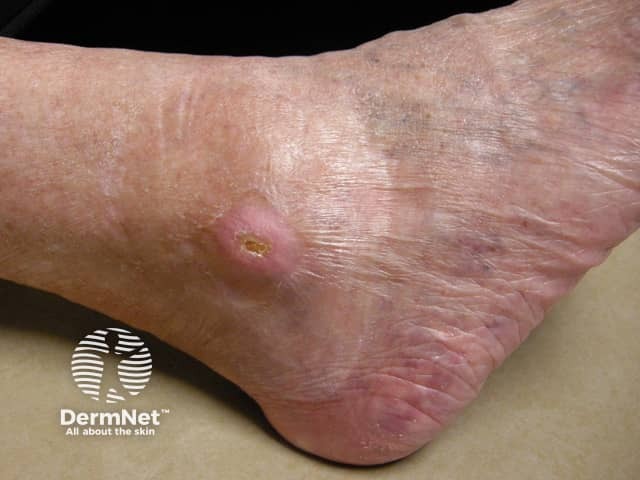
Basal cell carcinoma
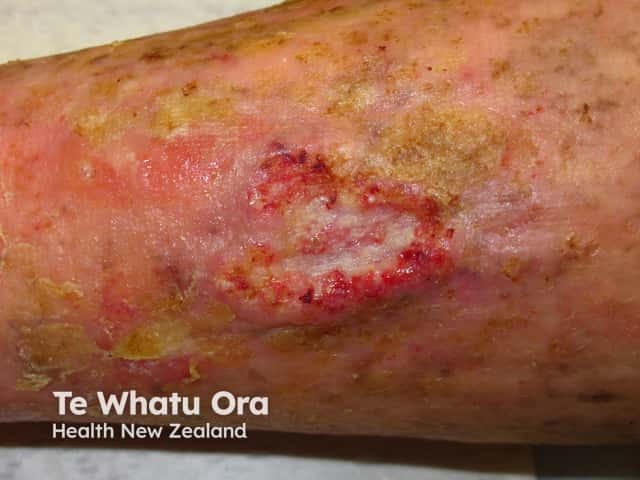
Squamous cell carcinoma
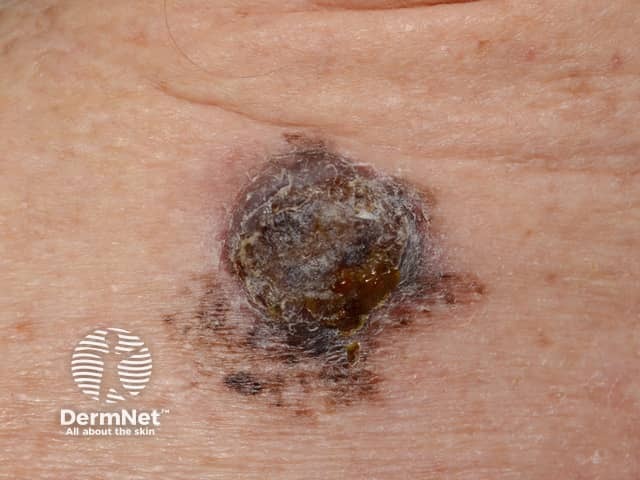
Ulcerated melanoma
Inflammatory causes of leg ulceration can be difficult to diagnose and difficult to treat.
If considering an inflammatory cause of leg ulceration, diagnostic tests may involve:
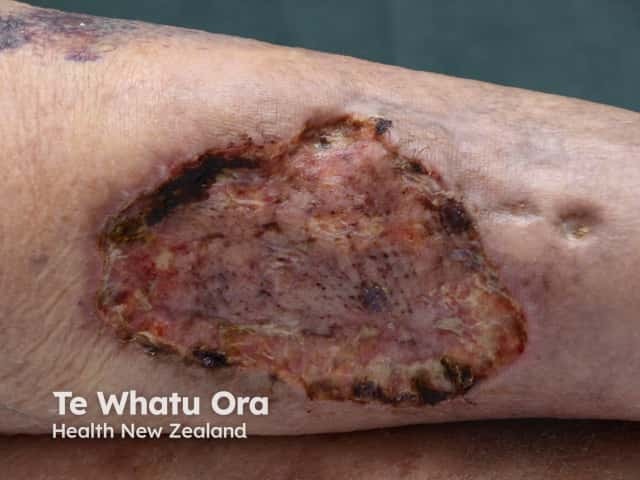
Pyoderma gangrenosum
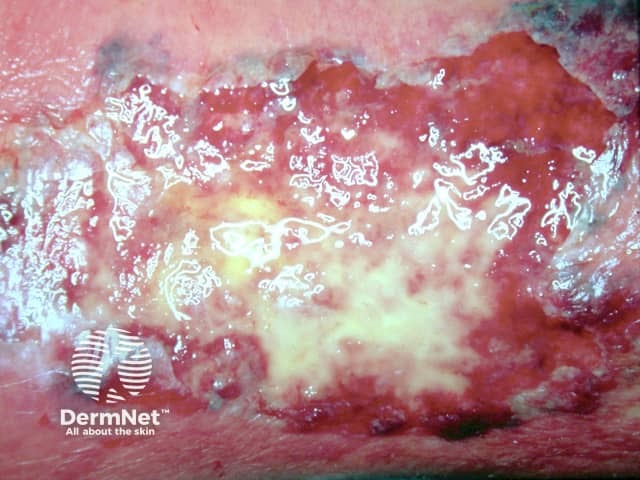
Pyoderma gangrenosum
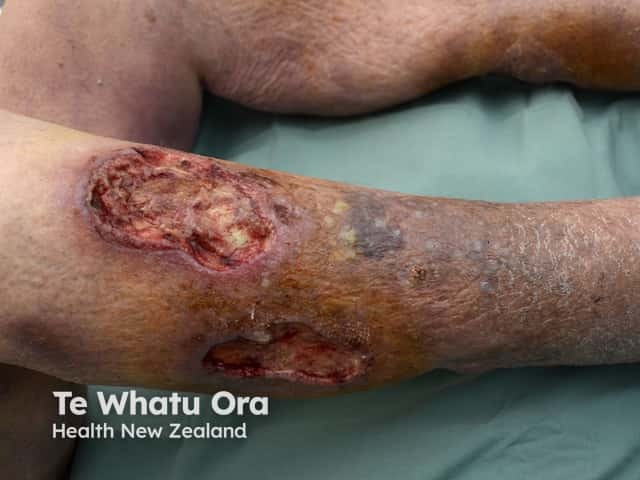
Pyoderma gangrenosum
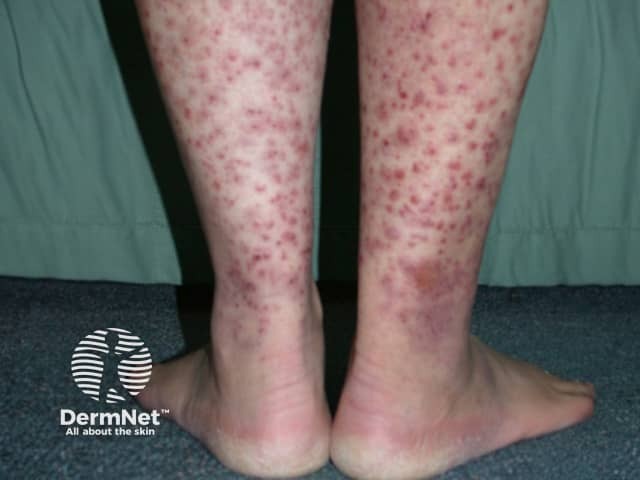
Small vessel vasculitis
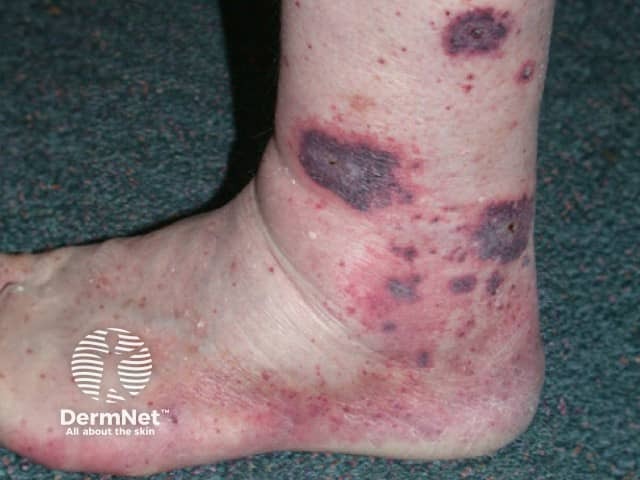
Small vessel vasculitis
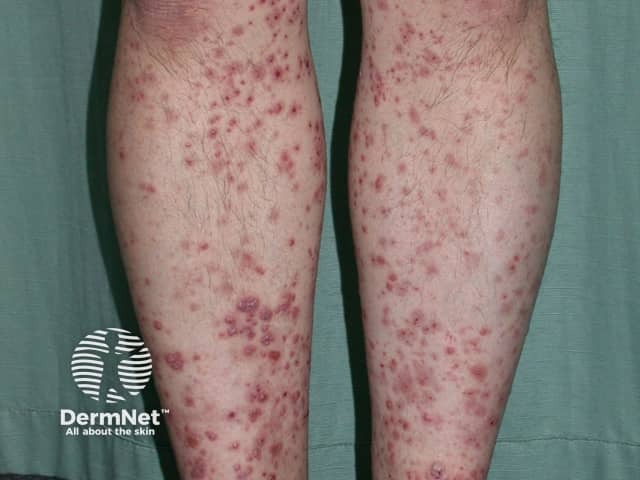
Small vessel vasculitis
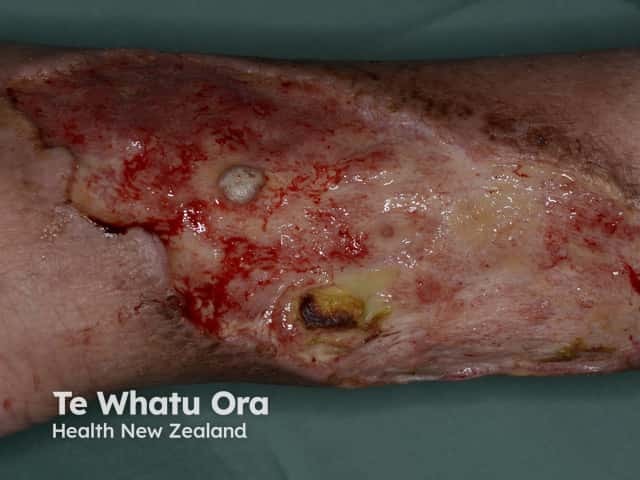
Polyarteritis nodosa
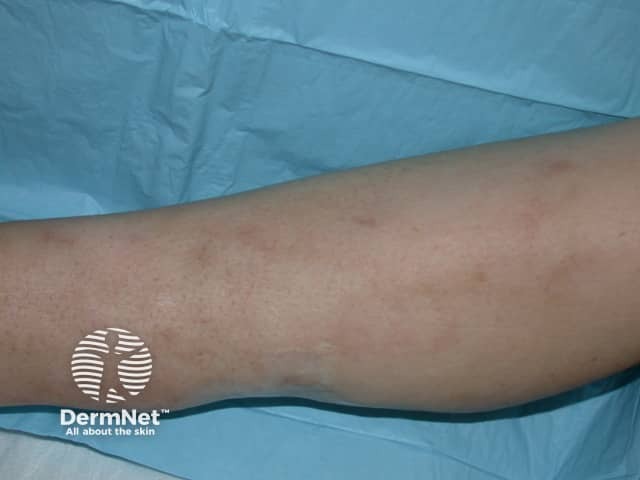
Polyarteritis nodosa
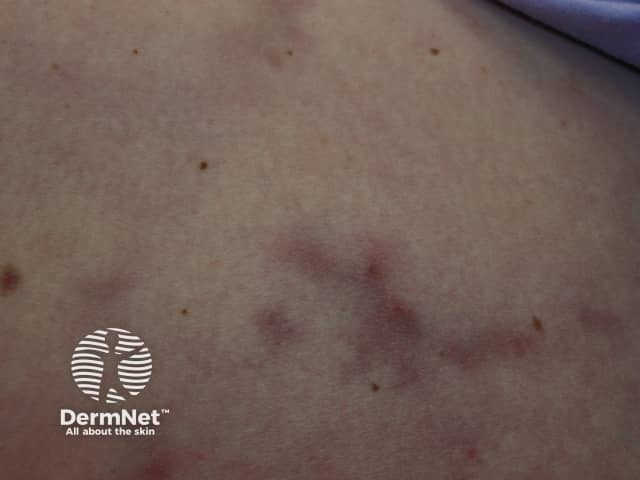
Polyarteritis nodosa
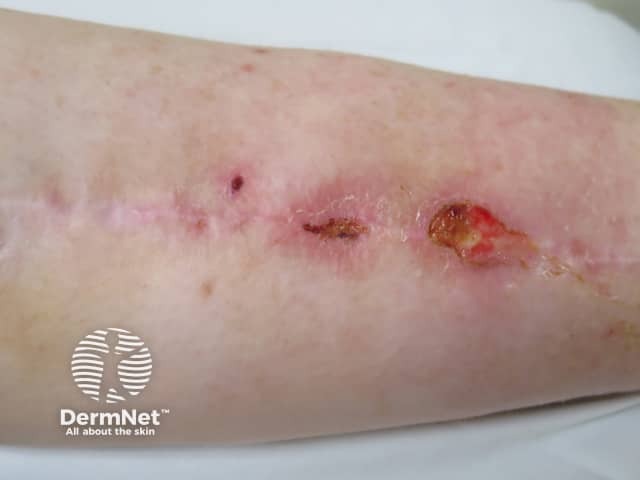
Rheumatoid ulcer
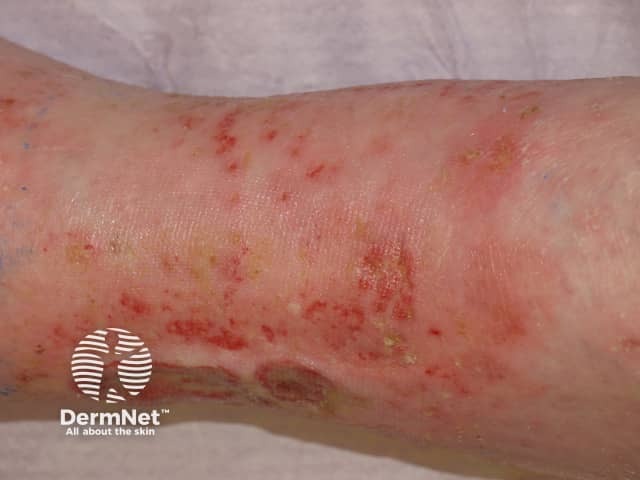
Rheumatoid ulcer
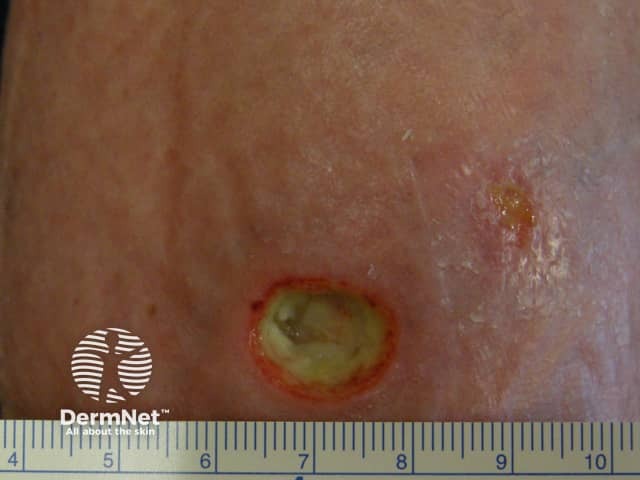
Rheumatoid ulcer
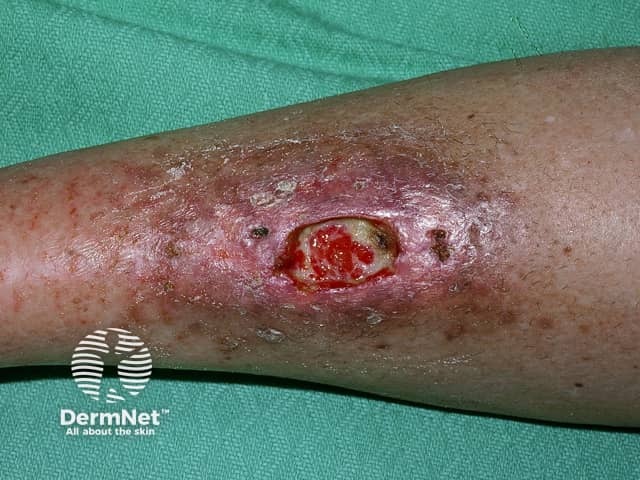
Ulcerated necrobiosis lipoidica
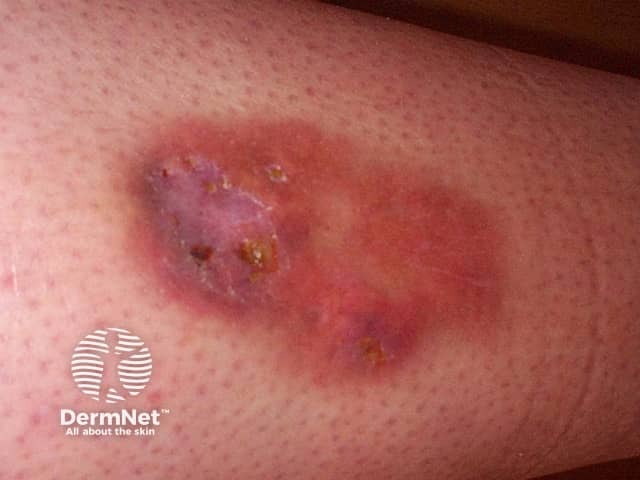
Ulcerated necrobiosis lipoidica
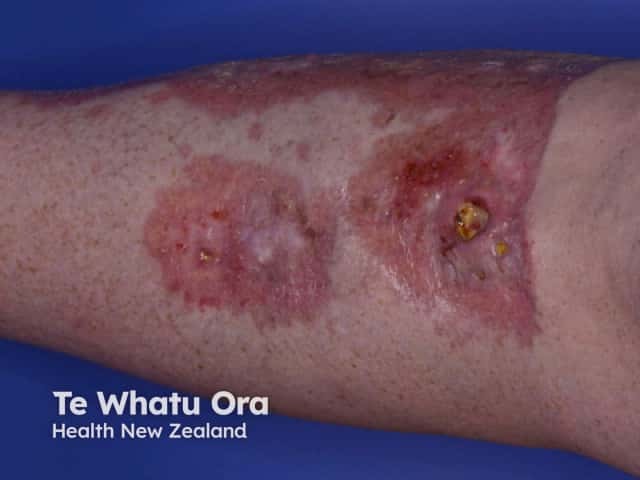
Ulcerated necrobiosis lipoidica
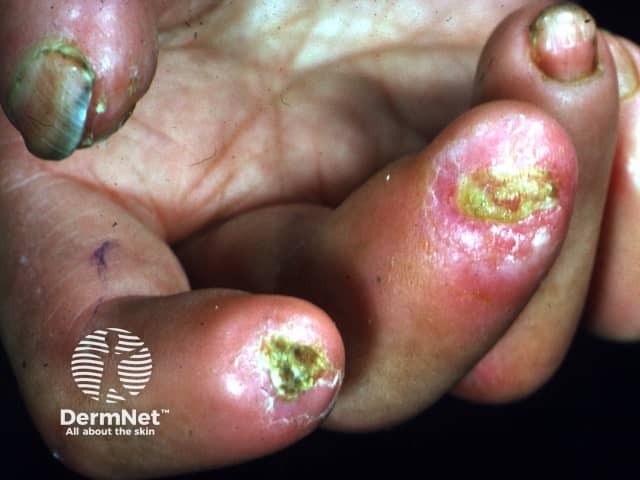
Systemic sclerosis
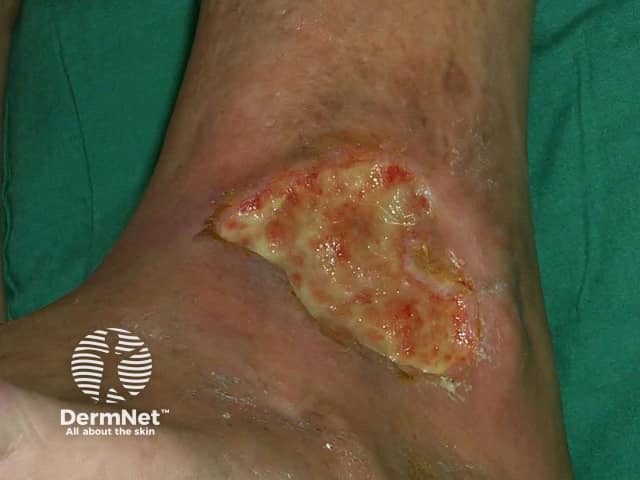
Systemic sclerosis
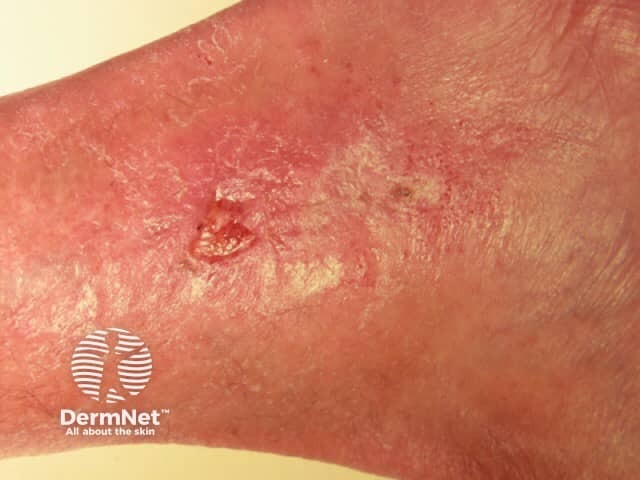
Systemic sclerosis
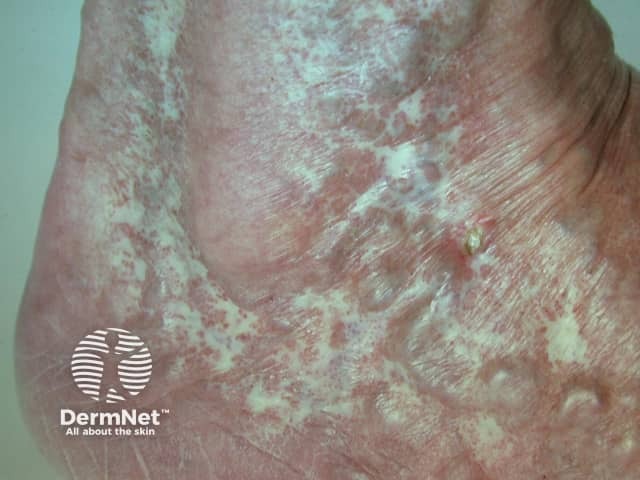
Livedoid vasculopathy
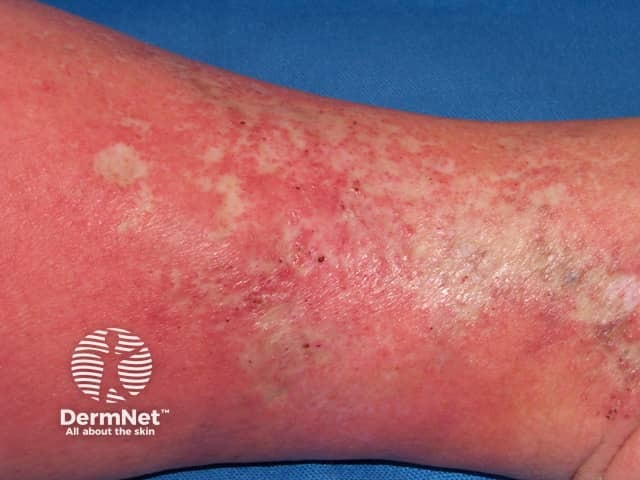
Livedoid vasculopathy
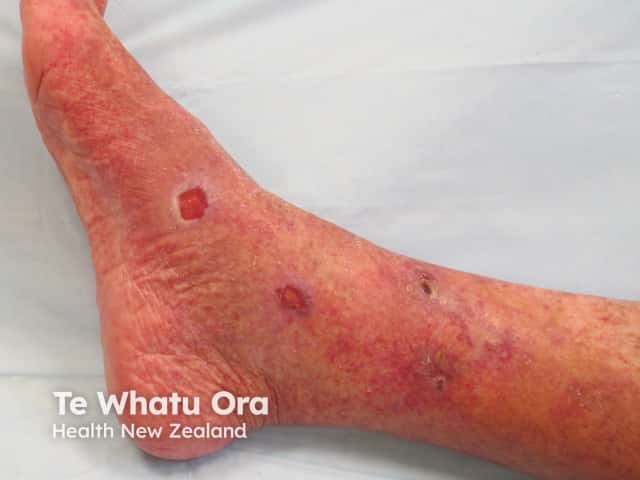
Livedoid vasculopathy
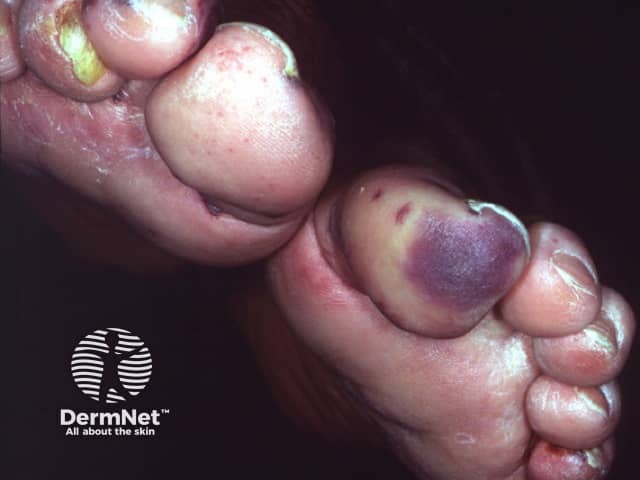
Cholesterol emboli

Cholesterol emboli
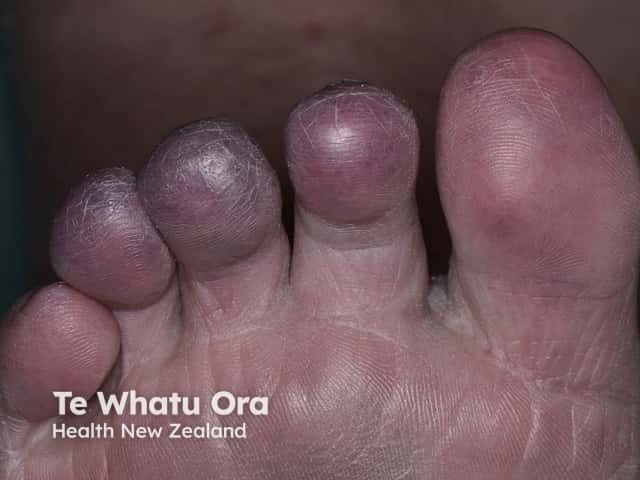
Cholesterol emboli
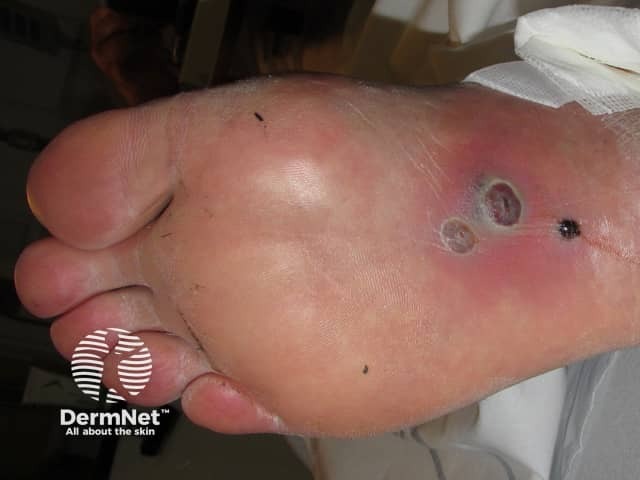
Septic emboli
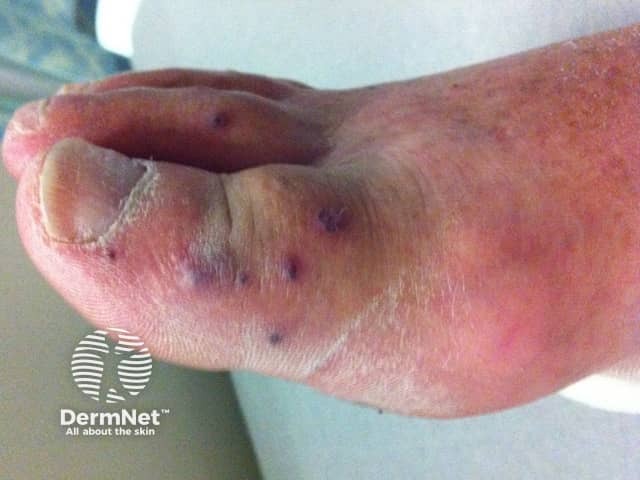
Septic emboli
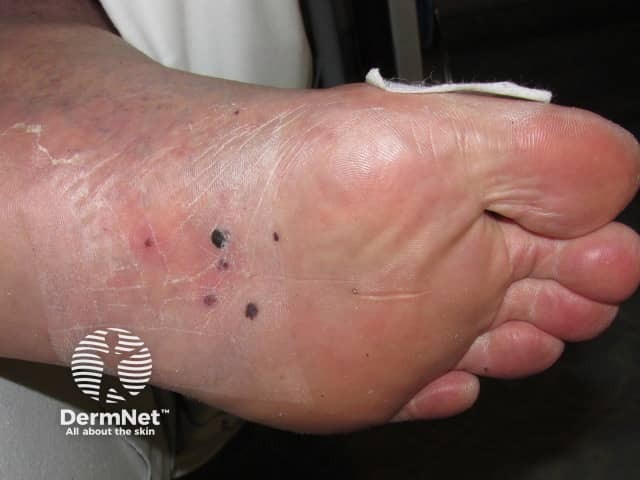
Septic emboli
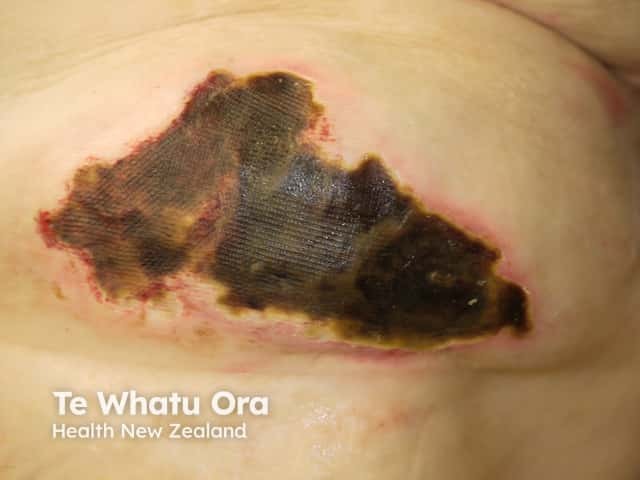
Calciphylaxis
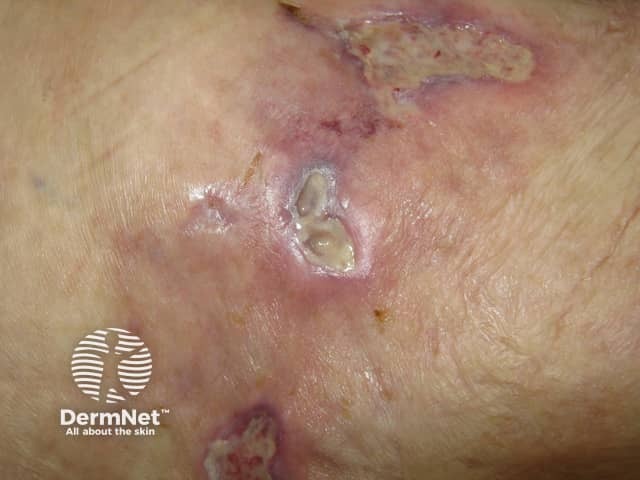
Calciphylaxis
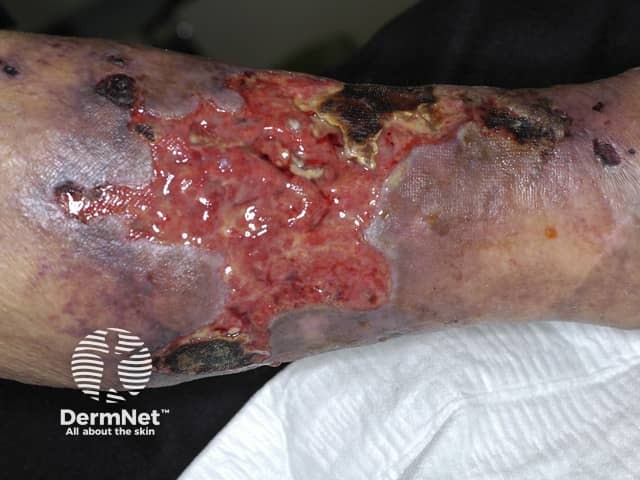
Calciphylaxis
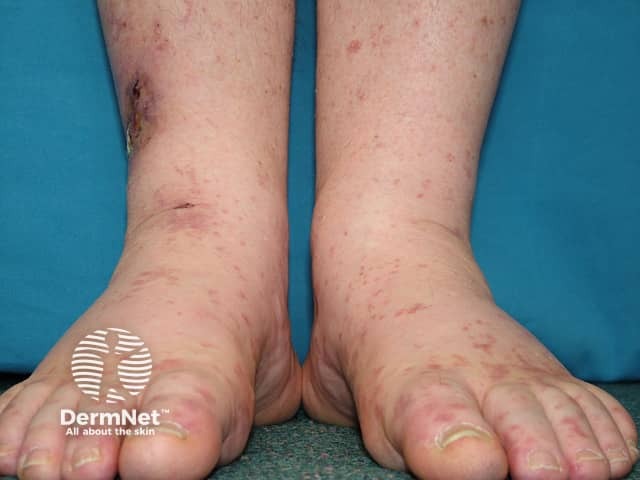
Cryoglobulinaemia
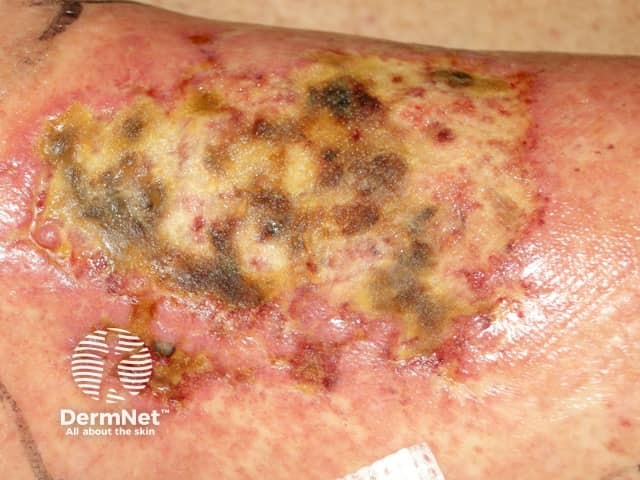
Cryoglobulinaemia
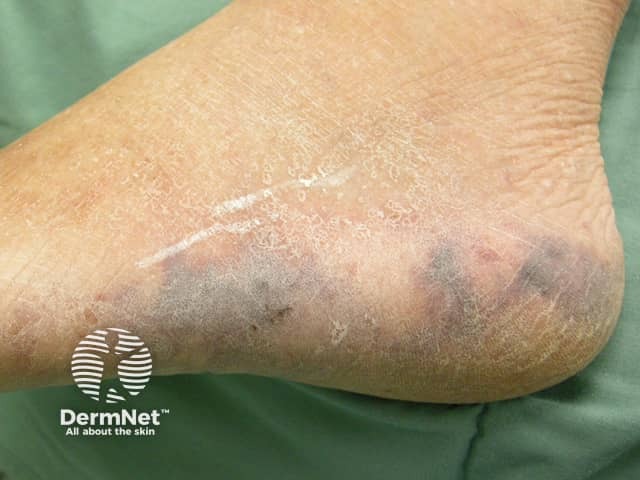
Cryoglobulinaemia
Levamisole-adulterated cocaine can result in a combination of: